Preface
Indian Foods: AAPI’s Guide to Nutrition, Health & Diabetes is a labor of love by a group of dedicated dietitians. This booklet has information which will guide Asian Indians and particularly Indian Americans of Indian origin better manage and prevent diabetes, hypertension, obesity and hyperlipidemia. In addition, this book can be used by physicians and other health care professionals who see patients in their clinic using the Asian Indian cuisine. I believe this book is a must have for all Indian Americans. It is available on the American Association of Physicians of Indian Origin (AAPI) website at www.aapiusa.org/resources. This revision is presented to the Indian American community and physicians as a community service on behalf of AAPI. The reader will find that this edition has a few added chapters and appendices. The two new chapters include “Do Indian Spices and Condiments Have a Role to Play in Preventive Health and Therapeutics” & “Renal Diet.” It is our small effort to help our community take charge to prevent diabetes, hyperlipidemia, and obesity and manage them if present.
With best wishes,

T.G.Patel, MD, MACP
Advisor, Public Health Committee, AAPI
Acknowledgement
The revised edition of the book was done in a timely manner due to Dr. Ranjita Misra’s leadership and coordinating efforts. We would also like to thank Padmini Balagopal as the coordinating editor for the first edition and Rita (Shah) Batheja as co-chair for her invaluable help in bringing together an expert group of contributors.
I want to personally thank the authors Nirmala Abraham, Padmini Balagopal, Chatterjee, Keya Deshpande, Madhu Gadia, Wahida Karmally, Karmeen Kulkar Rita Batheja, Sharmila i, Theja Mahalingaiah, Suraj Mathema, Ranjita Misra, Chhaya Patel, Sudha Raj, Nirmala Ramasubramanian, Janaki Sengupta and Geeta Sikand. These authors took time out of their busy family life, academics and work to revise this edition of the book. To date, this book is still one of the best resources on preventive health and disease management on the Asian Indian cuisine presented in a simple and user friendly format. This book can be downloaded in its entirety from the website www.aapiusa.org/resources/nutrition.aspx for use.
The reviewers Padmini Balagopal, Rita Batheja, Wahida Karmally, Karmeen Kulkarni, Ranjita Misra, T.G.Patel, Sudha Raj and Nirmala Ramasubramanian have done a tremendous job in getting the reviews back in time and in ensuring the accuracy of the material.
The Pocket Reference Card for diabetes was created by the Diabetes Committee of the Indo-US Health Summit, a new additions to this book. I want to thank Drs. Ritesh Gupta, Shashank Joshi, Anoop Misra, T.G.Patel and Banshi Saboo, along with the advisors who helped revise this Pocket Reference Card. This committee consists of Drs. Anuj Bhargava, Arvind Gupta, Neha Gupta, Shilpa Joshi, Sailesh Lodha, Mohan Mallam, Sundar Mudaliar, Rakesh Parikh, V. Ranga, Jayesh B. Shah, Ronak Shah, Priya Sivaprakasan, and Vijay Viswanathan. The Gestational Diabetes meal plan was created by Sharmila Chatterjee, another new addition to this book. I want to thank Padmini Balagopal for creating “What Can I Eat to Manage my Diabetes” and Wahida Karmally and Karmeen Karmally to review the document & the translators of the regional languages (Bengali, Gujarati, Hindi, Kannada, Malayalam, Marathi, Odia, Punjabi, Sindhi, Tamil and Telugu) Rajasri Chatterjee, Kaushik Chatterjee, Sharmila Chatterjee, Alokeraj Banerjee, Balwant Suthar, Rita Batheja, Bharat Shah, Varun Japee, Vanita Manchanda, Uday Meghani, Varsha, Roshan Khaki, Kavitha Simha, Sheela Krishnaswamy, Shaji Tewani, Alex Johnson, Vaishali Mohile Deepa Inamdar, Anita shra, GB Patnaik, Indu Jaiswal, Murali Sadani, Purshotam Sharangdhar, Sushila Sarangdhar, Suguna Lakshmi Narayanan, Anuradha Sivasundar, A Narasimha Reddy, Latha Sashi, N Lakshmi, and P Janaki Srinath.
Finally, I want to thank all the Indian Americans in the U.S. and Indians in India for helping us to assess data on our community by participating in different research projects. This book is a tribute to all Indian Americans and Indians all over.

T.G.Patel, MD, MACP
FORWARD BY AJEET R. SINGHVI, PRESIDENT AAPI



I am pleased to see the publication of the second edition of Indian foods: AAPI’s Guide to Nutrition, Health and Diabetes. The first edition was hugely successful and this edition was overdue and is being published at the right time.
Although there are over two thousand books on diabetes listed in the catalog of the Library of Congress (2,218 at the last count), however, there is a paucity of literature that deals with the largest population at risk: The Indian Population. The ancient Ayurvedic treatises by Sushruta and Charaka recommended diet as treatment for diabetes more than two thousand years ago in India. This is as relevant today, if not more so, as it was then. Further, it is not only of great value to Indians here in States but also to the general population India – especially given the expansion of quick service restaurants and the concomitant adoption of a diet of highly processed, high calorie, high sugar, high fat, but low nutrient value foods.
It will be of special benefit to all to realize that the concept of diet as treatment is centuries old. Through this concept, people will discover new and tasty foods that help manage or even reverse their diabetes and other related conditions.
This publication is truly unique. The contributors include M.D.s, Ph.Ds, and Registered Dietitians. There is a diet plan to suit every palate and for different ethnic groups and regions. The authors have taken into account the changing environment, customs, and preferences and have made modifications to suit all the segments of the population and all taste buds in the contemporary society.
This book makes us all proud. Health is wealth, and this book takes us a step forward in that direction. I am sure it will be very useful to the reader. I personally congratulate Dr TG Patel, Dr. Ranjita Misra and their entire team for this superb effort.
Sincerely,

Ajeet R. Singhvi, MD, FACG
President, AAPI president@aapiusa.org
Chapter 1
Introduction
Sudha Raj, PhD, RD
Since 1965 more than 2 million Asian Indians have immigrated to the United States from the Asian sub- continent of India. Recent census report that their numbers have increased from 1.6 million in 2000 to 2.7 million in 2007. The community continues to be ranked the third largest Asian American group in the United States after Chinese and Filipinos. Fifty percent of Asian Indians reside in the South and West followed by 35% in the north-east and the remainder in the Mid-West. Large Asian Indian communities are seen in the states of California, Illinois, New Jersey, New York and Texas. The community consists of academic, medical and technical professionals, individuals who own and/or work in commercial establishments and their dependents (spouses, children, siblings and elderly parents who visit from India for extended periods of time).
The Asian Indian community is diverse with regard to the region of origin in India and the religions they practice. India can be divided into four major regions-North, South, East and West. Each region has its own distinctive language, dialects, customs and food practices. Hinduism is the predominant religion practiced by Asian Indians followed by Islam, Buddhism, Jainism, Sikhism, Zorastrianism, Christianity and Judaism. The followers of these different religions observe different dietary laws and codes for fasting, and feasting thereby influencing their eating patterns. Throughout history, the culture and cuisines of India have been influenced by other civilizations such as the Moghuls, the British and now the Americans. The neighboring nations of Pakistan, Nepal, Bhutan, Bangladesh and Sri Lanka on all four frontiers share many common features with regard to dietary habits and food practices despite their unique cuisines.
Health problems and nutritional status of Asian Indians in the US
Some of the important health problems faced by Asian Indian immigrants include chronic degenerative diseases such as diabetes, hypertension, cardio-vascular disease and complications arising from any of these conditions. In fact, Asian Indian immigrants have a significantly higher risk of CVD (cardiovascular disease) with heart disease rates estimated to be one and one half to four times greater than Whites. In addition to the genetic susceptibility in developing Type 2 diabetes and cardiovascular disease, risk factors such as abnormal lipid levels, increased abdominal fat, diets high in fat, saturated and trans-fats, simple carbohydrates and sedentary lifestyles contribute to the development of chronic diseases.
What can you do?
Your nourishment does not depend on the selection of any one food. Instead it depends on the consistent and continuous selection of many different foods on a day to day basis. This book gives you suggestions on how to plan your diet with Asian Indian cuisine with foods and tips that will help to enhance your health.
Purpose and organization of this booklet
This book makes an attempt to present some tools for patients and the general public to help with lifestyle changes in the prevention and treatment of chronic diseases. Highlights of this book include:
- A brief description of two chronic degenerative diseases- Diabetes and Cardiovascular disease.
- A description of the different regional cuisines of India. Within each region we provide background information to illuminate the cultural context from which the ethnic foods and food habits have evolved, popular dishes, meal patterns highlighting typical and modified meal patterns for clients with chronic diseases, tips for changes and suggestions for weekend and party planning and tips on how to modify a high-fat recipe into a more heart-healthy one. Every chapter talks about weekend eating as the two days of feasting and partying can undo many of the benefits of eating healthy throughout the week.
- A description of common spices used in the various cuisines and their health benefits.
- A section on food exchanges that gives a list of some of the common foods and selected food items mentioned in the book as well as some of the ingredients in this cuisine with its English equivalent.
- Nutrition advice, tips and guidelines by qualified professionals and reviewers in the field of nutrition (you will find a brief write-up about the writer at the end of each chapter).
A Primer on Chronic Diseases in Asian Indians Diabetes
Diabetes is a chronic disorder characterized by high blood glucose and either insufficient or ineffective insulin, depending on the type of diabetes.
Type 1 diabetes also known as insulin dependent diabetes or juvenile onset diabetes typically strikes around the ages of 8 to 12 years but can occur at any age. The disease has a strong genetic link. The pancreas cannot synthesize insulin thereby altering the body’s metabolism. Insulin is required to assist the cells in taking up the needed fuels from the blood.
Type 2 diabetes is characterized by high blood glucose and insulin resistance. This disease usually begins after the second decade of life. However the widespread changes in lifestyle and dietary practices has resulted in the appearance of this disease at a much younger age. In the initial stages the pancreas produces insulin. The person may actually have higher than average insulin levels but the cells are not very responsive either because they have fewer number or malfunctioning receptors that are needed for the insulin to exert its action. Consequently the blood glucose levels increase thereby stimulating the pancreas to produce insulin. This exhausts the cells and reduces their ability to function. Generalized weight gain particularly in the abdominal region aggravates the condition because the higher body fat necessitates higher insulin production. Age, genetics, lifestyle and dietary factors promote the development of the disease.
Symptoms of Diabetes include frequent urination, excessive thirst, extreme hunger, unusual weight loss, increased fatigue, irritability and blurred vision.
Criteria for diagnosis
- Symptoms of diabetes together with casual (any time of day) plasma glucose concentrations of > 200 mg/dl.
- Fasting plasma glucose (At least 8 hours following no caloric intake) > 126 /dl.
- Two hour plasma glucose > 200 mg/dl during an oral glucose tolerance
Criteria for Impaired Glucose levels
- Fasting plasma glucose levels of > 110mg/dl –
126 mg/dl or post-prandial glucose levels (2 hrs after meals) of > than 140 mg/dl during an oral glucose tolerance test can be considered to be in the Impaired blood glucose range.
Introduction
Body Mass Index and Waist circumference
- A Body Mass Index of ≥23 and Waist circumference of >35.4” for men and 31.5” for women can put a person at risk for developing diabetes if there is a genetic
Blood Pressure - <120/80
HbA1c - <6.5
Complications of diabetes
The accumulation of glucose in the blood leads to acute and chronic complications. Therefore early, aggressive treatment to control blood glucose significantly reduces the risk of long term diabetes related complic-ations. Diabetes related complications include diseases of the:
- large blood vessels such as atherosclerosis
- small blood vessels resulting in loss of kidney function as seen in kidney diseases, retinal degeneration and
- nerves resulting in loss of sensation, increased infections stemming from unnoticed injuries, and gastrointestinal
Recommendations for Type1
Nutrition is an important part of the treatment regimen. Nutritional therapy focuses on maintaining optimal nutrition for growth and development in the child, educating clients about portion sizes, modifying recipes, controlling blood glucose, preventing and treating related complications. Focus is on meal intake patterns, consistency in carbohydrate intake to minimize glucose fluctuations.
Recommendations for Type 2
The American Diabetes Association recomm-ends that the distribution of calories between fats and carbohydrates should be individual-ized according to the individual’s assessment and treatment plan.
- Calories should be prescribed to maintain a reasonable body weight ideal for the person’s age, sex and lifecycle needs.
- Protein intake is recommended at 10-20% of caloric intake with a focus on plant based sources such as lentils and beans, cereal lentil combinations and the use of smaller portions of lean meats, poultry and
- Total fat, saturated fat and cholesterol intakes must be tailored to meet individual requirements based on blood lipid profiles. Focus on healthy fats rather than saturated fats and emphasize avoidance of trans-fats.
- Diet should focus on the consumption of complex carbohydrates such as whole grains, fruits and vegetables. Consistent and evenly spaced carbohydrate intake throughout the day should be emphasized. In this respect carbohydrate counting and exchange lists provided in this book will
- Current guidelines advise moderation of salt intake that is < 1500 mg. of sodium/day and no more than 2300 mg. of sodium/day.
Metabolic Syndrome
Metabolic syndrome is a condition closely related to insulin resistance. Abdominal obesity and insulin resistance aggravate the disease along with hypertension and abnormal lipid levels.
Diagnostic criteria put out by the International Diabetes Federation include a waist circumference of > 90 cms for men and 80 cms for women; a triglyceride level of >150 mg/dl; a HDL-cholesterol level of < 40 mg/dl for men and <50 mg/dl for women; a blood pressure of > 130/85 mm HG and a fasting plasma glucose of >100 mg/dl or previously diagnosed type 2 Diabetes.
Cardiovascular disease
More than 50% of cardiovascular disease occurrences arise from atherosclerosis. Atherosclerosis is a generic term used to describe the thickening of the arteries caused by the formation and deposition of an atherosclerotic plaque. The plaque is a fatty fibrous growth that
Indian Foods: AAPI's Guide to Nutrition, Health and Diabetes
ultimately becomes calcified and contributes to the blocking of the arterial blood vessel. This results in poor or restrictive blood flow contributing to the rise in blood pressure or hypertension, myocardial infarction and stroke. Associated conditions include peripheral vascular disease resulting from the plaque formation in the leg and congestive heart failure that impairs normal cardiac function. Major risk factors for cardiovascular disease include age, gender, family history, abnormal lipid profiles such as low HDL and high LDL cholesterol, hypertension, diabetes, obesity and physical inactivity, cigarette smoking and an “atherogenic diet” high in saturated fat, trans fats, cholesterol, processed foods and low in fruits and vegetables. Recommendations for reducing your risk for cardiovascular disease include:
- Regular screening for abnormal lipid profiles such as a high LDL and low HDL levels as well as monitoring of blood
- seeking help from a trained nutrition professional (To find a registered dietitian (RD) in your area visit eatright.org Click on the “Find a Nutrition Professional” link toward top of the page). A dietitian can help you focus on therapeutic lifestyle changes such as increasing physical activity (regular exercise of more than thirty minutes every day), quitting smoking, alcohol consumption in moderation, stress reduction, dietary modifications such as moderating total and saturated fat intake, replacing saturated fats with desirable polyunsaturated fats; increasing the use of plant based diets with minimal amounts of animal products and paying attention to the sodium content of the diet.
Sudha Raj PhD RD is a Senior Part-time Instructor in the Department of Nutrition Science & Dietetics in the College for Human Ecology at Syracuse University in Syracuse, New York. Contact information 315-443-2556 or sraj@syr.edu
References
- http://www.theheart.org/article/1112435.do (Accessed 1, 2011)
- http://factfinder.census.gov 2007- (Accessed Feb. 1, 2011)
- Nelms M, Sucher K and Long S. Nutrition Therapy and Pathophysiology. Thomson Higher Education.
- Misra A. et al. South Asian diets and insulin resistance. J Nutr. 2009 101, 465-473.
- American Diabetes Association. Diagnosis and Classification of diabetes mellitus. Diabetes Care, 29 (Supplement 1) S43-48,
- American Diabetes Association. Standards of medical care in diabetes. Diabetes Care. (Supplement 1): S4
- Jonnalagadda SS, Khosla P. Nutrient intake, body composition, blood cholesterol and glucose levels among adult Asian Indians in the United States. J. Immigr. Minority Health 2007 Jul; 9(3):171-8.
- Enas EA et al. Recommendations of the second Indo-US health summit on prevention and control of cardio-vascular disease among Asian Indians. Indian Heart 61(3): 265-74. 2009
Resource for Diabetes Education Material
- yourdiabetesinfo.org
- Two Reasons I Find Time to Prevent Diabetes: My Future and Theirs (in Gujarati)
- http://ndep.nih.gov/media/GujaratiTipsheet.pdf
- Two Reasons I Find Time to Prevent Diabetes: My Future and Theirs (Hindi)
- http://ndep.nih.gov/media/HindiTipsheet.pdf
- 4 Steps to Control Your Diabetes. For Life. (in Gujarati)
- http://ndep.nih.gov/publications/PublicationDet aspx?PubId=135
Introduction
- 4 Steps to Control Your Diabetes. For Life. (in Hindi)
- http://ndep.nih.gov/publications/PublicationDet aspx?PubId=141
- Take Care of Your Heart. Manage Your Diabetes (in Gujarati)
- http://ndep.nih.gov/media/TCH_AsAm_flyer_ pdf
- Take Care of Your Heart. Manage Your Diabetes (in Hindi)
- http://ndep.nih.gov/media/TCH_AsAm_flyer_ pdf
- If You Have Diabetes, Know Your Blood Sugar Numbers
- http://ndep.nih.gov/media/KnowNumbers_Eng. pdf
- Tips to Help You Stay Healthy
- http://ndep.nih.gov/media/TipsFeel_Eng.pdf
- Tips for Kids: How to Lower Your Risk for Type 2 Diabetes
- http://ndep.nih.gov/media/kids-tips-lower- pdf
- Diabetes Numbers at-a-Glance
- http://ndep.nih.gov/media/NumAtGlance_Eng. pdf
- The Power to Control Diabetes is in Your Hands Community Outreach Kit
- http://ndep.nih.gov/publications/OnlineVersion.aspx?NdepId=NDEP-44k
- Tips for Teens with Diabetes: Stay at a Healthy Weight
- http://ndep.nih.gov/media/Youth_Tips_Weight.pdf
- Tips for Teens with Diabetes: Make Healthy Food Choices
- http://ndep.nih.gov/media/Youth_Tips_Eat.pdf
- It's Not Too Late to Prevent Diabetes
- http://ndep.nih.gov/media/nottoolate_tips.pdf
- Kanaya AM et al. Prevalence and correlates of diabetes in South Asian Indians in the United States: findings from the metabolic syndrome and atherosclerosis in South Asians living in America study and the Multi-ethnic study of atherosclerosis. Metab. Syndro. Relat. Disorders. Apr 8 (2): 157-64.
- Palaniappan L et Leading causes of mortality of Asian Indians in California. Ethnic Dis. 20 (1): 53-7 Winter 2010.
Chapter 2
Epidemiology, Risks, and Complications of Type 2 Diabetes Mellitus
Ranjita Misra, PhD, CHES, FMALRC & TG Patel, MD, MACP
The prevalence (all cases) and incidence (new cases) of type 2 diabetes (T2DM) and pre-diabetes [as defined by impaired fasting glucose (IFG) or impaired glucose tolerance (IGT)] are rapidly increasing both in developed and developing countries. The global burden of T2DM is more pronounced in India than any other country in the world. An estimated 57 million adult Indians will have diabetes by 2025, with the condition manifesting at an earlier age and lower body mass index. Although, the higher prevalence of T2DM in Asian Indians can be attributable to established causes such as growing levels of obesity and physical inactivity, various epidemiological studies have shown that these factors alone are not sufficient to explain this trend. One important factor contributing to increased prevalence of T2DM in Asian Indians is excessive insulin resistance. Insulin resistance is highly prevalent in Asian Indians despite low rates of obesity. While insulin resistance is very complex and not completely understood, this pathophysiologic abnorm-ality results in decreased glucose transport in muscle, elevated hepatic glucose production, and increased breakdown of fat resulting in hyperglycemia. Indians seem to have a genetic predisposition towards insulin resistance with a low BMI and high central adiposity, sometimes also known as the ‘Yudkin-Yajnik’ paradox. This increased genetic susceptibility is further enhanced by environmental triggers such as physical inactivity, excessive calorie intake, and obesity.
The main etiological (causal) risk factors for T2DM are older age, obesity, family history, physical inactivity and dietary factors such as a high proportion of energy consumed as saturated fat and low intake of fruit and vegetables. The rapid rise and epidemiological transition of T2DM in India, especially in urban areas, is associated with westernized lifestyle. Changes in the traditional lifestyles, dietary patterns and technological advancement have resulted in a pronounced physical inactivity and the affluence of society has lead to consumption of diets rich in fat, sugar and calories. The observation of an association between low birth weight and risk of diabetes in later life has also led to the development of an alternative to the thrifty genotype hypothesis. It is hypothesized that the risk of T2DM is programmed by fetal nutrition and the pattern of early growth. The causal nature of these associations is strengthened by studies that show the incidence of diabetes is reduced by interventions aimed at reducing weight, increasing activity and improving diet.
With more than a billion people India is also home to significantly diverse groups of people in terms of ethnicity, caste and religion, socioeconomic status, educational level, and lifestyle and food habits. Studies on prevalence of T2DM show the rates in rural areas is significantly lower (3-6%) as compared
Epidemiology, Risks, and Complications of Type 2 Diabetes Mellitus
to urban areas (8-14%) in India. Pre-diabetes rates are slightly higher than T2DM prevalence but follow a similar pattern with urban prevalence significantly greater than the rural populations. Although prevalence of T2DM is lower than urban areas, rural Indians have higher glycosylated hemoglobin level (A1c) or poor control of the disease resulting in higher complications and mortality. Community- based diabetes prevention program in a rural Indian community also found rural youths, 10-18 years of age, had higher level of pre-diabetes. Lack of knowledge of T2DM and its associated complications, access to care & medical services, low educational level and income are primary factors for elevated mortality of diabetic patients in rural India.
Studies on South Asians (includes Asian Indians, Pakistanis, Bangladeshis, Sri Lankans, Nepalese, Maldives, and Bhutan) immigrants in the United Kingdom, Canada, Australia, and Africa show a higher prevalence of T2DM and CVD as well. In the United States, the Diabetes among Indian Americans (DIA) national study showed prevalence rate of T2DM and pre-diabetes among immigrant Asian Indians as 17.4% and 33% respectively, higher than other racial/ethnic groups in the United States.
Table 1: Prevalence of diabetes among rural Indians, urban Indians and Indian Americans
|
|
Fasting Blood Glucose Levels |
A1c Levels |
|||||||
|
US Site |
Number of cases |
Mean |
SD |
Mean |
SD |
< 8.0 |
≥ 8.0 |
||
|
Self-reported Diagnosed T2DM cases |
145 |
137.03 |
42.73 |
6.84 |
1.30 |
84.4% |
15.6% |
||
|
Undiagnosed cases |
36 |
156.03 |
35.58 |
7.28 |
1.35 |
80.6% |
19.4% |
||
|
Total number of respondent = 1038; Prevalence of Diabetes = 17.44%; Prevalence of Pre-diabetes = 32.9% |
|||||||||
|
Urban India |
Number of cases |
Mean |
SD |
Mean |
SD |
< 8.0 |
≥ 8.0 |
||
|
Self-reported Diagnosed T2DM cases |
57 |
134.10 |
47.68 |
6.85 |
1.22 |
79.4% |
20.6% |
||
|
Undiagnosed cases |
12 |
152.17 |
43.52 |
7.11 |
0.69 |
83.4% |
16.6% |
||
|
Total number of respondent = 508; Prevalence of Diabetes = 13.6%; Prevalence of Pre-diabetes = 23.4% |
|||||||||
|
Rural India |
Number of cases |
Mean |
SD |
Mean |
SD |
< 8.0 |
≥ 8.0 |
||
|
Self-reported Diagnosed T2DM cases |
35 |
137.03 |
42.73 |
6.84 |
1.30 |
84.4% |
15.6% |
||
|
Undiagnosed cases |
13 |
235.77 |
185.36 |
7.28 |
1.35 |
80.6% |
19.4% |
||
|
Total number of respondents = 532; Prevalence of Diabetes = 9.02%; Prevalence of Pre-diabetes = 13.1% |
|||||||||
Indian Foods: AAPI's Guide to Nutrition, Health and Diabetes
In the same study, comparison of rural Indians, urban Indians and immigrant Asian Indians in the US showed rural Indians had the lowest rate followed by urban Indians and immigrants in the US (Table 1). Despite a perception that they have high socio-economic status and good access to health care, US Asian Indians have marked variations in educational attainment, income, and wealth, and a significant number lack education and job skills. Recent immigrant cohorts comprise both highly educated professionals as well as individuals who lack education and job skills. The latter are mostly family members of earlier immigrants.
T2DM Complications: A focus on Diabetes and Cardiovascular Disease
T2DM is one of the leading causes of morbidity and mortality because of its role in the development of optic, renal, neuropathic, and cardiovascular disease. These complications, particularly cardiovascular disease (~50-75% of medical expenditures), are the major sources of expenses for patients with T2DM [for more information, please read the chapter on “Preventing Heart Disease in Asian Indians” and “Cardiovascular disease” in the introduction chapter]. In the United States, South Asian Indians have the highest ethnic-specific prevalence of CVD or coronary artery disease (CAD), with age-specific mortality two to three times higher than Caucasians. Results from the DIA study indicate traditional risk factors such as hypertension (21%), obesity (49.8%) and hypercholesterolemia (43.5%) may account for these high rates. Asian Indian immigrants have been found to have high rates of vascular disease in the United States and other countries. The CAD prevalence in US Asian Indians is 6 and 4 times higher than Chinese and other Asian Americans and associated with similarly higher prevalence of risk factors among this ethnic group. For example, the prevalence of central obesity, glucose intolerance, hypertension, high triglyceride levels, and low levels of high density lipoprotein cholesterol (HDL)-- the five ‘axes of evil’ of metabolic syndrome-- is the highest among the Asian Indians and continues to increase at a rapid pace. Mortality from CAD is twice in Indian Americans than other racial/ethnic groups in the United States. The United Kingdom Prospective Diabetes Study, showed for each 1% increase in A1c, there was a 14% increase in incidence fatal or nonfatal myocardial infarction. Projections based on the Global Burden of Disease study have shown that by the year 2020, the overall burden of cardiovascular disease in India will surpass other regions of the world. There is no doubt that significant reduction in diabetes related morbidity and mortality is feasible through effective educational and lifestyle interventions to reduce smoking, promote regular exercise, monitor healthy dietary habits and reading food labels, and manage stress.
Epidemiology of Nutrition and Diabetes Mellitus: Etiology and Environmental Factors
There is considerable evidence to show as individuals migrate from resource poor rural settings to urban areas and westernized countries such as the United States and United Kingdom, the risk and prevalence for T2DM rises. This increase is due to rapid acculturation associated with the migration. Although the concept of acculturation originated within anthropology, in recent years it has assumed a prominent role within epidemiology as a risk factor for chronic disease. The association between acculturation to a Western lifestyle and prevalence of diabetes has been established in several Asian American subgroups due to changes in diet, obesity and other lifestyle factors modulating the prevalence of T2DM. Consumption of sugar-sweetened drinks increases the risk for obesity and predisposes to T2DM. Recent data suggests an increase in the consumption of high fructose corn syrup and association between obesity and T2DM in the US. Glycemic index, or GI, is a number between 0 and 100 that reflects the effects of carbohydrates from food on an individual’s glucose levels. Glycemic index is important for individuals with T2DM since higher GI will increase sugar levels. Foods rich in dietary fiber might be protective and vegetarian diets tend to have less saturated fat and high dietary fiber.
Epidemiology, Risks, and Complications of Type 2 Diabetes Mellitus
Saturated fatty acids are positively related to fasting and postprandial glucose levels in normoglycemic Dutch men, the effect being independent of energy intake and obesity. In the United States, studies show the relative risk of developing diabetes was significantly reduced amongst those with the highest intake of vegetable fats and fiber. While light to moderate intake of alcohol is associated with enhanced insulin sensitivity, smoking increases the risk for T2DM. Intervention trials indicate diet and exercise programs are associated with reduction (nearly 60%) in the risk of progression of pre- diabetes to T2DM. Diets restricted in saturated fatty acids and increased fiber content seems to be particularly successful in this context. Furthermore, weight loss is beneficial and reduces the risk for T2DM.
Conclusions
Asian Indians are disproportionately burdened by T2DM and related complications. Increased genetic susceptibility may be enhanced by environmental triggers such as physical inactivity, high calorie, fat, and sugar intake, and obesity as individuals migrate from rural areas to urban areas to Westernized countries. Acculturation, defined as the process of adopting the cultural traits and social patterns, and western lifestyle are associated with unhealthy habits such as increased intake of dietary fat and saturated fat, lower consumption of fiber-rich and low glycemic index foods, and physical inactivity. These unhealthy behaviors are associated with higher risk and prevalence of T2DM and diabetes-related complications.
Ranjita Misra, PhD, CHES, FMALRC is a Professor and Research Director, Center for the Study of Health Disparities, at Texas A&M University. She is also a member of the Intercollegiate Faculty of Nutrition at TAMU and a member of the Public Health Committee of AAPI. Contact information (979) 845-8726 or ranjitamisra@gmail.com.
TG Patel, MD, MACP is an Associate Professor of Medicine at the Uniformed Services University of the Health Sciences, Bethesda, MD. Contact information (571)213-5393 or thakorg@gmail.com.
References
1. van Dieren S, Beulens JW, van der Schouw YT, Grobbee DE , Neal B. The global burden of diabetes and its complications: an emerging pandemic. Eur J Cardiovasc Prev Rehabil;17 Suppl 1:S3-8.
2. Wild S, Roglic G, Green A, Sicree R , King H. Global prevalence of diabetes: estimates for the year 2000 and projections for 2030. Diabetes Care 2004;27:1047-53.
3. King H, Aubert RE , Herman WH. Global burden of diabetes, 1995-2025: prevalence, numerical estimates, and projections. Diabetes Care 1998;21:1414-31.
4. Ramachandran A, Snehalatha C, Baskar AD, Mary S, Kumar CK, Selvam S et al. Temporal changes in prevalence of diabetes and impaired glucose tolerance associated with lifestyle transition occurring in the rural population in India. Diabetologia 2004;47:860-5.
5. Gupta R, Sarna M, Thanvi J, Sharma V , Gupta VP. Fasting glucose and cardiovascular risk factors in an urban population. J Assoc Physicians India 2007;55:705-9.
6. Mohan V , Deepa R. Risk factors for coronary artery disease in Indians. J Assoc Physicians India 2004;52:95-7.
7. Misra R, Patel T, Kotha P, Raji A, Ganda O, Banerji M et al. Prevalence of diabetes, metabolic syndrome, and cardiovascular risk factors in US Asian Indians: results from a national study. J Diabetes Complications; 24:145-53.
8. Gupta R. Predictors of health among Indians in United States. India Association of North Texas, Texas Indo American Physicians Society Meeting. Dallas, TX,2000.Indian Foods: AAPI's Guide to Nutrition, Health and Diabetes
9. Rangaswamy P. Asian Indians in Chicago: Growth and Change in a Model Minority. In: I.M. G. H. P. Jones editor. Ethnic Chicago. Chicago: Wm. B.Eerdmans Publishing Co; 1995.
10. Wild SH, Laws A, Fortmann SP, Varady AN , Byrne CD. Mortality from coronary heart disease and stroke for six ethnic groups in California, 1985 to 1990. Ann Epidemiol 1995;5:432-9.
11. Enas EA, Garg A, Davidson MA, Nair VM, Huet BA , Yusuf S. Coronary heart disease and its risk factors in first-generation immigrant Asian Indians to the United States of America. Indian Heart J 1996;48:343-53.
12. Enas A AS. Coronary Artery Disease In Asian Indians: An Update And Review. The Internet Journal of Cardiology 2001;1.
13. Deedwania P, Singh V. Coronary artery disease in South Asians: evolving strategies for treatment and prevention. Indian Heart J 2005;57:617-31.
14. Fernandez ML. Acculturation and biomarkers for type 2 diabetes in Latinos. J Nutr 2007;137:871-2.
15. Colditz GA, Manson JE, Stampfer MJ, Rosner B, Willett WC , Speizer FE. Diet and risk of clinical diabetes in women. Am J Clin Nutr 1992;55:1018-23.
16. Fung TT, Hu FB, Pereira MA, Liu S, Stampfer MJ, Colditz GA et al. Whole-grain intake and the risk of type 2 diabetes: a prospective study in men. Am J Clin Nutr 2002;76:535-40.
17. Facchini F, Chen YD, Hollenbeck CB , Reaven GM. Relationship between resistance to insulin- mediated glucose uptake, urinary uric acid clearance, and plasma uric acid concentration. Jama 1991;266:3008-11.
18. Balagopal, P., Kamalamma, N., Patel, T. G., & Misra, R. (2008). A community-based diabetes prevention and management education program in a rural village in India. Diabetes Care, 31(6), 1097-1104.
Chapter 3
Preventing Heart Disease in Asian Indians: Diet & Lifestyle Recommendations
Geeta Sikand,MA,RD,FADA,CDE,CLS
Prevention of heart disease among Asian Indians or South Asians (including Bangladesh, Nepal, Pakistan and Sri Lanka) is a major concern. The occurrence of heart disease among Asian Indians is significantly higher worldwide. According to a recent World Bank Report, heart disease is the leading cause of death in Asian Indian adults (ages 15 to 69 years). All South Asian countries and India in particular are facing a "health crisis" with rising rates of heart disease, diabete. obesity, unhealthy diet and low level of physical activity. The report has also predicted that if the treatable risk factors e.g. excess body Weight, blood pressure and LDL cholesterol remain untreated; it could lead to a global epidemic of heart disease in low and middle income countries.
By 2030 heart disease will emerge as the primary cause of death (36%) in India. A recent study of 52 countries showed that Asian Indians or South Asians suffer their first heart attack six years earlier (53 years versus 59 years) than other countries worldwide.
Heart disease is also the leading cause of death in women in every major developed country e.g. US and also in most emerging economies. The myth that heart disease is only a "man's disease" has been debunked.
What is Heart Disease?
Heart disease refers to diseases of the heart and the blood vessels due to atherosclerosis.Atherosclerosis begins with the deposition of cholesterol filled cells in the inner wall of blood vessels. Due to inflammation, a plaque is formed in the blood vessels. A plaque is a thickened wall of the artery. A damaged plaque can cause a blood clot with very rapid narrowing or blockage of the artery. A heart attack occurs when the blood flow to a part of the heart is blocked (often by a blood clot). Your diet and other lifestyle choices ccm affect your blood cholesterol and triglyceride levels. The good news is that heart disease can be prevented and treated with current knowledge. At the conclusion of this chapter a nutshell or six strategies geared towards how Asian Indian can adopt a heart-healthy diet, will be provided. The same strategies will be helpful for the treatment or high LDL, high triglycerides and the metabolic syndrome.
Risk Factors for Heart Disease
Risk factors increase the chances of a person developing atherosclerosis is and heart disease. According to the National Cholesterol Education Program (NCEP) Adult Treatment Panel III guidelines, the major risk factors for heart disease are:
- Cigarette smoking
- Diabetes mellitus (fasting plasma glucose equal to or greater than 126 mg/do
- Hypertension (Blood Pressure equal To or greater than 140/90 mmHg)
- High LDL cholesterol (equal to or greater than 100)
- Low HDL cholesterol (men less than 40mg/do, women less than 50)
- Obesity (Body Mass Index greater than 25)
- Lack of physical activity
- Family history of premature heart disease(presence of heart diseases in male first-degree relative less than 55 years & in female first degree relative less than 65 years)
- Age (men greater than 1.5 years; women greater than 55 years)
Indian Foods: AAPI'S Guide to Nutrition,Health and Diabetes
Additional risk factors
Your physician will determine whether you need these additional tests.
- Lipoprotein (a),
- Remnant lipoproteins
- Small LDL particles
- Fibrinogen
- High-sensitivity C-reactive protein (CRP)
- Impaired fasting plasma glucose(110- 125mg/di)
- Presence of subclinical atherosclerosis (measured by exercise testing, carotid intimal-medial thickness [CT scan],and/or coronary calcium [EBCT].
Presence of diabetes doubles the risk of heart disease in men and quadruples the risk in women. Lack of healthy dietary habits and a lack of physical activity along with being overweight increase the risk of heart disease,diabetes,high blood pressure and stroke.Asian Indians have a higher prevalence of high triglycerides, low high density lipoprotein (good cholesterol) levels, glucose intolerance, and central obesity. Metabolic syndrome or pre-diabetes is also common in Asian Indians. Some adults as well as children are also at a higher risk for developing heart disease associated with high LDL cholesterol(bad cholesterol)and high triglycerides due to overweight and diets high in fat and refined sugars. Genetic factors also play a role in heart disease.
Target Numbers for Asian Indians to Prevent Heart Disease
- Non HDL-Cholesterol less (Total Cholesterol-HDL= Non HDl- Cholesterol)
- LDL-Cholesterol less than 100 mg/dl
- Blood pressure. less than 40/80 mm
- Waist Circumference. less than 35" for men and less than 31" for women
Target Numbers for Asian Indians with Heart Disease or Diabetes
- Non-HDL-Cholesterol less than 100 mg/dl
- LDL-Cholesterol less than70 mg/dl
- HDL-Cholesterol greater than 40mg/dl for males and greater than 50 mg/dl for females
- HbA1c less than 6.5
- Blood pressure 120/80 mm if you are a diabetic
- Waist circumference less than 35" for men and less than 31" for women
It is important to achieve the target numbers as noted above. If any of your numbers are abnormal, the information provided in this chapter will help you understand the role or a heart healthy diet and lifestyle in preventing heart disease. This chapter also provides six practical strategies geared towards the Asian Indian cuisine. It is also important to seek your physician's advice, lake medications tmder medical suspension so as to reach your target numbers. A registered dietitian (RD) could also partner with you to help you achieve your target numbers. To find a registered dietitian (RD) in your area: www.eatright.org Click on the "Find a Nutrition Professional" link toward top of the page.
Preventing Heart Disease in Asian indians: Diet &Lifestyle Recommendations
What is HDL cholesterol
High-density lipoprotein is a part of the total cholesterol measurement. It is often referred to as "good" cholesterol. The recommended level for men with diabetes is greater than 40mg/dl and for women with diabetes is greater than 50 mg/dl.
What is LDL cholesterol
Low-density lipoprotein is a part of the total cholesterol in the blood. It is often referred to as "bad" cholesterol. LDL should be less than 70mg/dl for those with diabetes and/or heart disease.
Dietary Recommendations to reduce LDL (bad) cholesterol level
The National Cholesterol Education Program Adult Treatment Panel III recommends:
- Adjust caloric intake to achieve and maintain a healthy weight. Weight gain raises LDL (bad) cholesterol and triglyceride levels in the blood.
- Choose a diet low in saturated fat (less than 7% of caloric intake), trans-fat (less than 1 % of caloric intake) and dietary cholesterol (less than 200 mg/day) by consuming a diet high in fish (especially fatty fish), non-fat dairy products,small amounts of lean meat and/or lean meatalternatives e.g. dry beans e.g. rajma,channa,soybeans (like edamame), lentils (daal) and tofu.
- Include food sources of plant sterols & stanols. At the recommended dosage of 2 gm per day, plant sterols reduce cholesterol absorption in the intestine by up to 30% cu1d reduce LDL ``bad" cholesterol by 10%. Plant sterols have the same chemical structure as animal cholesterol which blocks the absorption of cholesterol eaten in the diet as well as cholesterol manufactured by the liver.
- Increase intake of viscous (soluble) fiber to 7-l3g daily e.g. oats, fruits such as strawberries, apples, vegetables such as okra, eggplant, brussel sprouts and legumes such as lentils. Soluble fiber can lower LDL cholesterol 3-5%.
It is recommended that adults eat 21 to 38 grams of total fiber daily.
Diet & Lifestyle Recommendations for Heart Health
A heart healthy diet includes fish (if religion pennits), fruits, vegetables, fiber, low-fat dairy products and low in salt and saturated fat. This dietary pattern is recommended for lowering LDL (bad) cholesterol and blood pressure when accompanied by regular physical activity and weight loss (if overweight). Regular physical activity at a moderate-intensity level for at least 30 minutes on most days of the week helps make your heart stronger and can help manage your weight.
- Enjoy your food, but eat less. Avoid oversized portions.
- Maintain a healthy weight or a BMI, (body mass index) of less than 23. Waist circumference should not exceed 35" in Asian Indian men and 31" in Asian-lndian women.
Make half your plate fruits & vegetables.
Switch to fat free or low fat milk (1%). Reduce calories from solid fats and added sugars (So FAS) and choose foods high in potassium, dietary fiber, calcium, and vitamin D.
Reduce salt by comparing sodium in foods e.g. soup, bread & frozen meals & choose foods with lower numbers.
- Drink water instead of sweetened beverages.
- Regular physical activity can also help you manage your cholesterol by raising your "good" HDL levels and lowering your triglyceride levels.
Source: 2010 US Dietary Guidelines (www.dietaryguidelince.gov)
Summary of a Heart Healthy Diet Pattern based on 2000 Calories per Day
- Fruits and vegetables. 4.5 cups daily (one serving= 1 cup raw leafy vegetable, V2 cup raw or cooked vegetable,½ cup vegetable juice;1 medium fruit, ½ cup fresh fruit).
Indian Foods AAPI's Guide to Nutrition, Health and ½ Diabetes
- Fish: 2 servings per week if religion permits ( 1 serving= 4 oz cooked fish preferably fatty fish e.g. salmon, mackerel, catfish).
- Legumes or lentils. Vegetarians: 5-7 times per week e.g. lentils, daal, rajma, channa and for non-Vegetarian;ms: at least 2 times per week (one serving=½ cup cooked legumes or lentils)
- Whole grains 3 serving per day choose from 1 slice whole grain bread, 1 OL dry whole grain cereal, ½ cup cooked whole grain brown rice,½ cup whole grain pasta, 1-6" chapati.
- Fiber 30 g daily (choose legumes, vegetables, fruits, whole grain, oats, rye, bran cereal, berrie , brown rice etc); 7 to 13 t,rrn soluble fiber e.g. whole oats, rye, barley.
- Nonfat Dairy Products. 2 to 3 servings per day (choose from 1 cup non fat or 1% milk, non-fat yogurt, 1% buttermilk),
- Fats & oils. 4. to 6 tsp daily (choc monounsaturated or polyunsaturated oils e.g. canola, corn, olive, soybean, safflower oil)
- Nuts and seeds. 2 to 4 times per week (½ cup or 1 1/2 oL nuts, avoid macadamia nuts and salted nuts, 2 tablespoon or ½ oz eecb).
- Sugar: limit to 5 servings week ( 1 servmg=1 tablespoon sugar, jelly or jam)
- Saturated fat 7%/total energy intake ( fat on meat or chicken skin, packaged desserts, whole milk, ice cream, huller, cheee, sour cream etc.
- Tran-fatty acid 0 gram (found in processed food., e.g. cookie , chip, Indian savory snack and fried foods).
- Cholesterol. limit to 200 mg daily (found in animal meats, organ meats, egg, etc).
- Alcohol. if you drink it is recommended you limit lo 1 serving per day (women) and 2 serving per clay (men). (1 serving= 5 oz "1ne, 12 oz beer, 1.5 oz of 80-proof spirits, or 1 oz of 100-proof pirils))
- Sodium: 1500 mg per day (read food labels, prepare food with as little salt as possible).
What is the metabolic syndrome?
Metabolic syndrome is the primary cause of an increase in heart disease in Asian Indians.. The American Heart Association and the National Heart, Lung, and Blood Institute recommend that the metabolic syndrome be identified as the presence of three or more of these components:
- Central obesity measured by' elevated waist circumference 1n Asian Indians Waist circumference in Asian Indians greater than 35" Asian Indian Women: greater than 31"
- High triglyceride.Equal to or greater than 1.50mg/el
Reduced HDL (''good'') cholesterol.
Men -Less than ,to mg/dl
Women - Less than 50 mg/dl- High blood pressure. equal to or greater than 130/85 mm Hg
- High fasting glucose 100 lo 125 mg/dl(pre diabetes)
Other components of the metabolic syndrome (insulin resistance and prothrombotic state) cannot be identified by routine clinical evaluation . However, in the presence of central obesity, they can be assumed to be presento some degree.
Metabolic Syndrome Treatment Recommendations by American Heart Association
The primary goal of treating the metabolic syndrome is to reduce the risk for heart disease and type 2 diabetes. Combining a heart healthy diet pattern and regular physical activity with even a small amount of weight loss (7-10%) in overweight people can reverse the metabolic syndrome. The primary approach is to reduce the major risk factors for cardiovascular disease: stop smoking and reduce LDL cholesterol, blood pressure and glucose levels to the recommended levels by:
Preventing Heart Disease in Asian indians: Diet & Lifestyle Recommendations
- Weight loss to achieve a desirable body weight (BMI less than 25 kg/m2)
- Increased physical activity with a goal of at least 30 minutes of moderate-intensity activity on most days of the week. Seek your physician's approval before starting your exercise program.
- Healthful eating habits that include reduced intake of salt, saturated fat e.g. butter, ghee,conut, coconut oil and coconut milk, palm oil, fatty meats, Trans fat e.g. vanaspati (Dalda), partially hydrogenated oils used in Indian savory snacks and dietary cholesterol e.g. egg yolks, meat, dairy.
What are triglycerides?
Triglycerides are a type of fat found in the blood. If triglycerides levels are high, they can increase the risk of heart disease. Triglycerides are stored in the fat cells. When caloric intake is excessive, the additional calories are converted into triglycerides (fat) and stored in fat cells. This is how the body stores its body fat. Take your triglyceride number seriously. Extremely high triglyceride (1000 or higher) can cause pancreatitis (inflammation of the pancreas). Several risk factors can increase the risk for very high triglycerides:
- Overweight / obesity
- Lack of exercise
- High LDL(bad)cholesterol and low HDL(good)cholesterol
- Type 2 diabetes
- Certain medications
- Family history
Table 1: National Cholesterol Education Program
(NCEP) cut points for normal to very high
triglyceride levels
| Noraml | Less than 150mg/dL |
| Borderline-high | 150-199 mg/dL |
| High | 200-499 mg/dL |
| Very High | 500mg/dL or higher |
Blood levels of triglycerides are measured in the fasting state after a 12-hour fast and no alcohol for 48hours before the blood test
To lower triglycerides
The National Cholesterol Education Program's Adult Treatment Panel III recommends:
- Weight loss of 7 to 10% of body weight should be encouraged if indicated.
- Avoid excessive intake of carbohydrate (not more than 50% of calories) especially refined carbohydrates e.g. sugar and sweets
- Choose fats Wisely and lower the intake of fat to not more than 35% of calories in the diet.
- Eat plenty of vegetables, fruits and whole grain, non-fat milk and non -fat dairy products, choose fatty fish, lean meat and lean meat alternatives e.g. tofu, soybcam lentils and legumes
- Abstain or limit alcohol intake according to your doctor's instructions
- Include regular physical activity such as walking for a minimum of 30 minutes on most days of the week.
Are fats & oils bad for a heart healthy diet?
All fats and oils are high in calories and can cause weight gain when excessive calories are consumed. However, some fats are good for heart health provided their calorie contribution does not cause weight gain. Fats are divided into 3 types based on the main type of fat they contain.
1. Unsaturated fats
Unsaturated fats are liquid at room temperature and are generally considered "good fats" such as omega- 3 (marine and plant derived), monounsaturated and polyunsaturated fats (omega-6).
Marine Derived Omega-3 fatty acids
Marine derived Omega-3 fatty acids found in fatty fish e.g. salmon are considered as "good fats" for
Indian Foods: AAPI's Guide to Nutrition, Health and Diabetes
two reasons. Firstly, they can lower the risk of heart disease and secondly lower triglycerides. Two servings (3.5 oz each) of fatty fish per week are associated with a 30-40% reduced risk of death from a heart attack or stroke in persons without heart disease. Fatty fish are a good source of omega-3 fatty acids e.g. eicosapentanoic acid (EPA) and dexahexanoic acid (DHA). If religion permits it is important to consume fatty fish. Good sources of marine omega -3 fatty acids:
- Salmon, farmed or wild
- Mackerel
- Herring
- Sardines
Methyl Mercury concerns from eating· fish
Limit eating large fish due to greater mercury content such as:
- - Swordfish
- - King mackerel
- - Albacore tuna
- - Shark
- - Tile fish
It is advisable for pregnant women and young children to avoid eating these fish according to the United States Food and Drug Administration /Environmental Protection Agency.
Plant derived Omega-3 fatty acids
Plants can also be a source of omega-3 fatty acids primarily alpha-linolenic acid (ALA). However, very small amounts of ALA convert to EPA and DHA.
Two to three grams/day of ALA may reduce risk of heart disease. Good sources of ALA (plant omega-3) are:
- Canola oil 1TBS = 0.94 g/senring
- Ground flax seeds 1TBS-1.6 g/serving
- Flaxseed oil 1TBS=7.3 g/serving
- English walnuts 1 TBS (7 halves) - 2.6 g/serving
- Soybean oil 1 TBS 0.94 g/serving
- Chia seeds (sabza) 1 tsp = 1.7 gm/serving
Chia seeds are a good source of plant omega 3 ALA. One ounce of chia seeds "sabza" provide 5 gm of ALA. Chia seeds are also a good source of antioxidants, fiber and calcium. This petite whole grain has a mild flavor and can be eaten whole or ground, raw or cooked. Chia seeds can be soaked in water and added to salads, dhal or chapatti flour. Try them sprinkled on yogurt, salad and soup or tossed with rice. Traditionally chia seeds are used in Indian desserts that are high in saturated fat and calories e.g. kulfi faluda. To increase intake of ALA, flax seed powder can also be used in preparing curries like sambar or dhal (lentil soup), vegetables, chappatis and salad dressing.
Monounsaturated fat(omega-9)
Monounsaturated fat (omega-9) are considered "good" fats because they may lower LDL (bad) cholesterol and may help raise HDL (good) cholesterol. Good sources of monounsaturated fats are:
- Olive oil, canola oil, peanut oil
- Avocados, olives (high in sodium)
Table 2: American Heart Association Recommendations for Omega-3 Fatty Acids (2002)
| Population | Recommendation |
|---|---|
| Persons who do not have heart disease | Eat a variety of fish (preferably oily) at least twice a week, include oils and foods rich in ALA |
| Persons disease who have heart | Consume 1 gm of EPA+DHA per day, preferably from fatty fish. Supplements could be used in consultation with a physician |
Preventing Heart Disease in Asian Indians: Diet & Lifestyle Recommendations
- Nuts: almonds,peanuts,pecans,pistachios, hazelnuts
Polyunsaturated fat (omega- 6)
Polyunsaturated fat (omega- 6) are considered "good" fats because they help lower LDL (bad) cholesterol when used in place of saturated fat. Good sources of polyunsaturated fat (omega 6) are:
- Com oil, safflower oil, sunflower oil
- Sunflower seeds
2. Saturated fats
Saturated fats are considered "bad" fats because they can raise LDL (bad) cholesterol. Saturated fats should be avoided or eaten in small amounts. Saturated fats are solid at room temperature. Sources of saturated fat are:
- Fatty cut of lamb, pork, beef, poultry with skin, beef fat, lard, bacon, sausage, hotdogs
- Whole milk & whole milk dairy products: butter, cheese, cream, ice-cream, yogurt made from whole milk
- Palm oil, palm kernel oil and coconut oils
3. Trans-fats
Trans-fats are also considered "bad" fats because they can raise "bad" LDL cholesterol and should be eaten in small amounts. Trans-fats are primarily man-made from vegetable oils as a result of food
processing which changes vegetable oils into semi solid fats e.g. partially hydrogenated fats. Trans-fats are also produced when oil is re-used. Trans-fats are also found naturally in meat, cheese, butter and dairy products. Sources of trans- fat are:
- Baked goods: pastries, cakes, donuts, cookies
- Fried foods: French fries, fried chicken, onion-rings, Indian savory snacks cooked in re-used oil e.g. chevda, bhel
- Stick margarine, shortening, dalda (vanaspati)
Diel lo lower blood pressure
Although some salt is essential to maintain life excessive intake of salt (sodium chloride) can raise blood pressure. The American Heart Association recommends no more than 1500 mg of sodium per day. A high salt intake also has effects causing damage to the heart, kidneys, and arteries independent of blood pressure. Be aware of how much salt is added to food during preparation and also read labels of ready-prepared foods. In addition to a low salt diet a blood pressure lowering diet should also be low in saturated fat and high in vegetables, fruits and non-fat dairy products. Weight loss and increased physical activity are also important components of a blood pressure lowering diet,
Six strategies for a heart healthy diet for Asian Indians
The following six strategies are practical tips geared towards the Asian Indian cuisine. For regional cuisines, refer to the variety of regional cuisines in this book e.g. Bengal, Gujarat, Mal1arashtra, North India, South India and Nepal.
Strategy # 1 Protein Foods: 2 to 3 Servings Daily
- One serving includes ½ cup cooked lentils (dhal or dal or daals) or ½ cup cooked dry beans (rajma, channa, soy beans), or 2-3 oz each of protein foods e.g. lean meat, fish or poultry (chicken & turkey) or 4 oz tofu or one egg plus two egg whites combined.
Choose a variety of protein foods if your religion allows. Good food sources of protein include beans, lentils, seafood, poultry, lean meat and egg whites. Fatty fish e.g. salmon is an excellent source of omega 3 fatty acids (good fat).
- Eat fish twice at least per week if religion permits. Increase the amount and variety of fish and seafood consumed by choosing seafood in place of some meat and poultry if your religion pennits. Fish with lowest mercury are preferred. These fish are smaller in size e.g. salmon, pollock, catfish, cod, clams, flounder, sole, canned light tuna, shrimp, crabs and scallops.
Indian Foods: AAPI's Guide to Nutrition, Health and Diabetes
- One egg three times per week is quite acceptable in an otherwise low saturated fat/low cholesterol _ diet. Substitute frequently with egg whites e.g. egg white omelets. Egg whites have no fat or cholesterol while they are an excellent source of protein.
- Tofu is a good source of protein especially for vegetarians. To reduce saturated fat, consume tofu in place of paneer in "palak paneer" or "matar paneer".
- Lentils (daals) or legumes (rajma, channa, black eyed beans) prepared with only a small amount of oil are an excellent source of protein and soluble fiber.
- Soybeans (edamame) are an excellent source of protein & fiber. Legume (dried beans and lentils) including "daal" are naturally low in fat, high in protein and carbohydrate, plant sterols and fiber.
- Vegetarian burger patties can be a convenient and nutritious alternative to tl1e meat patties. Check tl1e total fat, saturated fat and cholesterol content on tl1e label.
Strategy # 2 Dairy Products 2 to 3 Servings Daily
- One sen1ng includes 1 cup=8oz non-fat milk or 1% milk or low fat buttermilk or non-fat yogurt.
- Increase intake of fat-free or lmv-fat milk cu1d milk products, such as milk, yogurt, cheese, or fortified soy beverages.
- Select evaporated skim milk or non-fat powder milk or non-fat yogurt when making fruit smoothies, fruit shakes and desserts.Use 1% milk or evaporated skim milk (along with sugar·substitutes) when preparing Indian desserts e.g.kheer, payasscun, paneer or chenna.
Strategy # 3: Vegetables & Fruits 8 Servings (4.5 Cups) Daily
- Increase vegetable and fruit intake. Eat a variety of vegetables, especially dark-green cu1d red cu1d orange vegetables and beans and peas.
- Consume a higher intake of vegetables than fruits. Fruits are higher in carbohydrates as well as calories than vegetables. For e.g. one sen1ng of a vegetable equals ½ cup cooked or 1 cup raw=25 calories cu1d one serving of a fruit = one small to medium fruit or ½cup fresh fruit=60 calories.
- Select green vegetables in place of starchy ones as starchy vegetables are higher in calories and carbohydrate. Consume leafy green vegetables (spinach, cabbage, kale, mustard greens) & cruciferous vegetables (cauliflower, brussel sprouts, broccoli) eitler raw or prepare them in a small amount of oil
Strategy # 4: Whole Grains: 6 Servings Daily
- Consume at least half of all grains as whole grains. Increase whole-grain intake by replacing refined grains with whole grains. Reduce the amount of rice/chapatis when potatoes or other starchy vegetables are also included in the same meal.
- Select 100% whole wheat chapati flour. Add oatmeal (high in soluble fiber) &/or soy flour (high in protein) to chapatti flour. To control calories, avoid putting ghee/oil when making chapatis
Substitute other whole grains for rice & pulao e.g. quinoa (high in protein), barley and oats (high in soluble fiber), brown rice (high in fiber).
Choose foods with soluble fiber to help lower LDL cholesterol (bad cholesterol) e.g. whole oatc;, barley, dried beans, fruits and vegetables such as okra, brussel sprouts.
Limit the consumption of foods that contain refined grains cooked with solid fat., (butterghee, shortening) and added sugar e.g. cookies, cakes, pies and indian sweets such as laddoos, mathris, shakarparas.
Preventing Heart Disease in Asian Indians: Diet & Lifestyle Recommendations
Strategy # 5: Fats & Oils 4-6 tsp Daily
- 1 serving - 1 tsp oil or 6 almonds, or 2 walnuts or 2 TBS avocado
- Prepare foods using lower fat cooking methods such as grilling, broiling and baking instead of frying and sauteing. To reduce caloric intake, cook with a minimum amount of oil.
- Avoid ghee, butter, whole milk & cream in food preparation & processed foods to reduce saturated fat intake. Avoid coconut or coconut cream or use a lesser amount than call for in the recipe. Although coconut and coconut cream are high in saturated fat, coconut water (nariyal- paani) is not high in saturated fat. Limit use of whole milk in Indian tea "chai" because it adds saturated fat in the diet.
- Limit consumption of sweets e.g. pastries, kulli, rasmalai, kheer, barfi, halwa pcclas, pies, cake and cookies. These are generally prepared with saturated fat e.g. butter, ghee and whole milk and may raise LDL cholesterol, triglyceride and body weight.
- Avoid foods high in trans-fats. Like saturated fat, trans- fat raises LDL cholesterol levels & may lower "good" HDL cholesterol. Re-use of cooking oils increases the trans-fat content of the oil. Trans-fats are found in Indian savory/snack foods e.g. mathri, shakar paras chewda, bhel, sev etc. These are made with saturated fat and trans-fat e.g. ghee, shortening (vanaspati) and re-used cooking oils.
- Select a heart healthy spread (free of saturated and trans- fat) instead of butter or ghee, Read the label to make sure there is no "partially hydrogenated" oil in the ingredients list. Then look for as little saturated fat as possible. Look for spreads with less than a total or 2 grams from saturated and trans-fat per serving. Also look for "light" or "lite" spreads as they are half the calmies and also half the fat of regular spreads.
- Plant sterols and stanol-esters are found primarily in fortified foods e.g. Bennecol spread and Promise Active spread. Only 2 or 3 tablespoons of these spreads containing plant stanol esters provide 2 grams of plant stanols and may lower LDL cholesterol by 7-15 %. Beverage supplements containing plant stanols such as Cholest-off cmd Minute Maid Heart Wise orange juice may also help lower LDL cholesterol. Plant sterols in food or supplements should be consumed with meals because they help to lower the absorption of dietary cholesterol. The largest LDL cholesterol lowering response is noted when the dose is spread Over two or 3 meals per clay. Higher doses above 2 g/day offer little additional benefit. Since plant sterol/stanol fortified spreads and supplements also provide calories, other sources of fats should be reduced to maintain caloric intake to avoid weight gain.
- Avoid excessive intake of nuts and avocados as they are high in calories and may lead to weight gain. However, inclusion or few unsalted nuts e.g. walnuts, almonds, peanuts, pistachios in a heart healthy diet may decrease LDL cholesterol when weight is not gained. When weight is not gained, consumption of 5 oz of unsalted nuts per week is associated with a reduced risk of heart disease.
- In Indian restaurants select appetizers and entrees cooked in a tandoor. Good choices for appetizers are tandoori fish, tandoori vegetables, vegetable salads, fruits salads (fruits chaat) & roasted papadam with mint chutney. Avoid entrees prepared with added cream or butter or fried foods.
Strategy # 6 Decrease your Salt Intake to 1500 mg Sodium Daily to Lower Blood Pressure
- The American Heart Association and the recent US dietary guidelines recommend less than 1500 mg of sodium per clay. This sodium goal is lower than in previous guidelines because new data support this limit.
Indian Foods: APJ's Guide to Nutrition, Health and Diabetes
- Reduce salt intake by cooking with as little salt as possible.
- Compare sodium in foods by reading labels e.g. soup, bread & frozen meals. Choose foods with lower numbers.
- Substitute salt with herbs & spices e.g. cilantro, mint, cumin, black pepper, lemon.
- Avoid highly salted foods e.g. salted nuts, pickles, chutneys and salted savory/snack foods e.g. chevda, bhel etc.
- Prepare savory snack foods e.g. chewda, bhel etc at home with minimum salt and oil. To reduce salt in the recipe, enhance flavor by using more spices e.g. amchur, cumin, asafetida.
Alcohol Guidelines
If you drink and if your physician approves because you have no medical reasons not to drink alcohol, you should limit to one drink or less per day for women and two drinks or less per day for men. In general, one drink is 1 jigger or 1.5 oz hard liquor (80 proof spirits) e.g. whiskey, bourbon, vodka etc or 5 oz dry red or white wine or 12 oz beer.
What is the role of vitamin supplements and antioxidants in preventing heart disease?
Vitamin C supplements in combination with vitamin E and/or beta carotene have not shown any benefit in the prevention of heart disease. Some studies have shown they could be harmful. Vitamin D is also under study. It is expected that ongoing research will shed further light on the role of vitamin D supplementation in the prevention of heart disease.
Do you need a Registered Dietitian (RD) ?
A registered dietitian has expertise in nutrition. With the help of a RD, a heart healthy meal plan will be developed while taking your personal food preferences and medical history and lab reports into account. Follow up visits with your RD are also recommended to reach your heart health goals. This is referred to as medical nutrition therapy (MNT) by a registered dietitian (RD).
Geeta Sikand, MA, RD, CDE, Cl.S is a consultant dietitian in private practice in Irvine, California and an Associate Clinical Professor of Medicine: Cardiology at the University of California Irvine. Contact information (949) 726-1840 or gsikand@gmail.com
References
- South Asia at Health Crossroads with High Rates of Heart Disease, Diabetes, Obesity and Other Non communicable Diseases- New World Bank Report. Press Release No: 2011/325/SAR Washington, February 9, 2011. www.worldbank.org/ sarncdreport
- An epidemic of risk factors for cardiovascular disease The Lancet, Volume 377, Issue 9765, Page 527 , February 12, 2011.
- Effectiveness-Based Guidelines for the Prevention of Cardiovascular Disease in Women-2011 Update: A Guideline from the American Heart Association. Executive Writing Committee, Mosca L, Benjamin EJ et al Circulation. 2011; 123:00-00. Februcu 16, 2011.
- The Importance of Population-Wide Sodium Reduction as a Means to Prevent Cardiovascular· Disease and Stroke: A Call to Action from the American Heart Association". Appel et al http://circ.ahajounals.org Published on line Circulation Jan 13, 2011
- 2010 Dietary Guidelines for Americans released January)"31,2011\\IWw.dietaryguidelines.gov.
- The Practical Guide: Identification, Evaluation and Treatment of Overweight and Obesity in Adults: Bethesda, Md: National Institute of Health National Heart Lung & Blood Institute; 2000.NIH Publication No 00-4084. http://www.nhlbi.nih.gov/guidelines/obesity/prct gd c.pdf
- ATP III Treatment Panel Report. May 2001. Detection, Evaluation and Treatment of High Blood Cholesterol in adults. NIH Publication No. 01-3670 May 2001.
- Van Hom L, McCoin M, Kris Etherton P M, Burke F, Carson J, Champagne C, Karmally W, Sikand G. "The Evidence for Dietary Prevention and Treatment of Cardiovascular Disease." J Am Dietet Assoc 2008; 2: 287-331
- Grundy SM et al. Circulation 2005; 112: 2735- 2752.
- Enas EA. Dyslipidemia among indo-Asians: Strategies for identification and management. Brit J of Diabetes and Vascular Dis 2005; 5: 81- 90 (Review).
- Superko HR, Enas EA, Kot.ha P, Bhat NK, Garrett B. High-density lipoprotein subclass distribution m individuals of Asian Indian descent: the National Asian Indian Heart Disease Project. Prev Cardiol 2005; 8:81-6.
- Bhalodker N, Blum S, Rana T, Bhalodker A, Kitchappa R, Kim K-S, Enas EA. Comp;u-ison of large ;md small High density lipoprotein cholesterol in Asian Indian men compared to men in the Framingham Offspring Study. Am J Cardiol 2004; 94: 1561-1563.
- Eckel RH et al Preventing cardiovascular disease and diabetes; a call to action from the Amer Diabetes assoc and the Amer Heart Assoc. Diabetes C
- Lichtenstein AH et al Diet & Lifestyle Recommendations revision 2006: A Scientific Statement from the American He;ut Association Nutrition Committee. Circulation, 2006; 114:82-96
- Look AHEAD Research Group. Reduction in Weight and Cardiovascular Disease Risk Factors in Individuals with Type 2 Diabetes. Diabetes Care 2007;30:1374-1383.
- Abumweis SS, Barake R, Jones PJ. Plant Sterols/stanols as cholesterol lowering agents: a meta-analysis of randomized controlled trials. Food Nutr Res. 2008;52. Doi: 10.3402/ fnr.v52i0.1811.
- Grundy SM, Brewer HB, Cleeman JI, Smith SC, Lenfant C, for the Conference Participants. Definition of the Metabolic Syndrome, Report of the National Heart, Lung, and Blood Institute/American Heart Association Conference on Scientific Issues Related to Definition. Circulation. 2004; 109: 433-438.
- Screening for Obesity in Adults: Recommendations and Rationale, Rockville, Md: Agency for Healthcare Research and Quality, US Preventive Services Task Force: Nov 2003. http://www.ahrq.gov/clinic/3rduspstf/obesity/obesrr.htm
- Sikand G, Kris Etherton PM & Frank GF. Cardiovascular· Nutrition: In Wong ND, Garden J & Black H, eds. Preventive Cardiology, McGraw Hill 1999; 13: 319-72.
- Mccoin M, Sikand G, Johnson E & Vanhorn L. The Effectiveness of Medical Nutrition Therapy Delivered by Registered Dietitians for Disorders of Lipid Metabolism: A Call for Further Research. J Am Dietet Assoc 2008; 2:233-239
- Sikand, G; Kashyap, ML; Wong ND; Hsu .J C. Dietitian intervention improves lipid values and saves medication costs in men with combined hyperlipidemia and a history of niacin non compliance. J Am Diet Assoc. 2,000; 100:218- 224.
- Dhawan J. Coronary heart disease in Asian Indians. Curr Opin Lipidol. 1996;7: 196-198.
- Yagalla MV, Hoerr SL, Song WO, Enas E, Garg A. Relationship of diet, abdominal obesity, and physical activity to plasma lipoprotein levels in Asian Indian physicians residing in the United States. J Am Dietet Assoc. 1996, 96(3): 257-61.
- Grundy SM. Small LDL, atherogenic dyslipidemia, and metabolic syndrome. Circulation. 1997; 95:1-4.
- Reaven G. Insulin resistance and compensatory hyperlinsulinemia: role in hypertension, dyslipidemia and coronary heart disease. Am HeartJ. 1991;121:1283-1288
- Sikand G, Kashyap ML, Yang I. Medical Nutrition Therapy lowers serum cholesterol and saves medication costs in men with hypercholesterolemia. J Am Diet Assoc. 1998;98: 889-894.
- Barnett and Garg, Preventing cardiovascular complications in diabetes and Szapary and Conway, Functional foods in the prevention of cardiovascular disease In: Carson, Burke, Hark. Cardiovascular Nutrition: Disease Management and Prevention. Chicago, IL: American Dietetic Association, 2004
- What you need to know about mercury in fish and shellfish. FDN/CFSAN Consumer Advisory EPA-823-R-04-005. March 2004. http://www.cfsan.fda.gov/ ~dms/admehg3.html.
Chapter 4
Renal Diet for Asian Indians
Chhaya Patel, MA, RD, CSR
1 meat serving =
- 1 oz. of poultry, seafood, or fish
- 1 medium egg or ¼ cup egg substitute
- ¼ cup tuna
- 1 oz. natural cheese(Limit to________ ounces per week.)
- ¼ cup cottage cheese (Limit to______per week.)
1 bread or starch =
- 1 slice of bread/Chapati/puri/½ nan
- ½ cup cooked rice or noodles
- ¼ pita (6 in. wide)
- ½ cup cooked cereal
- ¾ cup dry cereal
- ½ bagel or sandwich bun
1 vegetable serving =
- ½ cup vegetables
- 1 fruit serving =
- ½ cup canned fruit
- 1 medium-sized fresh fruit (about the size of a tennis ball)
- ¼ - ½ cup fruit juice
- Fresh fish, eggs and poultry
- Enriched bread or pasta and rice
- Allowed vegetables and fruits
- Olive oil, butter or margarine
Foods to Enjoy
The following food and diet information will help you to eat as healthy as possible while receiving hemodialysis treatments.
Protein
Protein is the backbone of the hemodialysis diet. It is necessary for growth and repair of body tissues. It helps your body fight infection and prevents loss of muscle. The highest quality protein comes from animals. Although plant foods have protein, the quality is low. Those on hemodialysis need high quality protein.
Foods to Enjoy
Fish
- Bass
- Catfish
- Carp
- Codfish
- Flatfish
- Grouper
- Halibut
- Haddock
- Kingfish
- Perch
- Salmon, fresh
- Snapper
- Sole
- Tilapia
- Trout
- Tuna, fresh
Poultzy
- Chicken
- Cornish hen
- Duck
- Goose
- Turkey
Seafood
- Clam
- Crab
- Lobster
- Scallops
- Shrimp
Indian Foods: AAPI's Guide to Nutrition, Health and Diabetes
Acceptable Starches

White Rice

Vermicelli

Chapati

Parathas

Masala Dosai

Pongal

Puris

Jowar Roti

Naan
Renal Diet for Asian Indians
Miscellaneous
- Eggs
- Egg Substitute
- Cottage cheese
Reminder!
Always remember to take your phosphorus binders with a meal or snack.Protein foods are high in phosphorus.
Portion Guide for Protein Foods
- Half chicken breast is about 3 to 4 ozs.
- Chicken thigh is about 2 to 2 ½ ozs.
- Chicken leg is about 1 to 1 ½ ozs.
- Deli roast meats, 2-3 slices are about 3 ozs.
- 12 large shrimp are about 3 ozs.
- ¼ cup of unsalted tuna is 1 Oz
- 1 egg is equal to 1 oz.
- ¼ cup egg substitute is 1 oz.
Dialysis and Protein Foods
Each time you have a hemodialysis treatment, protein is removed from your blood along with the waste products. The amount of protein you eat must be enough to replace that loss in hemodialysis and provide your daily requirements.
To determine whether you are getting enough protein , the amount of Albumin in your blood will be measured monthly. If your albumin is 4.0 or higher you are eating enough protein. Studies have shown that people on dialysis who have an albumin of 4.0 or higher live longer and healthier.
These protein-rich foods are high in sodium and should be limited or used sparingly
Processed Meats
- Lunch meats
- Pickled fish
- Sardines/canned fish
Other Foods
- Cheese
- Buttermilk
- Canned or frozen dinners
- Canned or packaged soup
- Fast foods
- Pot pies
These protein foods are high in Potassium and Phosphorus. Check with your Dietitian before using
- Pinto beans
- Brown beans
- Navy beans
- Red beans
- Black beans
- Lima beans
- Refried beans
- Purple hull peas
Peanuts/peanut butter
Can I be a vegetarian if I have chronic kidney disease?
If you are diagnosed with chronic kidney disease (CKD) and are a vegetarian you can remain as one. You do not have to start eating meat because you have CKD or have started dialysis. In order to continue with your vegetarian lifestyle as well as incorporate a renal diet, you will need to devise a meal plan to fit your nutritional needs. You should talk with a renal dietitian about foods that are kidney-friendly and vegetarian-specific. Here are some things your dietitian may implement for your new diet:
- Monitor your calorie intake to make sure you are getting enough calories.
- Include vegetarian sources of protein and calorie supplements when needed.
- Increase your phosphate binders that may be needed for meals and snacks.
- Lower potassium dialysate for those on dialysis to control potassium levels.
- Make sure your dialysis prescription is adjusted as needed for acceptable urea clearances.
- Provide resources and renal education material specific to your needs.
indian Foods: AAPI's Guide to Nutrition, Heald1 and Diabetes
Kidney-friendly foods for a vegetarian
Vegetarian diets can meet protein needs. Protein is made up of chains of amino acids, which are sometimes referred to as "the building blocks of life." Plant foods contain many essential amino acids and some can be considered as complete protein foods. Some plant protein may lack one or more essential amino acids, but a variety of vegetarian foods can be combined throughout the day to provide adequate amounts of essential amino acids without consuming meat, eggs or milk. Plant protein can be enough to get adequate protein into your renal diet.
Protein enriched foods for vegetarians on a kidney diet can include:
- Meat analogs (meat substitutes such as soy burgers, tofu hot dogs and deli slices)
- Soy products (tofu, tempeh)
- Beans and lentils
- Nuts and nut butters
- Eggs and egg substitutes
- Dairy products
- Grains
The protein and nutrient content can vary for tofu products, soy milk and meat analogs. It is important to check product labels for the specific nutrient content per serving (such as protein, sodium, potassium, phosphorus, etc.). Powder and liquid protein supplements may be an option for patients with unusually high protein needs or who are unable to meet their protein needs by food alone. Eggs or egg substitutes are a source of HBV (high biological value) protein, also known as high quality protein. HBV protein can be consumed by lacto-ovo vegetarians.
Calories
It is important that you eat a variety of foods-not just protein. If you do not get enough calories from foods other than those high in protein, your body will break.down your muscle tissue to use for energy. You may need to add some high calorie foods to keep from losing weight or to regain weight you have lost.
High calorie foods to enjoy (If you have diabetes, please consult your dietitian before using these foods)
Candy
- Mints
- Gum drops
- Hard candies
- Jelly beans
- Marshmallows
Cake
- Angel food cake
- White/yellow cake with icing
- Coffee cakes without nuts
- Pound cake
Pie
- Fruit pies with allowed fruits
- Lemon meringue pie
- Fruit tarts
Miscellaneous
- Danish rolls
- Donuts (raised)
- Honey
- Jam or jelly
- Lemonade
Renal Diet for Asian Indians
- Vanilla sandwich cookies
- Sugar cookies
- Syrup
- Table sugar
- Toaster pastry
- Vanilla wafers
- Non-dairy whipped topping
Indian Desserts
- Burfi
- Halwa
These foods are high in Phosphorus and/or Potassium. Please limit or avoid!
- Candy with chocolate, nuts or peanut butter
- Chocolate cake
- Bro-wnie
- Fudge
- Chocolate cookies
- Cream pies
- Sweet potato pie
- Pumpkin pie
- Milkshakes
- Nuts
- Potato chips
- Ice cream
- Burfi and Halwa
- Dessert made with milk
Helpful Hints for Adding Calories
- Add sugar to beverages and cereal
- Add jam, jelly, honey or syrup to bread, muffins, cmd rolls
- Drink beverages that have calories
- Eat an allowed dessert daily
- Add whipped topping to dessert or fruits
- Eat allowed candies between meals
- Spread frosting on cakes and cookies
- Spread margarine or butter on hot bread or rolls
- Use margarine or butter on cooked vegetables, rice, noodles and cooked cereals
- Fry meats, fish or eggs in margarine or oil
- Add low salt gravies to your meat.
- Use mayonnaise or salad dressing on sand" ches and salads
More high calorie foods to enjoy
Fats can add a lot of the calories you may need if you want to gain or maintain weight.
- Butter
- Ghee
- Margarine
- Crecun cheese
- Cooking oil
- Mayonnaise
Your portions of these foods will be reduced if you are on a low fat, low cholesterol d1et Please consult your dietitian.
Phosphorus
Phosphorus is a mineral that is necessary to build strong, healthy bones and teeth. It is also important in storing and efficiently using energy in body cells. When the kidneys are not working the phosphorus level can get too high. A high phosphorus level can make your bones weak and brittle and also lead to calcium deposits that can form in the blood vessels and soft tissues of your body. A good phosphorus level for people on dialysis is 3.5 to 5.5.
There are 3 ways to keep your phosphorus in good range
- Come to and complete all of your dialysis treatments.
- Follow your diet.
- – Eat low phosphorus foods. Ask your dietitian to suggest some.
- – See "Foods That May Cause Phosphorus Trouble" below.
- Take your phosphorus binders
- – Phosphorus is in almost all foods so it is important to take your phosphorus binders every time you eat.
Phosphorus Binders
Binders keep phosphorus out of your blood. Phosphorus binders are taken with meals and snacks. Remember...the only way binders work is to take them with food. Phosphorus binders come in many names: Renvela, Fosrenol, PhosLo, Calcium Carbonate (Tums), Alternagel are some of the names. Take the amount of binders that are prescribed for you! Your Dietitian or Doctor will tell you how much binder you need to take with each meal and snack to keep your phosphorus normal.
Foods that May Cause High Phosphorus (Please limit or avoid!)
Dairy Products
- Milk, eggnog
- Cheese
- Yogurt
- Pudding
- Custard
- Ice cream
- Cream soups
- Milkshakes
- Casseroles made with cheese
Dried Beans
- Red or black beans
- Mung beans
- Lentils and Dals
- Navy beans
- Lima beans
- Pinto beans
- Kidney beans
- Blackeyed peas
- Pork and beans
- Soybeans
Nuts and Seeds
- Pecans
- Almonds
- Cashews
- Walnuts
- Peanuts
- Peanut butter
- Sunflower seeds
- All other nuts and seeds
Protein Foods
- Enhanced meats
- Liver
- Oysters
- Canned salmon
- Organ meats
- Sardines
Whole Grains and Cereals
- Bran
- Granola, trail mix
- Brown rice
- Bran muffin
- Whole grain breads
- Whole grain cereals
- Biscuit, canned, froz, or fast food
Other Foods
- Beer
- Colas & all phosphoric acid-containing drinks
- Pizza
- Cocoa
Renal Diet for Asian Indians
- Molasses
- Macaroni and cheese
- Wheat germ
- Carmel
- Chocolate
- Dried fruits
- Coffee drinks made with milk
- Cake donuts
- Commercial pancakes and waffles
- Desserts made with milk Helpful
Hints to Lower Phosphorus
- Use non-dairy milk substitutes, such as Mocha Mix®, Coffee Rich®, Coffee-Mate, Rice Dream® or Dairy Delicious® in place of milk on cereals and in recipes.
- Try cream cheese on crackers or sandwiches instead of cheese or peanut butter.
- when using cheese in cooking, choose the sharpest flavor and use less than the amount listed in the recipe.
- Enjoy sorbet, fruit ice, Italian ices, popsicles or sherbet instead of ice cream for a cool and tasty treat.
- Drink non-cola sodas. All cola drinks (diet and regular) contain phosphoric acid. Try some of the flavored seltzer waters or make your own. Check labels on canned or bottled beverages to make sure they do not contain phosphates.
- Eat popcorn (unsalted) instead of nuts for a snack.
- Choose hard candy as it has less phosphorus than chocolate.
- Try mixed vegetables instead of lima beans or corn with meals.
- If biscuits, pancakes, and waffles are a favorite, make them from scratch as mixes and commercial products are high in phosphorus.
Phosphate restriction for vegetarians with kidney disease
About 50 to 70 percent of phosphorus is absorbed in the body from a typical diet of both plant and animal-based foods. In general, phosphorus is greater in animal products than from plant-based food. Much of the phosphorus in grains and legumes can be in the form of phytic acid, known as the main storage area of phosphorus in many plant tissues, which reduces the absorption of phosphorus to around 50 percent.
Legumes, nuts and seeds will need to be limited for patients with chronic kidney disease, if potassium and phosphorus levels become an issue. Consumption of a vegetarian diet may require an increase in the number of phosphate binders for patients in end stage renal disease. (ESRD) or on dialysis.
Potassium
Potassium (K) is a mineral that is necessary to keep your muscle., functioning properly. The heart is your biggest muscle. That is why your heart is affected when potassium levels are too high or too low.
Healthy kidneys regulate the amount of potassium the body needs. In kidney failure, the amount of potassium in the body can get too high and cause dangerous problems .
High Potassium in the blood may cause:
Nausea
Difficulty breathing
Irregular heartbeat
↑K Cardiac arrest/heart attack
Tingling In tJ1e
extremities Loss of
consciousness Slow or
weak pulse
Indian Foods: AAPI's Guide to Nutrition, Health and Diabetes
Low Potassium in the blood may cause:
- Muscle weakness
- Nausea, vomiting, diarrhea
- Irregular heartbeat
- Dizziness
Normal Potassium Level 3.5 to 5.5.
- Your dialysis treatment helps control your • blood potassium level. Make every scheduled • treatment and stay the full length of the treatment.
- If your Potassium is lower than this you should talk to your Dietitian about getting more potassium in your diet.
- If your Potassium is higher than this you should limit the amount of potassium that you eat.
- Most of the Potassium in your diet comes from Fruits and Vegetables. Use the following tables to determine which fruits and vegetables are the best choices.
Foods to Enjoy(Serving Size 1/2 cup unless otherwise stated)
- Apple, applesauce
- Apricots(1)
- Blackberries
- Blueberries
- Boysenberries
- Cherries
- Coconut
- Cranberries
- Cranberry sauce
- Figs(2)
- Fruit cocktail
- Grapefruit(½)
- Grapes
- Kumquats
- Lemon
- Lime
- Manclcuin oranges, canned
- Peaches, end, fresh 1 small or ½ lge
Fruit

- Pears, canned,1 small or ½ lge
- Pineapple, fresh or canned
- Plums (2)
- Prunes (2)
- Raspberries

Rhubarb
- Strawberries (5 medium)
- Tangerine (1)
- Watennelon (1 cup)

Juices
- Apple
- cranberry
- grape
- Pineapple
- peach nectar
- pear
- nectar
- apricot nectar
Grapefruit juice: Discuss medication reactions with your dietitian or doctor:
Vegetables
- Asparagus
- Bamboo shoots, canned
- Bean sprouts
- Beets, canned
- Broccoli
- Brussels sprouts
- Cabbage
- Carrot
- Cauliflower
- Celery
- Collards
- Corn*
- Cucumber
- Eggplant
- Endive
- Green beans, wax beans
- Kale
- Leeks



- Lettuce
- Mushrooms
- Mustard greens
- Okra
- Onion
- Parsley
- Peas, green*
- Peppers, green or red, mild or hot
- Radishes
- Summer squash
- Spaghetti squash
- Snow peas
- Toria
- Turnips & turnip greens
- Watercress
- Waterchestnuts, cnd
- Zucchini

Potatoes-0nly if soaked 2 to 4 hrs to reduce potassium (Ask your dietitian about "Dialyzing" potatoes)
(*allowed but high in phosphorus)
Food that May Cause High Potassium(Please limit or avoid!)
Fruits
- Bananas
- Cantaloupe
- Casaba melon
- Dates
- Dried fruits
- Honeydew melon
- Kiwi
- Mango
- Nectarine
- Oranges
- Papaya
- Persimmons
- Starfruit (carambola)
(poisonous for dialysis pts,not based on K+ content). Do Not Eat!
Juices
- Orange juice
- Prune juice
Avoid any juices with added calcium
Miscellaneous Foods
- Bran cereal
- Chocolate
- Salt substitute
- Lite salt
- Nuts and seeds
- Soy milk
- Artichokes
- Avocado
- Bamboo shoots, fresh
- Beans, dried, ckd (kidney, lentils, lima, navy, pinto, soy)
- Beets, fresh and beet greens
- Cactus
- Chard
- Chinese cabbage
- Fenugreek leaves
- Kohlrabi
- Papadi
- Peas (dried)
- Pickles
- Potatoes, unless "dialyzed"
- Pumpkin
- Rutabagas
- Sauerkraut* *
- Spinach (cooked)
- Succotash
- Sweet potatoes
- Tomato
- Tomato paste, puree or sauce
- Tuver
- Waterchest:nuts, fresh
- Carrot juice
- Tomato juice* *
- Prune juiceM
- Vegetable juices* *
- V-8 juice cocktail * *
Vegetables
Juices
* * also High Sodium
Helpful Hint
Reduce the amount of potassium in vegetables by dialyzing them.
- Clean, peel and thinly slice or chop the vegetable.
- Cover vegetable with water and soak for one hour. Potatoes should be soaked two to four hours or longer.
- Drain the water and cook the vegetable your favorite way.
Potassium restriction for vegetarians with kidney disease
Fruits and vegetables are the biggest source of potassium and may need to be limited for vegetarians with chronic kidney disease. Other foods high in potassium that vegetarians may use are soybeans, textured vegetable protein (TVP), soy nuts, soy flour, natto (soybean paste) and wasabi. Careful planning of these foods can be worked into a vegetarian diet. However, potassium amounts will need to be modified and levels monitored carefully.
Sodium
Too much sodium can cause:
- High blood pressure
- Increased thirst
- Damage to the heart
- Difficulty breathing
- Puffiness and swelling
Therefore, you should limit the amount of sodium in the foods you eat.
Sodium in Foods
- The main source of sodium in the diet is salt.
- Sodium generally comes from convenience foods, fast foods, processed and canned foods, and snacks that have sodium or salt added during their processing.
- To reduce the salt, and therefore sodium, in your diet, decrease your intake of processed foods. This means any food that has been processed. If a food is not fresh, it is usually high in sodium.
Helpful Hints
- Many restaurants are providing nutrition information including sodium.
- Learn what foods contain large amounts of sodium and which foods have a small amount of sodium.
- Read labels. Compare different brands of similar items (like salad dressings) and choose the one with the least sodium.
|
Instead of |
Use this |
|
§ Canned vegetables |
§ Fresh or frozen vegetables, cooked |
|
§ Processed meats (ham, bacon, bologna, etc) |
§ Unprocessed meats, fish, seafood, or poultry, cooked without salt |
|
§ Convenience/ready made foods (boxed, canned, or frozen meals) |
§ Buy fresh natural ingredients and cook them with herbs and spices. |
|
§ Fast Foods |
§ Pack sandwiches using fresh, unsalted ingredients. |
|
§ Salted snack foods (chips, pretzels, etc) |
§ Eat fresh, crisp fruits and vegetables for crunch without salt; apples, carrots, green pepper strips, cucumber slices, etc. |
Sodium restriction for vegetarians with kidney disease
Sodium content of some vegetarian foods can be high. The foods with high sodium content are usually processed, commercially-produced plant proteins. To reduce sodium intake, the use of high sodium foods such as meat analogs, salted nuts, miso, frozen entrees, marinated tofu products,savory snacks and meals in a cup should be limited. In comparison to meat, meat analogs have much higher sodium content and need to be limited.
|
Type of meat |
Amount of protein |
Amount of sodium |
|
Meat, 1 ounce |
7 grams |
25 mg |
|
Meat analog |
7 grams |
260 mg |
Add a little spice…
Mix these spices together and use instead of salt.
- Garlic powder
- Marjoram
- Thyme
- Parsley
- Savory
- Mace
- Onion powder
- Black pepper
- Sage
- Cumin
- Curry powder
- Garam masala
Other low sodium seasonings to use
Almond extract, allspice, anise, basil, bay leaf, carraway seed, cardamom, celery seed, chili powder, chives, cilantro, cinnamon, clove, cumin, curry, dill, dry mustard, garlic, garlic powder, ginger, horseradish, lemon juice, mace, maple extract,onion powder, oregano, paprika, parsley, pepper, peppermint, poppy seeds, poultry seasoning, rosemary, saffron, sage, Tabasco® brand hot sauce only (other have added sodium), tarragon, thyme, vanilla extract, vinegar, Wright’s Liquid Smoke®, Mrs. Dash®.
High sodium seasonings to avoid
Accent ®, BBQ sauce, seasoned salt such as Lawry’s® ,celery salt, garlic salt, onion salt, Old Bay®, pickles, soy sauce, steak sauce, Worchestershire sauce.
Salt substitues contain potassium chloride (KCl) and should not be used by hemodialysis patients. Check labels on seasoning blends to make sure KCl is not an ingredient. Morton’s Salt Substitute®, Nu-Salt® and Morton’s Lite Salt® all contain potassium.
Foods That May Cause High Sodium
(Please limit or avoid!)
- Processed cheese like American
- Canned or dried soups
- Canned vegetables or tomato juice
- Pizza, frozen dinners, pot pies
- Potato chips, corn chips, pretzels
- Salted microwave popcorn
- Salt pork
- Soy sauce
- Dill pickles and olives
- Barbecue sauce
- Saurkraut
Fluids
Your fluid intake must be balanced with the amount of fluid you excrete in your urine. If you drink or eat more fluid than you excrete daily you will retain fluid and gain “fluid weight”.
When measuring your fluids, use an 8 oz. cup or measuring cup.
Indian Foods: AAPI's Guide to Nutrition, Health and Diabetes
|
1 cup liquid |
= |
8 oz. |
|
½ cup liquid |
= |
4 oz. |
|
½ cup ice cream |
= |
2 oz. |
|
1 cup crushed ice |
= |
4 oz. |
|
½ cup jello |
= |
4 oz. |
|
1 cup soup |
= |
8 oz. |
|
1 can soda |
= |
12 oz. |
|
1 popsicle |
= |
3 oz. |
|
1 cup tea or coffee |
= |
6 oz. |
Here's a simple way to keep track of your daily fluid allowance
- Each morning, measure your daily fluid allowance in water and store it in a container.
- Every time you drink some type of fluid or use any other fluid like ice, jello, or Popsicle; pour out an equal amount of water out of your container.
- When all the water is gone, it will tell you that you have used up your fluid allowance and it is time to Stop!
Learn to stretch your fluid allowance to last you the whole day. Follow some of the hints provided below.
Helpful Fluid Hints
- Drink only when thirsty. Don’t drink from habit or to be sociable.
- Satisfy thirst by eating cold or frozen fruit such as grapes.
- Avoid high sodium/salty foods like canned soup, Chinese foods, fast foods, chips, etc.
- Rinse your mouth frequently with water, but don’t swallow. Keep your mouth moist all the time.
- Chew gum. Sport gums are especially helpful.
- Have a piece of hard sour candy or bite down on a piece of frozen lemon wedge.
- Water
- Milk, cream
- Soup
- Coffee
- Tea
- Lemonade
- Kool-aid
- Soft drinks
- Alcoholic drinks
- Ice
- Popsicles
- Gelatin
- Ice cream
- Choose fresh, simple items to avoid salt
- Allowed fresh vegetables and fruits are a good choice
- Fresh salad of allowed fruits and/or allowed vegetables
- Ask for oil and vinegar dressing or dressing on the side so that you can control the amount you use
- Try squeezing lemon or lime over salad greens for a dressing
- fish, seafood, chicken and other poultry
- Ask for gravies, sauces and marinades “on the side” so you can control the amount eaten
- Vegetarians can substitute beans, lentils or tofu for meats
- Portions served in restaurants may be very large; watch your serving size and take excess home
- Grilled items are good choices
- Mixed dishes such as casseroles are generally high in phosphorus and sodium
- Fresh, steamed, or fried; unsalted
- Nan, Chapati, Paratha, Puris, White or Italian breads and rolls (without garlic salt)
- Idli, Dosa and rice products
- Pasta, macaroni, noodles and rice
- Allowed fruits, sorbet, angel food cake, plain cookies, gelatin
- Desserts with out milk products, Pies or cobblers made with apple, blueberry, cherry or lemon
- Tea (made from tea bag), coffee, iced tea(made from tea bag), lemonade, water (within allowed amount of fluids)
Remember: 2 cups of fluid will equal 1 pound of weight gain!
Fluid Foods:Visible Fluids
"Hidden" Fluids
Here are some ideas to help you make good choices when dining out
Appetizers
Salad
Entrees
Renal Diet for Asian Indians
Vegetables
Breads/Starches
Dessert
Beverages
Dialysis Vitamins
Hemodialysis removes water soluble vitamins. To stay your healthiest, you should replace these vitamins by taking a renal vitamin supplement. Your doctor will prescribe a vitamin for you. Please take only vitamin and mineral supplements that have been approved by your doctor, nurse or dietitian.
Take your vitamin after hemodialysis on dialysis days and anytime on other days.
A balanced vegetarian diet that includes a variety of plant foods is able to meet the needs for vitamins and minerals, as well. The position of the American Dietetic Association on vegetarian diets states, “appropriately planned vegetarian diets are healthful, nutritionally adequate and provide health benefits in the prevention and treatment of certain diseases.”
Iron, calcium, zinc, vitamin D and B12 should not be a concern for vegetarians on dialysis. The renal vitamin that hemodialysis patients are usually prescribed should contain vitamin B12 and zinc.
Nutritional Supplements
A variety of nutritional supplements are available to provide nutrition when you are unable to eat enough or do not feel like eating. If you are having problems eating, your dietitian can provide information on supplements and recommend the best one for you.
Chhaya Patel, MA, RD, CSR is DaVita Renal / Divisional Dietitian in the San Francisco Bay Area. She is a Certified Specialist in Renal Nutrition, the Area 1 Representative for Renal Practice Group of ADA, and she was Associate Chair and Region V representative for the Council on Renal Nutrition / NKF. Contact information 925-937-0203 or chhaya88@hotmail.com.
Reference
1. Chhaya Patel and Mary Denny, Cultural Foods and Renal Diets: Multilingual Guide for Kidney Disease Patients and Clinical Guide for Dietitians, CRN Northern CA. 1997.
Chapter 5
Eastern Indian Diet: Odia & Bengali Cuisine
Ranjita Misra, PhD, CHES, FMALRC
The dietary habits of people in the Eastern coastal states of Odisha (language spoken is Odia) and West Bengal (language spoken is Bengali) include the consumption of both vegetarian and non- vegetarian food. It is rare to find strict vegetarians in this region since Brahmins of Odisha (previously called Orissa) and Bengal eat fish and meat (mostly chicken and mutton). Cooked with very little or, at times without oil, these two eastern states offer a variety of low-calorie delicacies. There are many similarities yet vast cultural and linguistic diversity exists, which along with the geographic heterogeneity makes the Odia and Bengali cuisine unique. Both regions have their distinctive food habits and cooking styles: Bhaja, Bhapa, Bhuna, Chachchari, Chhenchara, Dalma, Dalna, Dum, Ghanto, Jhol, Pora, and Tarakari. To the casual palate, the Eastern Indian food means rice and fish. Both states share the love for fish and rice due to the long coastline shared by them on the Bay of Bengal. Fish and other sea food such as crab and shrimp are in plenty in this region and so are the recipes. Rice is the staple food in Eastern India. The other characteristic features of coastal cuisines include the use of coconut in many recipes. Unlike other coastal kitchens, however, coconut oil is not commonly used. Instead, the preferred cooking medium is mustard oil or refined vegetable oil (mostly groundnut). Traditionally food was cooked on cowpat (made of dried cowdung), wood or charcoal fires but recent years have seen an emergence of gas, electric, and microwave ovens.
In terms of day-to-day cooking, Eastern Indians don't use many spices. The flavors are usually subtle, foods are delicately spiced unlike the fiery curries typically associated with Indian cuisine. The main seasoning is ‘Panch phutana’ (in Odia) or ‘Panch Phoran’ (in Bengali), which is a mixture of mustard seeds, coriander seeds, methi seeds, black coriander seeds etc. This mix is widely used for tempering vegetables and dhal/lentils, while garam masala, curry power, and turmeric are commonly used for non-vegetarian curries. The other major ingredient is garlic and mustard seeds finely ground together, called as Besara in Odia and Sorsho Bata in Bengali. Odias and Bengalis are rice eaters and along with rice, a typical Odia or Bengali meal has to have a combination of a stir fried or deep-fried vegetable; lentils; a mixed vegetable curry typically cooked with garlic and mustard paste or saag made from various green vegetables such as spinach or fenugreek and seasoned with paanch puoran; and of course, the ubiqitous Maccher Jhol or fish curry.
Odia and Bengali cuisine recognizes and gives a place for the five basic tastes of astringent, bitter, sweet, sour and hot. While the Odia meal does not have a specific course of serving the food items, an authentic Bengali meal does. It begins with bitters, either in the form of shukto (a kind of stew with vegetables, drumsticks or bitter gourd) and moves on in stages through the dhals with fries and fritters, a vegetable dish like a ghonto or chhokka, to the non-vegetarian items of fish or meat. Before ending on a sweet note, there is the occasional treat of astringent or sweet chutney.
Eastern Indian Diet: Odia & Bengali Cuisine
In general, Odia and Bengali meals include one or more of the following.
- Rice, white and parboiled (most commonly used). Rice is the staple food in Odisha and Bengal and is incorporated in many ways. For example puffed rice is used frequently for breakfast and snacks. Pakhala, a popular Odia dish consumed during the summer months, is made of cooked rice, water, and yoghurt.
- Rotis are consumed mostly at dinnertime or during breakfast.
- Dhals and legumes of various kinds. Most common dhals are toor, urad (especially to make cakes and snacks), gram and mung (most frequently used). Dhal is sometimes cooked with vegetables called “dalma.”
- Fish is an integral part of the diet. In fact it is considered auspicious, and no Odia and Bengali function can do without fish. The fish is prepared in innumerable ways – steamed or braised, stewed with greens or other vegetables and with sauces that are mustard based. Fish curry cooked with mustard and garlic paste is very popular. There is a preference for Hilsa fish followed by Bass, Mullet, Rohu and Katla (all are fresh water fishes). The delicious Dahi Macch is prepared with fried fish dipped in gravy made of curd.
- Mutton, chicken, and eggs, along with seafood are also used. The coastline offers an abundant variety of shrimps, lobsters, and crabs that are relished in a variety of cooking styles and often spiced up.
- Consumption of lamb and pork are not very common in Eastern India.
- Vegetables are consumed in different forms: stir-fried, sautéed, bhartha (pureed or minced vegetables), or curried with a paste of garlic, ginger, and onion. Fresh vegetables are often seasoned with light spices (Panch phoran or Panch Phutana). Often vegetables are cooked with fish, mutton, and chicken, especially in the curry form.
- Fruits are consumed fresh, mostly as after dinner desserts. These include watermelon, mango, lichees, apples, oranges, guavas, papayas, and a variety of plantains, and bananas.
- Tea is the most popular drink and is usually served with milk and sugar. Use of coffee is rare in the average households. Other popular drinks include coconut milk (from the young coconut, mostly a popular street-side drink), Lassi, a delicious iced curd drink, and Nimbu paani (lemon squash).
- Ghee is served on top of cooked rice to enhance flavor.
- Water is served with meals. For most traditional meals, people sit down on the floor on a mat and eat with their fingers.
- Coconut – is abundantly available and mostly used in the cooking (curries, dalma, sweets, chutneys) etc.
Sweets
People of Odisha and West Bengal are sweet lovers, and have always been known for their particular weakness for sweets. It is rare to see meals completed without sweets. The choice of sweets for Odia and Bengali meals are unlimited. From the ubiquitous mishti doi and rossogolla, to the rarer pithey and pulli, the choice is boundless. Certain sweets are made on special events. Use of chhana (reduced milk) for making sweets is honed to perfection. Rasgolla and innumerable varieties of sandesh are available today. Besides these the tradition of homemade pitha, and sweets made of rice powder, sweet potato, kheer, coconut and gur is still common.
Indian Foods: AAPI's Guide to Nutrition, Health and Diabetes
Meal Pattern for the Traditional Odia/Bengali Client with Type 2 Diabete
|
Time |
Typical |
Modified |
|
|
Calories : 3127 Carbohydrate : 445 grams (56%) Protein : 141 grams (18%) Fat : 87 grams (25%) |
Calories : 1852 Carbohydrate : 270 grams (58%) Protein : 98 grams (21%) Fat : 39 grams (19%) |
|
Breakfast (7:30 AM) |
§ 1 cup tea with whole milk and sugar § 1 cup chuda (puffed rice) upama |
§ 1 cup tea with skim milk (or 1% fat milk) and with no sugar (preferable). § 2 slices of whole wheat roti/ bread toast. § 2 table spoon of chutney § 2 tsp margarine |
|
Snack (10:30 AM) |
|
§ 3 graham crackers |
|
Lunch (12:00 noon) |
§ 3 cups of cooked rice § 2 oz of meat or fish § 1 cup of dhal § 1 cup of stir-fried vegetables § 2 table spoon of tomato/dhania chutney § ghee, pickles |
§ 1 ½ cups of cooked brown rice § ½ cup of dhal § 1 cup of stir-fried vegetables § 2 oz of fish (low fat) or meat (white, lean) § 1 cup low fat yogurt § 2 table spoon of tomato or dhania chutney (fresh) |
|
Afternoon tea and snacks (3:30 PM) |
§ 2 cups of Mudhi (puffed rice) and mixture (fried nuts and legumes) |
§ 1 fresh fruit |
|
Dinner (7:00 PM) |
§ 3 cups of cooked rice § 1 cup of dhal § 3 oz of meat or fish § 1 cup of stir-fried vegetables § 1 cup of curry (mixed vegetable and chickpeas). § pickles |
§ ½ cup cooked brown rice § 1 roti § 1 cup stir-fried vegetables § 2 oz of chicken or fish § 1 cup raw salad |
|
Snack (9:00 PM) |
|
§ 1 cup of skim milk |
Eastern Indian Diet: Odia & Bengali Cuisine
Some Examples of Healthy and Not so Healthy Foods:
|
Healthy Foods (use often) |
Not so healthy foods (use less often) |
|
Starches | |
|
Roti |
Parata fried with oil |
|
Plain brown/basmati rice (cooked) |
Pulao or fried rice w/ >1 tsp oil |
|
Roasted mudhi or chuda (puffed rice) |
Chuda upama with oil and vegetables |
|
Meat or meat alternatives | |
|
Dhal (mung, toor, or masoor) |
Dhal with lots of oil or ghee |
|
Baked Fish or Chicken |
Fried chicken or fish |
|
Pan-fried fish w/masala (cooked with oil and spices) |
Fried fish in tomato gravy |
|
Vegetable dishes |
|
|
Stir-fried vegetables |
Vegetable curry w/ lots of oil and spices |
|
Dalma (mixed Vegetable w/ dal) |
Dalma with coconut and ghee |
|
Dairy | |
|
Yogurt and buttermilk made w/ skim milk or 2% milk |
Yogurt and buttermilk w/ whole |
|
Raita made with low-fat milk |
Raita with fried boondi |
|
Rasgolla and other steamed desserts |
Desserts made with whole milk and or fried |
|
Fruit dishes | |
|
Plain fresh fruit |
Fruit salad with jaggery & nuts |
Weekend and Party Planning
Food plays an important role in social gatherings of Oriyas and Bengalis. Festivals and weekends are the time when people indulge in rich and high calorie food, alcoholic beverages, and soft drinks. Plan ahead and adjust your food intake for the whole day to avoid a heavy overload of carbohydrates and fats and protein. Request your host or the Restaurant to prepare 1-2 special or modified dishes for you!
Ranjita Misra, PhD, CHES, FMALRC is a Professor and Research Director, Center for the Study of Health Disparities, at Texas A&M University. She is also a member of the Intercollegiate Faculty of Nutrition at TAMU and a member of the Public Health Committee of AAPI. Contact information (979) 845-8726 or ranjitamisra@gmail.com
References
- Introductory Nutrition and Nutrition Therapy by Marian Maltese Eschleman. Lippincott Publishers, Philadelphia, 1996.
- "Bengali Cooking: Seasons and Festivals" by Chitrita Banerji. Published by Inbook.
- "The Calcutta Cook Book: A Treasury of Recipes from Pavement to Palace" by Minakshie Dasgupta. Penguin Publishers.
- "A Taste of India" by Madhur Jaffrey. Macmillan Publishing Company, Incorporated.
- "The Healthy Cuisine of India: Recipes from the Bengal Region" by Bharti Kirchner. Published by Lowell House, Los Angeles.
- http://hicalcutta.com/sutapa/recipes
Chapter 6
South Indian Cuisine
Nirmala Ramasubramanian, MS, RD, CDE
South Indian cuisine refers to foods from 4 states, namely Tamil Nadu, Karnataka, Andhra Pradhesh and Kerala; also included is Pondichery, which is a union territory. Variations in food practices along with language, culture, heritage and customs are very apparent among the 4 states. There are innumerable area- based specialty foods. For example, Pondichery cuisine is a blend of different cultures, including Tamil Nadu, Kerala and Andhra Pradesh while it also reflects the French influence. However, one may be able to find some common features.
In general, South Indian meals include one or more of the following in varied forms:
- Rice, white or parboiled. Since rice is the staple food of South India it is incorporated in various ways.
- Dhals or legumes of various kinds. Most common dhals are toor, urad, Bengal-gram and mung. The 2 staples, namely rice and different dhals are used in a variety of ways- pounded, ground, fermented, boiled, sautéed and so on. e.g. Idli, Dosa etc.
- Most commonly used animal protein foods are fish, chicken, lamb, mutton and eggs for non- vegetarians
- Vegetables, both green and starchy, are generally stir-fried or roasted to crispness (curry or porial) and/or served wet including dhals and coconut (koottu)
- Fruits are usually consumed fresh or as juices
- Desserts are generally made from reduced milk and white sugar (payasam or kheer), jaggery or brown sugar-based cooked rice and lentils (sweet pongal, appam,adirasam, jilebi), and other sweetmeats, using clarified butter, nuts and spices like cardamom (Kesari, Halwa etc).
- Ghee or clarified butter is served with rice as a flavor enhancer. Sesame, peanut and vegetable oils are generally used in cooking
- Salt served separately on the plate for optional use
- Pickles and pappads (crispy wafers) are often used as side dishes
- Water served with meals
- Hot beverages such as "milky" coffee or tea with sugar
- The most commonly used spices are coriander, asafetida, cumin seeds, fenugreek, ginger, pepper (red, green, and black), turmeric, saffron, cardamom and various combinations of these used as curry powders and dessert enhancers.
Shredded coconut, coconut oil, coconut milk, fried plantain chips and fish are more common in Kerala and Pondicherry, whereas spicier foods are popular in Andhra, including pickles and chutneys. Cereal- lentil preparations using oil or clarified butter are more common in Karnataka and Tamil Nadu.
Acculturation of Indians in America includes the selection of American or other ethnic foods as main meals or snacks especially by younger generation. e.g. Sandwiches, pizza, pasta etc. Additionally foods from other regions of India are commonly used by South Indians, e.g. puris, samosas, chapathis, etc.
South Indian Cuisine
Meal Pattern for the Traditional South Indian Client with Diabetes Type 2
|
Meal |
Typical |
Modified |
|
|
Total Calories : 3585 CHO : 525 gm (59%) Protein : 128 gm (14%) Fat : 107 gm (27%) |
Total Calories : 1905 CHO : 269 gm (55%) Protein : 88 gm (18%) Fat : 58 gm (27%) |
|
Breakfast 7:30 A.M. |
§ 1 cup coffee with whole milk § 3 Idlis or § 1 plate of Upuma § 2 tbsp. of coconut chutney |
§ 1 cup of coffee with ½ cup fat free or 1% milk § 2 Slices of whole wheat or multi grain toast § 2 tsp. of Margarine OR § 2 small Idlis OR § 1 cup of cracked wheat upuma § with 2 Tbsp. of tomato /veg or dhal chutney |
|
Snack 10:30 A.M. |
None |
§ 1 Fresh fruit (a small apple) § 8 oz. diluted buttermilk (½ cup lowfat yogurt and ½ cup water) |
|
Lunch 12:30 P.M. |
§ 3 cups of White rice § 1 cup Sambhar § 1 cup Rasam § 1 cup green plantain curry § 1 cup mixed veg. koottu § 1 cup curds/whole milk yogurt § 1 or 2 fried papadums or potato chips § 2 tsp ghee, § Pickles |
§ 1 ½ cups of Brown rice OR § 2 small rotis with ½ cup of brown rice § 1 cup Sambhar or dhal § 1 Cup Rasam § 1 cup green beans curry § Shredded Carrot Salad with lemon juice § ½ cup fat free yogurt § 1 small roasted pappad/appalam § 2 tsp oil in cooking |
|
Afternoon coffee 4 P.M. |
§ 2 murukkus/chaklis (pretzel like fried) § Coffee with whole milk |
§ ½ cup dry cereal mix (made with puffed rice, puffed wheat and ~6 peanuts or ~4 cashews) § 1 Cup coffee with fat free milk |
Indian Foods: AAPI's Guide to Nutrition, Health and Diabetes
|
Dinner 7:30 P.M. |
§ 3 cups of cooked white rice § 3 oz. of fish, chicken, or lamb (Non vegetarians) § 1 cup sambhar or dhal based vegetables § 1 cup fried vegetables such as Potato or Bhendi § 1 cup whole milk yogurt § Pickles/pappads etc |
§ 1 cup cooked brown rice or cracked wheat § 3 oz fish or white meat chicken (Non vegetarians) OR § 1 cup whole gram dhal or chick peas sundal § 1 cup spinach curry (dry or wet) § 1 cup Raita with grated cucumber (½ cup low fat yogurt and ½ cup cucumber) § 2 tsp oil in cooking |
|
Snack 9:30 P.M. |
§ 1 fresh fruit § 1 cup ice cream |
§ 1 Kiwi or small orange § 4 walnuts or 12 peanuts |
|
Healthy Foods (use often) |
Not-so heart healthy (use less often) |
|
Starches |
Starches |
|
§ Idli - steamed, low fat § Doas cooked with minimum oil § Uppuma made with cracked wheat § or Quinoa or Pohe |
§ Idlis topped with a lot of oil § Dosa roasts using extra oil or butter § Uppuma with liberal amount of oil or ghee |
|
Meat or meat alternatives |
Meat or meat alternatives |
|
§ Dhal or kootu or Sprouted mung dhal § Dhal Adais w/ controlled oil and veg. added § Chicken Tikka § Pan-fried fish w/masala |
§ Dhal with excess ghee or oil § Dhal Adais with excess oil § Fried chicken § Fried fish in coconut sauce |
|
Vegetable dishes |
Vegetable dishes |
|
§ Stir-fried green vegetables such as § cabbage curry/pallya § Mixed Vegetable kootu with § Minimal coconut |
§ Fried Potato curry with excess oil! § Aviyal with a lot of coconut, § Potato/Plantain |
|
Dairy |
Dairy |
|
§ Buttermilk made w/ skim or low fat milk § Pal kootu or Majjiga pulusu w/low-fat curds |
§ Buttermilk w/ whole or 2% milk § Pacchadi (Raita) w/fried boondi |
|
Fruit dishes |
Fruit dishes |
|
§ Plain fresh fruits § Plain Jack fruit or mango |
· Banana Panchamritham w/jaggery, ghee & nuts · Chhakkapradaman w/nuts/fruits |
South Indian Cuisine
Tips for changes
- Use brown rice instead of white rice. The increase in fiber content will improve glycemic control. There is a general misconception that diabetics must avoid all rice, which is not necessary. Avoiding excess portions is the key.
- Instead of using rice as the main staple grain, include a variety of grains such as cracked wheat, oats, barley, quinoa, ragi and other millets.
- Avoid washing rice several times before cooking or cooking in excess water and draining.
- Keep in mind that the recommended portions are for cooked products wherever applicable. e.g.1 Serving of dhal= 2 Tbsp of uncooked dhal 1 Serving of rice = 3 Tbsp. of uncooked rice. This is important because the finished product may vary greatly in quantity and consistency!
- Try to cook with minimum amount of oil. Preferred oils are olive, canola or peanut oils as they are high in monounsaturated oils.
- While using potato, green plantain or other starchy vegetables, remember to count them as carbohydrates and cut down on rice eaten at the same meal. Smarter thing would be to select green vegetables more often than starchy ones.
- Use green vegetables more freely and learn to cook them in small amounts of oil. Salads are good with every meal. Simple lemon and vinegar dressings may be freely used.
- Switch over to fat free, skim or 1% milk instead of whole milk. This will reduce the saturated fat and calorie content of the diet.
- Avoid fried snack foods as much as possible; learn to cook with recipes requiring dry roasting, baking etc. Remember people with diabetes are more susceptible to high cholesterol in their blood, as well as heart disease.
- Use lean cuts of animal proteins (meats/poultry) and use appropriate portion sizes. Avoid using more than 3 eggs per week. Egg whites are okay.
- Vegetarians may increase and improve the quantity and quality of protein by incorporating soy curd (tofu), soy flour, skim milk powder, nut butters and if allowed, egg whites.
- Pickles, chutneys, pappadums, etc. are very high in sodium. People with hypertension must take note that table salt, baking powder, and baking soda are sources of sodium and therefore must be used carefully.
- Desserts must be restricted to allowed quantities of fresh fruits. Artificially sweetened low fat desserts or desserts using allowed foods with minimal amount of real sugar may be used with prudence.
- Drink plenty of water throughout the day, at least 6 to 8 cups a day.
- Learn to read the nutrition labels on food packages.
Weekend and Party Planning
South Indians are very similar to other immigrants in trying to entertain and relax on the weekends. Food becomes an important part of the social gatherings. Quite often, festivals and holidays are celebrated on the weekends with friends. Pot-luck dinners are very popular. Men may indulge in alcoholic beverages while women generally limit themselves to sodas and juices.
Party meals consist of several varieties of rice, vadas, and bondas as well as fried and creamy vegetables prepared with liberal quantities of oil and coconut, nuts and dry fruits. Fried home made rice/lentil snacks, roasted nuts, potato chips, rice and lentil wafers, and chutneys make the feasts mouth watering and of course calorie-laden! Special desserts of various kinds appropriate to the festival/celebration are also brought in, in addition to cakes and doughnuts to satisfy the palate of the younger generation.
Indian Foods: AAPI's Guide to Nutrition, Health and Diabetes
Party Tips
- Try to eat a sensible, small snack, like a bowl of soup, before leaving the house, to curb overindulgence.
- With appetizers, use a small plate, fill it with healthy snacks, and limit the number of fried snacks.
- Drink seltzer with lime/lemon for a splash of flavor, without the calories of juice, soda or alcohol.
- When dinner items are served, survey all the offerings first, and envision your plate accordingly: ½ salads and green vegetables, ¼ rice/breads, ¼ chicken, fish or other protein.
- Take the time to enjoy your food and refrain from going back for seconds.
- When choosing desserts, be very sensible. Choose fruit.
Hosting the party or festival
- When hosting, offer fresh, colorful veggies (baby carrots, cucumber strips, bell pepper strips, cauliflower florets) in lieu of,or in addition to fried snacks. Serve the veggies with coriander chutney or a low-fat yogurt-based dip.
- Try to offer 1 or 2 vegetable dishes, lightly stir- fried or steamed, and a healthy salad. Ensure that your guests have good, healthy options.
Nirmala Ramasubramanian, MS, RD, CDN, CDE has extensive experience in acute care dietetics and clinical research of diabetes. She is presently employed at North Shore University Hospital/Healthcare System in Manhasset, New York. Contact information 718-969-1827 or nirmala1@gmail.com
References
- India & Pakistani Food Practices, Customs, and Holidays. American Dietetic Association. American Diabetes Association Inc.
- Chandra Padmanabhan. DAKSHIN: Vegetarian Cuisine from South India, Angus & Robertson Publishers.
Chapter 7
Maharashtrian Cuisine
Keya Deshpande Karwankar, MS
Maharashtrian cuisine boasts of being wholesome, nutritious and intricate. You would find one ingredient like dal could be made in three or four elaborately different ways. The cuisine encompasses a variety of food preparations, from the coconut based coastal cuisine to an interior distinctive cuisine known as Varadi cuisine. Although, all the them share a lot of commonalities:
Grain Group
Examples of one serving size would be: 1 chapati, ½ cup of cooked rice, ½ cup of pohe.
- As in most of the other states of India, rice is the staple food grain in Maharashtra too. A maharashtrian meal cannot be complete without chapati or bhakri (jawar or bajra roti) with toop (clarified butter-ghee).
- Breakfast comprises of preparation like pohe(seasoned beaten rice).
- Desserts or sweets like sheera (sweet semolina), kheer, shankarpaali (made out of refined flour and sugar) are common. And special occasions call for puris (deep fried) or one of the most liked maharashtrian dish called puranpoli (chapati with a lentil and jaggery filling).
Vegetable Group
Example of a serving size would be ½ cup of cooked vegetables and 1 cup of raw vegetables, like spinach.
- There is an enormous variety of vegetables in the regular diet made in both gravy and dry style. Curries like bharlivangi, bharlibhendi are made on special occasions.
- The vegetables are more or less steamed and lightly seasoned so as to retain their nutritional value. Deep frying and roasting is not a common practice. And few of the common dishes are bharit (lightly cooked or raw vegetables in yogurt), paale bhaji (leafy vegetables), paatal bhaji (spinach or fenugreek with lentil and peanuts), zunka (made with gram flour and vegetable).
- Salad or koshimbir is a very important part of every meal. It is made out of a variety of raw vegetables like cucumber, tomatoes, onions, spinach. And this is garnished with coriander and peanut powder, and is lightly seasoned with phodni (hot oil with spices).
Fruits Group
Example of a serving size would be a tennis ball size of apple, a medium banana, ½ cup of aam ras.
- Fruits are consumed both whole and pureed. Aam ras (mango puree) and shikran (banana in milk) are commonly consumed. And in summer pana (raw mango juice) is relished.
- (Pureed ,sweetened fruits carry concentrated calories and adjustments have to be made accordingly to avoid a high sugar load at any one meal).
Milk/Yogurt Group
- Example of a serving size would be 1 cup of milk, ½ cup of yogurt, 1 cup of butter milk.
- Milk is used in the preparation of tea and many of the sweet preparations like kheer.
Indian Foods: AAPI's Guide to Nutrition, Health and Diabetes
- Yogurt is a very vital ingredient in preparing koshimbir, bhajis (vegetables), chutney (spicy accompaniment made out of a variety of foods) and it is also used to make a famous maharashtrian dessert, shrikhand (Curd whey with sugar).
- Taak (buttermilk) and yogurt is also eaten with rice. Buttermilk is also used to make taaka chi kadi (buttermilk with gram flour).
Meat, Poultry, Fish, Dry beans/Lentils, Eggs and Nuts Group
- An example would be ½ a cup of dal, ½ cup of chicken or mutton curry.
- Dal (Toor dal) or umpti (sweet and sour toor dal) are a must with rice for a maharashtrian. A variety of lentils like masoor, chana, toor, mung are used in the preparation of varan (dal).
- Mooga chi dal (mung dal) , mooga chi usal , vatana chi usal (dried peas) are also the delicacies. Sprouted mung dal is used widely and is prepared in many different ways.
- Peanuts are used in a lot of preparations like chutney, chikki (peanut and jaggery), and it is used as garnish for many of the koshimbiri and bhaji.
- The people in the coastal parts of maharashtra enjoy a variety of fish like bombil (bombay duck), which is batter fried, bangda (mackerel) is curried with red chilles, ginger and tirphal (a spice). Paaplet (pomphret) is usually barbecued or shallow fried.
- Lamb and chicken is mainly consumed in the interior part of maharashtra.
- Foods in this group are excellent sources of proteins, B vitamins, iron and zinc. Lentils/ dals are also a good source of fiber.
Food preparations during upaas (fast)
Fasting time actually turns out like a feast, as maharashtrians prepare numerous dishes garnished with peanuts. Sabudana chi khichadi, sabudana wada (a deep fried snack) bagaar (a type of rice), batata cha khees (grated potato-seasoned) are the hot favorites during fasting.
Jaggery, tamarind and kala masala (is a special blend of spices) is added in most of the vegetables and lentils which makes the foods piquant .
Although maharashtrians usually tend to stick to the traditional cooking style, maharashtrians in America have incorporated a tad of western cooking, making it a nice blend of both.
One Day Menu Plan for a Traditional Maharashtrian Client with Type II Diabetes
|
Meal |
Typical |
Modified |
|
|
Calories : 3402 Carbohydrate : 462 grams (54%) Protein : 114 grams (13%) Fat : 130 grams (33%) |
Calories : 2048 Carbohydrate : 326 grams (64%) Protein : 102 grams (19%) Fat : 40 grams (17%) |
|
Breakfast: 8.30 AM |
§ 1 cup chaha (tea) with whole milk and sugar. § 1 bowl pohe. § 1 banana |
§ 1 cup chaha made out of skimmed milk and sweetener. § 1 cup of pohe. § 1 apple. |
Maharashtrian Cuisine
|
Meal |
Typical |
Modified |
|
Lunch: 12.30 PM |
§ 2 cups white rice § 2 chappatis with oil or ghee § 1 cup umpti (toor dal with jaggery and tamarind) § ½ cup batata chi bhaji (Potato curry). § ¼ cup cucumber koshimbir (salad) with peanut powder and phodni. § 1 cup yogurt or buttermilk. |
§ ½ cup brown rice § 2 phulkas without oil or ghee § 1 cup varan (toor dal without jaggery). § ½ cup string beans bhaji or 1 cup methi chi bhaji (fenugreek curry). § ¼ cup cucumber koshimbir without peanut powder or phodni. § ½ cup non-fat yogurt or buttermilk. |
|
Snack: 4.00 PM |
§ 1 cup chaha (tea) with whole milk and sugar. |
§ 1 cup chaha made out of skimmed milk and sweetener. § 2 whole wheat crackers. § ½ cup watermelon. |
|
Dinner: 8.00 PM |
§ 1 cup white rice. § 2 chappatis with oil or ghee. § 1 cup mooga chi usal (mung dal) with fresh grated cocunut. § 1 serving of fried fish. § 1 cup kokum kadi (kokum fruit in coconut milk) |
§ ½ cup brown rice. § 2 phulkas without oil or ghee. § 1 cup mooga chi usal (mung dal) without coconut. § 1 serving barbecued fish (with very little oil). § 1 cup kokum juice without coconut milk or ¼ cup kokum kadi with coconut milk. |
Weekend and Party Planning
Weekends are usually spent with friends and relatives and food becomes a major part of the good times. Presentation of food has a lot of importance for Maharashtrians. Party favorites include a different type of rice preparation like vaangi bhaat (brinjal rice), tondli bhaat (tindora rice). Fried snacks like chewda (made out of beaten rice), chakli (deep fried, made out of gram flour) are often served. Shrikhand (curd whey and sugar), aamrakhand, or kheer are served as desserts.
Keya Deshpande Karwankar, MS is Senior Manager of Operations and Quality at Apollo Health and Lifestyle Limited in Hydrabad India. Contact information keyakarwankar@gmail.com.
Macronutrient calculations were done by Anwar Al- Mansoor, MPH Nutrition candidate, Hunter College, New York. Contact information anwar.almansoor@gmail.com.
Chapter 8
Gujarati Cuisine
Rita Batheja, MS, RD, CDN
Gujarati Cuisine is primarily vegetarian with Jain and Buddhist influences. Gujarat can be divided into 4 regions and due to the different climatic conditions; there are slight variations in eating habits and preparation of food. The four regions are South and North Gujarat, Kathiavad and Kutch. Gujaratis have a sweet tooth and therefore add jiggery and/or sugar to every dish from vegetables to chutneys including dal and pickles. Jains do not eat onion and garlic. Rotli is prepared soft like a petal, Phulkas to a crunchy bone dry texture called Khakhras. Khakhras are used for breakfast or as a snack or while travelling.
South Gujarat
In Surat, vegetable dishes like Undhiyu and Paunkh are very popular. Suratis add green chilies to add life to the food. They love sweets like Nankhatais and Gharis which they buy from local bakeries and shops. No expensive ingredients are used or elaborate preparations are made yet food in its simplicity tastes exotically different.
North Gujarat
Food is non-spicy and oil is used sparingly. It is popular for its traditional Gujarati Thali, which has its origins in this city. It consists of Farsan (appetizer) like Khaman Dhokla and Khandvi (chickpea flour), one variety of Dal or Kadhi (prepared from yogurt), hot fluffy Puri or Rotli, couple of vegetables, sprouted beans, Raita (yogurt), Doodhpak (sweetened milk with saffron and nuts), Papad, Chutney and Pickle.
Kathiawad
Kathiawadis love Dhebras (made from wheat flour, yogurt, spinach, green chilies, sugar and salt) that they eat with Chhunda (sweet, sour and hot mango pickle). They also use Methia Masala (dry powder made from fenugreek seeds, chili powder and salt) to sprinkle on vegetables. They also use red chili powder to make spicy cuisine and eat lot of peanuts and til (sesame seeds) – Peanut Chiki (made with gud) tastes delicious.
Kutch
Kutchi cuisine is very simple. They mainly use rice and pulses. Main dish is Khichdi (mixture of rice and mung dal) and Kadhi (curry made of yogurt) or Bajra no rotlo (made from Millet) with homemade pure ghee (butter) and gud (jaggery), guvarnu shak (vegetable) and Chhash (buttermilk). Kutchhis also eat Dudhi Muthia (made from Snake Squash and flour) and some common dishes like Dhokla (a salty steamed cake), Doodhpak or Shrikhand (sweet made of Whoe Milk Yogurt, Cardamom, Slivered Pistachio/ Almonds, Saffron and Charodi) with hot fluffy puris.
In short, Gujarati Cuisine’s concentration is on fried snacks and the use of plenty of ghee, oil, sugar and jaggery. Many Gujaratis do not eat green vegetables frequently and hardly eat fruits.
Gujarati Cuisine
|
Meal |
Typical |
Modified |
|
|
Calories : 4244 Carbohydrate : 606 grams (57%) Protein : 99 grams (9%) Fat : 161 grams (35%) |
Calories : 1531 Carbohydrate : 247 grams (65%) Protein : 70 grams (18%) Fat : 37 grams (22%) |
|
Breakfast 7:30 am |
§ 1 cup Chai (Tea) with whole milk § 4 tsp regular sugar § 2 –3 Theplas |
§ 1 cup Chai with 1% milk § 1 package – no calorie sweetner § 1 Thepla or 2 plain Khakhras § ¾ cup 1% Milk § 1 cup Water |
|
Snack 10:30 am |
§ 30 Salted Peanuts |
§ 10 unsalted roasted peanuts § 1 cup Water |
|
Lunch 12:30 pm |
§ 4 Rotlis with 4 teaspoons ghee § ½ cup Toor Dal with sugar § 1 cup Black eye peas with sugar § 1 cup Bhat (rice) § ¼ cup Yam § ¼ cup Dahi (yogurt) § 1 cup regular soda § 1 tsp vegetable oil in cooking |
§ ½ cup Salad with lemon and vinegar § 1 Sooki Rotli – no ghee § ½ cup Toor Dhal no sugar § ¼ cup Black eye peas no sugar § ¼ cup Bhinda nu Shak (Okra veg.) § ¼ cup Bhat (cooked rice) § ½ cup Dahi (1% milk) § 1 small apple § 1 cup Water § ½ tsp olive oil in cooking |
|
Tea Time 3:30 pm |
§ 1-2 cup Chai with 1 oz whole milk § 4 tsp regular sugar § 1 cup Fried Chevda § 1 ½” x 1 ½” Mohanthal (sweet) |
§ 1 cup Chai with 1oz 1% milk § 1 pkg – no calorie sweetener § ¾ cup homemade high fiber high protein or high fiber cereal Chevda § 1 cup Water |
|
Dinner 8 pm |
§ 1 Fried Papad § 3 Parathas with 6 tsp oil § 1 cup Batata nu shak (Potato veg.) § 1 cup Chhash (Buttermilk) § 2 1” Mug-ni dal ni Kachori with Amali-ni chutney § 2 Tbsp Chhunda (mango pickle) |
§ ½ cup Salad with Balsamic vinegar § 1 Paratha with ½ tsp oil– use non-Stick pan. § ½ cup Palak with 1% lowfat Paneer or Extra firm silken Tofu § ½ cup 1% Dahi (yogurt) § 1 medium Orange § 1 cup Water |
|
Snack 9 pm |
§ 6 Khajur (Dried Dates) § 1 oz bag Potato chips § 1 cup water |
§ 3 Khajur (Dried Dates) § 6 Almonds § 1 cup Water |
Indian Foods: AAPI's Guide to Nutrition, Health and Diabetes
Weekend and Party Plannig
Gujaratis love weekend gatherings and partying, which starts from Friday evening till Sunday evening. Mostly men drink few pegs of scotch with snacks such as kachoris, samosas, vegetable cutlets, cashew rolls and varieties of Bhajias. Problems in this area that call for your attention before you go to that party or the restaurant: Remember PORTION CONTROL and move more eat less that makes perfect sense. Plan your day’s meal ahead of time so that importance is given to healthful preparations, the kind and amount of fat used and the importance of avoiding carbohydrate or fat loading.
Party meal consists of
Fried Papad, Puries, Shrikhand (rich sweet made from whole milk yogurt, sugar, Cardamom, Slivered Pistachio/Almond, Saffron and Charodi ) Valor nu shak (pulses or legumes),Undhiyu (mixed vegetables, potato, flour ball – muthias swimming in oil), Vegetable Pulao, Kadhi (made with buttermilk), Raita, Kataki ( cubed mango pickle).
It is recommended that to go easy on appetizers,offer variety of sliced vegetables with Humus (Mediterranean dish) as an example. Humus is made from ground chick peas, sesame paste (Til- high in calcium), green chillies, ginger and lemon (easy recipe – can keep in the refrigerator).
Consider serving Handva, Dhokla and Idli instead of fried items. Example 1” square Dhokla = 1 Rotli,½ cup Pauva = 1 Rotli, got the idea! That is called carbohydrate counting. Dairy, vegetables, fruit and food from the grains group all contain carbohydrate. Consumers with Diabetes need to learn about serving sizes.
Modified Party Meal
- ½ cup lettuce and tomato salad
- 1 teaspoon fat free salad dressing (Walden farm brand tastes good)
- 1 3” Puri
- ⅓ cup Undhiyu
- ¼ cup Kadhi
- ¼ cup Vegetable Pulao
- 1 small oven baked Samosa
- 1 oz. Shrikhand
- ¼ cup fresh fruit salad
|
Eat Frequently |
Eat Infrequently |
|
Dairy | |
|
§ 1% or 2% Milk § Dahi made from 1% or 2% Milk |
§ Regular Milk § Dahi made from regular Milk |
|
Meat or Meat Alternatives | |
|
§ Black eye peas with no calorie sweetener § Roasted Papad |
§ Black eye peas with sugar § Fried Papad |
|
Vegetable | |
|
§ Palak vegetable with 1% low fat paneer or § Extra firm Silken tofu § Bhinda (Okra) Nu Shak |
§ Batata Nu Shak § Mashed Yam |
|
Fruit | |
|
§ Grapes § Fruit Shrikhand made with 1% Dahi |
§ Mohanthal § Shrikhand made from Whole Milk Dahi |
|
Grain | |
|
§ Home made high fiber cereal (Chevda) § Paratha with 1 tsp olive oil – use non stick pan |
§ Fried Chevda § Paratha with 1 tablespoon cotton seed oil |
Gujarati Cuisine
Rita (Shah) Batheja, MS RD CDN is an Internationally Renowned Registered Dietitian and Integrative Nutritionist in Private Practice in Long Island, New York and the Founder of the Indian American Dietetic Association. Contact information 516-868-0605 or krbat1@juno.com.
Macronutrient calculations were done by Anwar Al- Mansoor, MPH Nutrition candidate, Hunter College,New York. Contact information anwar.almansoor@gmail.com.
References
- Ethnic and Regional Food practices, a series Indian and Pakistani food practices, customs and Holidays, 2nd edition – American Dietetic Association. American Diabetes Association,Inc.
- Little India, December 1996 Vol. No. 12 “Affairs of the Heart – Health Watch.
- Practical Management of Diabetes – 2nd edition.Sharad Pendsey, MD – Diabetes Clinic and Research Center, Nagpur, India.
Chapter 9
North Indian Cuisine
Madhu Gadia, MS, RD, CDE
North Indian cuisine typically represents foods of Punjab, Haryana, Delhi, Jammu and Kashmir, Himachal Pradesh, Uttar Pradesh, Uttarakhand, Rajasthan, Bihar, Jharkhand, Chhattisgarh, and Madhya Pradesh. Basically, all the states north and west of Maharashtra are often clumped together in this generalization. Each state has its own specialties but it is the similarities that classify the food of this region. North Indian food is often called “Punjabi food”. North Indian food is the most popular food in restaurants and therefore it is synonymous with Indian food throughout the world.
Wheat is the staple food of this region. “Basmati” rice is grown in the northern plains and is often the rice of choice for pulaos and biryanis. Variety of dals or beans such as garbanzo, kidney, urad as well as moong and toor dal are used. Milk, butter and ghee are used extensively. Chicken and mutton are the most popular meats eaten in this region. Most of the cooking is done on the stovetop using the roasting and frying method.
Punjabis and refugees from West Punjab (which is now in Pakistan), came and settled in Punjab and Delhi. They were very enterprising people and had a style and food of their own. They popularized tandoori food (that gets its name from the tandoor clay oven in which the food is cooked) in this region. Punjabis opened restaurants at every corner and thus tandoori food was born. They developed a ‘formula’ that worked and Punjabi food became very popular. Today most Indian restaurants around the world serve tandoori dishes and typically Punjabi food.
North Indian food is a combination of simple to very elegant vegetarian and non-vegetarian fare. A simple vegetarian meal may consist of moong dal, subji and phulka (thin whole wheat roti). The food is seasoned with asafoetida, cumin, turmeric, coriander powder and garam masala. The garam masala is often referred to as a north Indian spice blend. Onion and garlic may or may not be used. Then there are the non-vegetarian favorites like chicken and lamb dishes heavily seasoned with spices, onion, ginger and garlic. Foods like stuffed paratha, saag and makki-ki-roti (corn roti), chole and bhature, kofta, rogan josh, tandoori chicken, biryanies and pulao are very popular in this cuisine. Variety of desserts such as barfi, laddu, and gulab jamun are extremely popular in this region.
North Indian food is often described as “rich”. The food is often fried, and a fair amount of ghee, butter and nuts may be is used. The food is seasoned heavily with onion, ginger, garlic and spices like cardamom, cinnamon and cloves that give the food a “rich” color and flavor.
Nutritionally speaking, north Indian meals with plenty of whole grains, green leafy vegetables, and beans are high in complex carbohydrates, fiber, vitamins and minerals. The overall fat and saturated fat content of traditional meals may be high due to extensive use of milk, butter, ghee and oil. The meal can be easily modified in overall fat content by using small amount of unsaturated oil to season the food. In order to reduce saturated fat, substitute low fat or fat free milk wherever possible and use butter and ghee sparingly.
North Indian Cuisine
North Indian food can be easily incorporated into a healthy lifestyle. If you have diabetes, it is important to watch the carbohydrate content of each meal. Plan balanced meals of roti, dal, meat (if non- vegetarian) non-starchy vegetables and salad. A typical ‘thaali’ meal (pre-portioned out foods in small cups served on a large plate or ‘thaali’) with balance of nutrients, flavors and textures may work well with diabetes and a healthy diet. The amount of carbohydrate in each meal should be individualized. Portion size of foods is important to determine the actual carbohydrate intake. Remember within reason most foods can fit into a diet for a person managing his/her diabetes. See sample menu below.
Sample Menu
A sample menu of a typical vegetarian (and non- vegetarian meal) and a modified meal plan is given below. A typical meal as mentioned earlier is high in carbohydrate and fat. By some modification in the amount of oil and ghee used, substituting low fat and low
carbohydrate vegetables as well as cutting down on portions will help in cutting down in carbohydrate and fat content and therefore the total calorie intake. The recommendations for a well-balanced meal plan are carbohydrate 50 to 70 percent, protein 10 to 20 percent, and fat 30 to 35 percent. Consult a dietitian for an individualized meal plan.
Table below identifies foods to eat often and foods to eat less frequently
|
Food Groups |
Eat More Often |
Avoid or Eat less often |
|
Starches |
§ Roti, phulka, chapatti § Brown basmati rice § Potatoes-prepared with minimal oil |
§ Paratha, puri, kachori, naan § Pulao, Biriyani § Fried potatoes |
|
Fruits |
§ All fresh fruits § Monitor portion size of fruit § Light canned fruit |
§ Regular canned fruit |
|
Vegetables |
§ All vegetables cooked with minimal oil |
§ Creamed or fried vegetables |
|
Meat And Meat Alternatives |
§ Dal cooked in minimal oil § Chicken (without skin) and fish cooked in minimal oil § Eat lean lamb, goat, pork or beef less often and in small quantity § Low fat cheese § Low fat paneer § Part skim Ricotta cheese § Tofu |
§ Fried or creamed dal § Chicken, fish, or red meat cooked with cream § High fat cuts of lamb, goat, pork or beef § Regular Cheese § Regular paneer § Regular Ricotta Cheese |
|
Dairy |
§ Skim milk, fat free yogurt and buttermilk |
§ 2% or whole milk and its products |
|
Fats |
§ Canola, vegetable, or olive oil § Nuts such as almonds, peanuts, walnuts § Seeds such as sunflower seeds |
§ Butter, ghee, cream, half- and- half Coconut, coconut oil, coconut milk |
Indian Foods: AAPI's Guide to Nutrition, Health and Diabetes
Menu Plan for a Traditional North Indian with Type II Diabetes
|
Meal |
Typical Meal |
Modified Meal | ||||
|
|
Calories Carbohydrate Protein Fat |
: : : : |
2600 350 grams (55%) 80 grams (12%) 100 grams (33%) |
Calories Carbohydrate Protein Fat |
: : : : |
1600 220 grams (55%) 70 grams (17%) 50 grams (28%) |
|
Breakfast |
§ 1 cup çhai (Tea) / whole milk § 3 teaspoons sugar § 1 potato paratha 1 tsp Pickle |
§ 1 cup çhai / skim milk § no calorie sweetener § 2 whole wheat toast § 1 teaspoon butter § 1 cup skim milk | ||||
|
Lunch |
§ 2 roti with 1 teaspoon ghee § 1 cup rajmah (or chicken curry) § ½ cup spinach and potato subji § ½ cup onion and cucumber salad § 1 roasted papad |
§ 2 roti-no ghee § 1 cup low fat rajmah (or low fat chicken curry) § ½ cup spinach subji § ½ cup onion and cucumber salad § 1 roasted papad | ||||
|
Tea Time |
§ 1 cup chai / whole milk § 3 teaspoons sugar § ¼ cup namkeen (fried snack) § 1 laddu (sweet) |
§ 1 cup chai / skim milk § no calorie sweetener § 1 oz (30grams) mixed nuts § 1 Banana | ||||
|
Dinner |
§ 2 parathas § 1 cup chole (1 cup Kheema) § 1 cup potato and pea subji § ½ cup dahi (whole milk yogurt) |
§ 2 roti-no ghee § ½ cup chole (or ½ cup low fat kheema) § 1 cup cauliflower subji § ½ cup dahi (fat free) | ||||
|
Snack |
§ 1 cup Kheer |
§ 1 orange § 1 cup skim milk | ||||
Weekends and Parties
There is often a distinct difference in our eating between weekdays and weekends. Weekdays we are bound by time and schedules and it is easier to control the types and amounts of foods we eat. People will often say they do so well Monday to Friday implying that they make good choices in their meal selection. But come weekends (starting Friday night) we lose all restraints in our food selection. Indians love to party, as it is our way of socializing and connecting with our culture. Socializing is associated with special occasion foods of puri, chole, pakore, and not to mention kheer and halwa (generally high-fat foods). Portion control is a good tool to use here. If you are the host, plan your parties to balance meals and incorporate some lower fat foods like vegetable trays as appetizers and use less fat in your dishes. If you are the guest at a party and everything you see is high in fat and calories watch your portion sizes, enjoy the company and thank the hosts for a wonderful evening. You will be much happier on Monday morning!
North Indian Cuisine
|
Typical Party Menu |
Serving Suggestions (Watch portions and total carbohydrate intake to avoid elevated blood sugar after the meal, and enjoy the party and company.) |
|
§ Samose or pakore with chutney § Puri § Chole § Chicken curry (non-vegetarian) § Potato Pea subji § Cauliflower with potato subji § Kofte § Onion, cucumber, radish salad § Boondi Raita § Matar Pulao § Chai § Gulab Jamun |
§ 1 Samosa § 1 Puri § ½ cup Chole § ½ cup Chicken curry (non-vegetarian) § ½ cup Cauliflower subji, avoid the potatoes § 1 kofta § 1 cup onion, cucumber, radish salad § ¼ cup Raita § Chai § (Skip pulao and dessert) |
Madhu Gadia, MS, RD, CDE (Registered Dietitian and a Certified Diabetes Educator) is an author of New Indian Home Cooking (Penguin Group 2000) and The Indian Vegan Kitchen (Penguin Group 2009). She is a Wellness Director for Compass Group and teaches the art of Indian cooking around the country. Contact information www.cuisineofindia.com.
References
- Exchange Lists for Meal Planning, American Dietetic Association, 1995.
- The Indian Vegan Kitchen: More Than 150 Quick and Healthy Homestyle Recipes; Madhu Gadia, M.S., R.D., 2009.
- New Indian Home Cooking: More than 100 delicious, nutritional and easy low fat recipes!; Madhu Gadia, M.S, R.D., 2000.
Chapter 10
Nepali Cuisine
Suraj Mathema, MS, RD, CDE
Many people of Nepalese origin following Nepali dietary practices live in India. Nepali cuisine, in part, has been influenced by cooking practices in North India and Tibet. But, there are many typical indegenous dishes such as gundruk, lapsi achar, qua gasa (Newari dish), sukti etc. Also, the sub-ethnic groups have their own variations of dishes.
In general, Nepali meals include one or more of the following in varied forms:
- Rice is most popular in grains, then wheat. Maize is not as popular as rice and wheat. Even less popular are millet, barley and buckwheat
- Dals or legumes of various kinds. Most common dals are toor, urad, gram and mung. The two staples, namely rice and different dals are used in a variety of ways such as pounded, ground, boiled, sautéed and so on.
- Most commonly used animal protein foods are, chicken, goat, water buffalo and eggs for non- vegetarians
- Green vegetables are stir-fried, while most other vegetables are seasoned with light spices and prepared in curry form.
- Fruits are usually consumed fresh or as juices.Lapsi is typically eaten as achar.
- Commonly consumed sweets are: Kheer, Gulaab Jaamun, Halwa, Mahi (by product of milk after the butter had been churned out, often sweetened before consumption), Rasogolla, Rasmalai, Laddoos etc.
- Hot tea is most popular drink for all seasons. It is served with milk and sugar.
- Ghee or clarified butter is often served with rice as flavor enhancer. Mustard oil is mostly used for cooking.
- Water served with meals
- The most commonly used spices are coriander, cumin, ginger, turmeric. And others used in typical dishes are timur (szechwan pepper – used in aloo achar, qwa gasa etc.), jimbu ( used in urad dal)
Heart Healthy Meal Pattern for the Traditional Nepali Client
|
Time |
Typical |
Modified |
|
|
Calories : 2800 Carbohydrate : 336 grams (48%) Protein : 140 grams (20%) Fat : 99.5 grams (32%) |
Calories : 1900 Carbohydrate : 261 grams (55%) Protein : 119 grams (25%) Fat : 42 grams (20%) |
|
Breakfast (7:00 AM) |
§ 1 cup tea with whole milk and sugar § 2 slice bread § 1 egg |
§ 1 cup tea with skim milk (or 1% fat milk) and with no sugar (preferable). § 2 slices of whole-wheat bread/ toast. § 2 tsp margarine |
Nepali Cuisine
|
Snack/Lunch1 (9:30 AM) |
|
§ 1 fruit, 3 graham crackers |
|
Lunch/Snack (1:00 PM) |
§ 2 cups of rice2 § 2 oz of meat/chicken § 1 cup of dal § 1 cup of stir-fried vegetables § 2 table spoon of tomato/coriander chutney § Ghee, pickles |
§ 2/ cup of brown rice 3 § ½ § 1 cup of dal § 1 cup of vegetable curry § 2 oz of Chicken (skinless) or meat (white, lean) § 1 cup low fat yogurt § 2 table spoon of tomato or coriander chutney (fresh) |
|
Afternoon tea and snacks (4:00 PM) |
§ 1 cup of Chiura (beaten rice) § 1 cup fried vegetable § 1 cup tea |
§ ½ cup Chiura or § 3 saltine-type crackers or § 10 unsalted roasted peanuts and § 1 cup tea with low fat milk without sugar. |
|
Dinner (7:00 PM) |
§ 2 cups of rice § 1 cup of dal § 3 oz of meat or Chicken § 1 cup of stir-fried vegetables § 1 cup of curry (mixed vegetable and chickpeas). § Pickles |
§ 2/3 cup brown rice § 1 cup stir-fried vegetables § 1 cup mixed vegetables with chickpeas. § 1 cup dal or § 3 oz of skinless chicken or Fish § ½ cup salad |
|
Snack (9:00 PM) |
|
§ 1 fresh fruit § 1 cup of skim milk |
Many Nepalese following traditional meal time eat Lunch at about 9:00 AM and snack at 1:00 PM 2 Rice refers to cooked rice wherever mentioned in this article
Tips for changes
- Encourage brown rice instead of white rice.
- Instead of using only rice, select from a variety of grains, such as cracked wheat, oats, and barley.
- Avoid washing rice several times before cooking or cooking in excess water and draining. Doing this may lose valuable vitamins and enriched iron.
- Keep in mind that the recommended portions are for the cooked product where applicable
- Try to cook with minimum amount of oil, preferably olive oil or canola oil which are high in monounsaturated fats.
- While using potato, or other starchy vegetables, remember to propotionately cut down on the amount of rice eaten. Smarter thing to do is selecting a green vegetable more often than starchy ones.
Indian Foods: AAPI's Guide to Nutrition, Health and Diabetes
Some examples of Heart-healthy and Not So Heart-healthy foods:
|
Food Groups |
Heart-healthy |
Not so Heart-healthy (use less often) |
|
Starches |
Plain rice, plain roti |
Fried rice, fried potato |
|
Meat and Meat Alternatives |
Dal, skinless chicken |
Fried Dal, chicken with skin |
|
Dairy |
Skim milk, low fat yogurt |
Regular milk, yogurt with extra cream |
|
Vegetables |
All vegetables with no more than one teaspoon of oil per ½ cup cooked vegetable |
Fried vegetables, creamed vegetables |
|
Fat/oils |
Margarine, canola oil |
Butter, coconut oil |
7. Use green vegetables more freely and learn to cook them in a small amount of oil. Salads are good with any meal. Simple lemon or vinegar dressings may be freely used.
8. Switch over to skim or 1% low fat milk instead of whole milk. This will reduce the saturated fat content in the diet.
9. Avoid frying of snack foods; learn to look for recipes, requiring dry roasting, baking etc. Remember people with diabetes are more susceptible to high cholesterol in their blood and heart disease. Practice low fat cooking methods, using non-stick pans.
10.Use only lean cuts of animal proteins and practice correct portion sizes. Avoid using more than 3 whole eggs/week. Egg whites are okay.
11.Pickles, chutneys etc are very high in sodium. People with hypertension must take note that table salt, baking powder, and baking soda are sources of sodium and therefore must be used carefully.
12.Desserts should be restricted to fresh fruits; artificially sweetened low fat desserts made from allowed foods may be used occasionally.
13.Drink plenty of water, at least 6 to 8 cups a day.
Weekend and Party Planning
Food plays a major role during the weekends and the social gatherings. Nepalese tend to live in an extended family environment. As a result, members of the family constantly get in and out of the house at different times. Thus, food is constantly being prepared to ensure that nobody remains hungry including the guest that come unannounced, which is a common event. Most Nepalese prefer to eat home cooked meals. It is quite common for family members and guests to consume high caloric foods. High caloric fried snacks and desserts are commonly offered to guests. Refer to the Summary section on how to eat healthy.
Suraj Mathema, MS, RD, CDN, MBA is a Registered and Certified Dietitian who has worked as Dietitian with geriatric and developmentally disabled population for more than sixteen years. He is currently working in New York City as a Consultant Dietitian for Nutrition Consulting Services. Contact information smathema1@yahoo.com
References
- The Nepal Cook Book, Association of Nepalis in The Americas 1996
- Cooking in Nepal, Ratna Pustak Bhandar (1982)
- Creative Nepali Cooking with Tulsi Regmi, Tulsi Regmi.
Chapter 11
Low Fat Cooking & How to Modify a Recipe
Nimesh Bhargava, MS, RD, CNSD, MBA
Diet related diseases like heart disease, obesity, cancer and diabetes greatly affect the quality of life. The need to manage these diseases with proper diet and a growing health-consciousness has brought awareness in people to explore new ways of cooking and eating. There are many sources to draw from including low-fat cookbooks and the latest sources are the numerous websites that offer low-fat recipes.
It is important to remember that while fats, ‘ghee’ or oils bring richness and taste to the food, they also contain twice the amount of calories as compared to carbohydrate or protein. Besides being a concentrated source of calories they are readily converted and stored as body fat. The type of fats and oils as well as amounts used will determine if a recipe is heart-healthy or not. Most of your favorite recipes can be easily changed to lower the fat, salt, and sugar content and increase fiber. This section of the book is devoted to tips on making your favorite recipes healthier.
Making your favorite recipes healthier
With a little practice, you can turn any favorite recipe into a healthy dish.
Always ask yourself – “Can I reduce the amount of salt and ghee / oil?”
Always use a measuring cup or a measuring spoon. Never pour from a container or guess the amount of salt and oil. You may know the amount of oil or salt to be added in the recipe. With time the serving size increases if you do not measure the ingredients.
- Fats like ghee, butter, oil or even margarine can be cut by half to two thirds the amount in the recipes. Try cutting the amount by small amounts first then gradually increasing to half to two thirds the amount. To replace the loss of taste when ghee or oil is reduced, consider adding alternatives such as vegetable broth, vegetables, fruit juices, herbs, spices, skim milk or skim milk powder.
- Change the cooking recipe: Instead of frying, bake, boil, broil or steam the food item. This will significantly reduce the amount of fat you consume.
- Use nonstick cooking pots and pans. Coating baking pans with vegetable cooking spray rather than using ghee or oil.
- Sauté foods in water, wine, or fruit juice rather than oil or ghee.
- Removing or cutting down oils from curry, dal, sambar or rasam. If the recipe was cooked with too much oil, cool it after cooking. Then skim the excess fat with a tea spoon to remove e the oil from the surface.
Use a plastic degreaser constructed like a pitcher with a spout that allows the liquid to be poured from the bottom instead of the top.
- Trimming fat from poultry, beef or pork: Remove the skin of the chicken or turkey. Trim visible fat from beef or pork before cooking.
- Reduce the amount of salt by adding spices and herbs. Below is the list of spices that goes well with Meat, Vegetables and Fruits:
- Increase fiber by cooking brown rice instead of white rice, use whole wheat bread instead of white bread, do not sieve the flour before making the flat bread or “rotti” and leave skins on fruits or vegetables.
LowFat Cooking & How to Modify a Recipe
Vegetables: Add lemon, ginger, vinegar, dry mango powder, anardana, black pepper, corriander dry or green leaves, sesame seeds, fennel seeds, basil, oregano, onion, garlic, turmeric, tamarind and tarragon
Fruits: Cinnamon, cloves, cardamom, vanilla, or mint
Fish, Poultry, Meat: Bay leaf, chives, dry mustard, lemon, garlic, onion sage, or basil
The following table shows how you can substitute ingredients to make your recipe healthier:
|
Food Item |
Substitute with |
|
Cream |
Evaporated Skim Milk |
|
Whole Milk |
Skim Milk or 1% Milk |
|
1 cup ghee |
¾ cup vegetable oil |
|
½ cup ghee |
1/ cup vegetable oil 3 |
|
Regular cheese |
Low fat cheese or skim milk cheese |
|
Cream cheese |
Light cream cheese |
|
Butter |
Margarine |
|
Mayonnaise |
Light mayonnaise or reduce calorie mayonnaise |
|
Salad dressing |
Reduced calorie, light or fat free salad dressing |
|
Regular Gelatin |
Sugar-free gelatin mix or fruit juice mixed with unflavored gelatin |
|
1 Whole egg |
¼ cup egg substitute 2 egg whites or 1 egg white 1 teaspoon vegetable oil |
|
1 Ounce baking chocolate |
3 tablespoons cocoa powder and 1 tablespoon vegetable oil |
|
1 can condensed cream soup |
Homemade white sauce (1 cup skim milk +2 tablespoons flour +2 tablespoons margarine) |
|
Cream of celery soup |
1 cup of white sauce+¼ cup celery |
|
Cream of mushroom soup |
1 cup white sauce+1 cup mushroom |
|
Cream of chicken soup |
11/ cups of white sauce +I 2 chicken bouillon cube |
|
Fat in baked recipes |
Use no more than 1-2 tablespoons of oil per cup of flour: increase liquid slightly to add extra moisture |
|
Syrup packed canned fruit |
Juice packed canned fruit |
|
2 tablespoons flour (as thickener) |
1 tablespoon cornstarch or arrow shoot |
|
Sugar in baked recipes |
Reduce the amount by ½ the original amount: use no more than ½ cup added sweetener (sugar, honey, molasses, etc) per cup of flour. Add vanilla extract, cinnamom, and nutmeg to increase sweetness. Use half the amount of sugar and replace the other half with apple sauce or well ripen mashed bananas |
|
Baking Powder |
Low sodium baking powder |
|
Salt in recipes |
Reduce amount or eliminate by using spices and herbs |
|
Garlic, onion and celery salt |
Use garlic, onion and celery powder |
Guide to Ingredients
Anise seed : Ajwain or Carum
Asfoetida : Hing
Aborigine : Begun or baingan (eggplant)
Chapatti flour : Atta
Bay leaf : Tej patta
Bitter gourd : Karela
Black pepper : Kali mirch
Cardamom : Elaichi
Red chilies : Lal Mirch
Cinnamon : Dalchini
Cloves : Lavang
Coconut : Nariyal
Coriander seeds : Dhaniya
Cumin : Jeera
Curry leaves : Kari patta
Fennel : Saunf
Fenugreek : Methi
Garlic : Lahsun
Ginger : Adrak
Gram flour : Besan or chickpea flour
Jaggery : Gur
Mace : Javitri
Mango powder : Amchoor
Mint : Hara pudeena
Mustard : Sarson or Rai
Nutmeg : Jaiphal
Onion Seeds : Kalonji
Oregano seeds : Ajwain
Parsley : Ajmood ka patta
Paneer : Indian cheese
Pomegranate seeds : Anardana
Poppy seeds : Khus khus or posta dana
Raisin : Kismish
Red lentils : Masoor dal
Saffron : Kesar
Sesame seeds : Til
Tamarind : Imli
Toor Dhal : Yellow split lentils
Turmeric : Haldi
Vinegar : Sirka
Yellow split peas : Channa dal
Yogurt : Dahi
Sambar (Serves 4) (Original recipe)
- ½ c red lentils
- 1 tablespoon vegetable oil
- 1 tsp mustard seeds
- ½ tsp asafetida
- ½ tsp fenugreek seeds
- ½ tsp cumin seeds
- 1 dried red chili halved
- 2-3 curry leaves
- 2 green chili
- 1 cup mixed vegetables cut small pieces (onion, potato, radish, eggplant, zucchini, green bell pepper)
- 2 tbsp tamarind juice
- 1 cup water
- 1 tbsp sambar powder
- 1 tbsp chopped fresh coriander
Cook the lentils in boiling water for about 1 hour until tender then drain and set aside. Heat the oil and fry the mustard seeds, asafetida, fenugreek, and cumin seeds, red and green chili and curry leaves until the mustard seeds start crackling. Add the green chilies and vegetables and fry for 2 minutes. Add the tamarind juice, water, sambar powder, turmeric and salt, cover and simmer over a low heat until the vegetables are tender. Stir in the cooked lentils and simmer for 5 minutes. If the sambar needs to be thickened, blend the rice flour with the water, stir it into the pan and simmer for a few minutes. Garnish with coriander and serve hot with rice.
LowFat Cooking & How to Modify a Recipe
Sambar (Modified recipe)
- ½ c red lentils
- 1tsp mustard seeds
- ½ tsp asafetida
- ½ tsp fenugreek seeds
- ½ tsp cumin seeds
- 1 dried red chili halved
- 2-3 curry leaves
- 2 green chili
- 1 cup mixed vegetables cut small pieces (onion, potato, radish, Aborigine, zucchini, green bell pepper)
- 2tbsp tamarind juice
- 1 ½ cup water
- 1tbsp sambar powder
- 1 tbsp chopped fresh coriander
Cook the lentils in boilin Cook the lentils in boiling water for about 1hour until tender then drain and set aside. Roast mustard seeds, asafetida, fenugreek, and cumin seeds, red and green chili and curry leaves until the mustard seeds become brown in the heavy frying pan. Add the green chili and vegetables and add ½ cup of water and cook for 5 minutes. Add the tamarind juice, water, sambar powder, turmeric and salt, cover and simmer over a low heat until the vegetables are tender. Stir in the cooked lentils and simmer for 5 minutes. If sambar needs to be thickened, blend the rice flour with the water, stir it into the pan and simmer for a further few minutes. Garnish with coriander and serve hot with rice.
Soups Serving 4
Tomato soup with bread croutons (Original recipe)
- 500 gyms ripe tomatoes
- 1 small onion
- 4 cups of water
- Oil for deep frying
- 2 slices bread
- Salt & pepper
Cut tomatoes and onion into small pieces and add water in a pan. Boil and cook for about 20 – 25 minutes. Puree the ingredients in a blender and then pass it through a sieve. Cut the bread slice in ½ inch squares. Heat the oil and fry the bread squares until golden brown. Serve the soup in a bowl, sprinkled it with croutons, salt and pepper to taste.
Tomato soup (modified recipe)
- 500 gyms ripe tomatoes
- 1 small onion
- 4 cups of water
- 1 tablespoon olive oil
- 2 slices bread
- Pepper
- Oregano & basil leaves
Cut tomatoes and onion into small pieces and add water in a pan. Boil and cook for about 20 – 25 minutes. Puree the ingredients in a blender and then pass it through a sieve. Brush olive oil on the bread slice. Cut the bread slice in ½ inch squares. Sprinkle oregano and basil leaves on the bread. Place bread squares in 350°F oven for 10-12 minutes until golden brown. Serve the soup in a bowl, sprinkled it with croutons, and pepper to taste.
Vegetables and Vegetarians Dishes
Palak Khadi Serving 4 (original recipe)
- 2 cups plain yogurt
- ¼ cup gram flour
- ½ tsp ground red chili
- ½ tsp ground turmeric
- Salt
- 2 cups water
- ½ cup fresh palak boiled
Indian Foods: AAPI's Guide to Nutrition, Health and Diabetes
- 2 table spoon ghee
- ½ tsp mustard seeds
- 2 red chilies
- 1/8 tsp asafetida
Heat ghee in a heavy based pan and fry mustard seeds until they start crackling. Add asafetida, red chilies, boiled palace, and then water. Mix yogurt and gram flour in a bowl. Pour it in the pan. Add salt, chili and turmeric. Bring to boil, stir occasionally. Reduce the heat to medium – low then simmer for 25 minutes. Serve khadi hot with plain rice or chappatis.
Palak Khadi Serving 4 (modified recipe)
- 2 cups fat free plain yogurt
- ¼ cup gram flour
- ½ tsp ground red chili
- ½ tsp ground turmeric
- Salt
- 2 cups water
- ½ cup fresh palak boiled
- 2 table spoon canola oil or vegetable oil
- ½ tsp mustard seeds
- 2 red chilies
- 1/8 tsp asafetida
Heat oil Heat oil in a heavy based pan and fry mustard seeds until they start crackling. Add asafetida, red chilies, boiled palak, and then water. Mix yogurt and gram flour in a bowl. Pour it in the pan. Add salt, chili and turmeric. Bring to boil, stir occasionally. Reduce the heat to medium – low then simmer for 25 minutes. Serve kadhi hot with plain rice or chappatis.
Dal
Dal Makhani Serving 6 (original recipe)
- 250 gm Urad dal (black gram)
- 100 gm red kidney beans
- 1 small onion grated
- 2 ripe tomatoes chopped
- 4 tablespoons ghee
- 1 tablespoon grated fresh ginger
- Salt
- 1 tsp garam masala
- 2 green chilies chopped
- ½ cup cream
Wash dal and beans thoroughly. Soak them overnight. Boil beans and dal in a pressure cooker with salt for 30 minutes or until tender. Mash some of the cooked dal with a spoon. In another saucepan, heat the ghee and fry ginger, chilies and onions for 10 minutes or until the onion is lightly browned. Then add tomatoes and cream. Cook for 10 minutes. Reserve 1 tablespoon of this mixture and stir the remainder into dal and beans. Add garam masala and salt. Garnish with the reserved onions and tomato mixture. Serve hot with rice or chappatis.
Dal Makhani Serving 6 (modified recipe)
- 250 gm Urad dal (black gram)
- 100 gm red kidney beans
- 1 small onion grated
- 2 ripe tomatoes chopped
- 2 tablespoons vegetable oil
- 1 tablespoon grated fresh ginger
- Salt
- 1 tsp garam masala
- 2 green chilies chopped
- ½ cup light cream
Wash dal and beans thoroughly. Soak them overnight. Boil beans and dal in a pressure cooker with salt for 30 minutes or until tender. Mash some of the cooked dal with a spoon. In another saucepan, heat the oil and sauté` ginger, chilies and onions for 10 minutes or until the onion are lightly browned. Then add tomatoes and cream. Cook for 10 minutes. Reserve 1 tablespoon of this mixture and stir the remainder into dal and beans. Add garam masala. Garnish with the reserved onions and tomato mixture. Serve hot with rice or chappatis.
Spiced Chick Peas Serving 4
(Original recipe)
- 250 gm chick peas
- 650cc / 2 ½ cups water
- ½ tsp baking soda
- 4 table spoon ghee
- inch grated ginger
- 2 green chilies chopped
- 1 tsp garam masala
- 2 table spoon green mango powder
- ½ tsp red chili powder
- 2 tsp coriander powder
- Black salt to taste
- Coriander fresh chopped
- 1 onion chopped
Soak the chick peas overnight in the water with baking soda. Boil the chick peas in pressure cooker for 30 minutes until tender in low fire. Heat ghee in another pan and fry ginger and chilies add all ingredients simmer for 2-3 minutes. Add the chick peas and stir well. Cover and simmer gently for 10 minutes. Sprinkle with coriander and onion. Serve
Spiced Chick Peas Serving 4
(Modified recipe)
- 250 gm chick peas
- 650cc / 2 ½ cups water
- ½ tsp baking soda
- 2 table spoon canola oil or vegetable oil
- inch grated ginger
- 2 green chilies chopped
- 1 tsp garam masala
- 2 table spoon green mango powder
- ½ tsp red chili powder
- 2 tsp coriander powder
- Black salt to taste
- Coriander fresh chopped
- 1 onion chopped
Soak the chick peas overnight in the water with baking soda. Boil the chick peas in pressure cooker for 30 minutes until tender in low fire. Heat oil in another pan and fry ginger and chilies add all ingredients simmer for 2-3 minutes. Add the chick peas and stir well. Cover and simmer gently for 10 minutes. Sprinkle with coriander and onion. Serve hot with rice or chappatis.
Rice Dishes Serving (4)
Vegetable Pulao (original recipe)
- 225 gm/ 1 cup basmati rice washed and soaked in cold water for 30 minutes
- ¼ cup ghee
- 1tsp cumin seeds
- 4 cloves
- 1 inch cinnamon stick
- 4 cardamom pods
- 2 bay leaves
- 1 red onion finely sliced
- 100 gm cauliflower, cut into 1 cm/ 1/2 inch slices
- 100gm peas
- 2 medium carrots,cut 2.5 cm/ 1 inch slice
- 25 gm/ 1/3 cup raisin
- 1 medium carrots,cut 1 cm/ 1/2 inch pieces
- 1 tsp garam masala ground
- 1/2 tea spoon ground red chili
- 1/2 tsp turmeric powder
- Salt to taste
- 500 cc/ 2 cups water
- Coriander leaves.
Indian Foods: AAPI's Guide to Nutrition, Health and Diabetes
Drain rice and leave it to drain in colander. Heat the ghee in a non stick pressure cooker over medium heat. Add the cumin seeds followed by cloves, cinnamon stick, cardamom and bay leaves. Let the spices sizzle for 15-20 seconds, then add the onion and fry until golden. Add the rice stir fry for 2-3 minutes; add all vegetables, garam masala, chili, turmeric powder, salt and raisin. Then pour water. Bring to boil for 1 minute then reduce the heat to low, cover and cook for 15 minutes or until tender. If there is any water left, dry off on a high heat. Garnish with washed coriander leaves. Serve with low fat plain yogurt.
Vegetable Pulao (modified recipe)
- 225 gm/ 1 cup basmati rice washed and soaked in cold water for 30 minutes
- 1 table spoon canola or sunflower oil
- 1tsp cumin seeds
- 4 cloves
- 1 inch cinnamon stick
- 4 cardamom pods
- 2 bay leaves
- 1 red onion finely sliced
- 100 gm cauliflower, cut into 1 cm/ 1/2 inch slices
- 100gm peas
- 2 medium carrots,cut 2.5 cm/ 1 inch slice
- 25 gm/ 1/3 cup raisin
- 1 medium carrots,cut 1 cm/ 1/2 inch pieces
- 1 tsp garam masala ground
- 1/2 tea spoon ground red chili
- 1/2 tsp turmeric powder
- Salt to taste
- 500 cc/ 2 cups water
- Coriander leaves.
Wash rice and leave it to drain in colander. Heat the oil in a non stick pressure cooker over medium heat. Add the cumin seeds followed by cloves, cinnamon stick, cardamom and bay leaves. Let the spices sputter for 15-20 seconds, then add the onion 2-3 minutes, add all vegetables, garam masala, chili, turmeric powder, salt and raisin. Then pour water. Bring to boil for 1 minute then reduce the heat to low, cover and cook for 15 minutes or until tender. If there is any water left, dry off on a high heat. Garnish with washed coriander leaves. Serve with low fat plain yogurt.
Bread
Chappatis or Phulkas Serving 10 (original recipe)
- 14 oz whole wheat flour plus more for dusting
- ½ tsp slat
- 1/4 cup / 4 table spoon ghee
- 225 gm/ 1 cup basmati rice washed and soaked
- 8 ½ fluid oz lukewarm water
In a large bowl mix flour, salt and oil then gradually add water and mix until dough is formed. Transfer the dough to a clean surface and knead it for 5-6 minutes. Cover the dough with a damp cotton cloth, leave to rest for 30 minutes. Divide the dough in half and cut each portion into 10 equal sized balls. Dust a cake of dough lightly with flour and roll out into a 6 inch disk. Keep remaining cakes covered with a damp cloth.
Preheat a heavy cast-iron griddle pan over medium high heat. Place a chapatti on it and cook until surface begins to dry. Turn it over and cook until the underside has brown patches. Turn it over again and press the chapatti with fish slice. The chapatti will puff up now. Cook until brown patches appear on the other side.
Wrap the chappatis in a sheet of aluminum foil lined with paper towels to keep hot until you finish cooking all the dough. Serve with any curry or vegetable dish.
Cauliflower Maratha Serving 6 (original recipe)
- 350 gm grated cauliflower
- 450 gm / 4 cups whole wheat flour
- 2 medium potatoes, boiled, peeled and mashed
- 2 chopped green chilies
- 1 cm/ ½ inch ginger roots, grated
- 1 tablespoon chopped fresh coriander
- 1 tsp garam masala
- ½ tsp red chili
- Salt to taste
- 1 tsp green mango powder (amchoor)
- 300 cc/ ½ pt. /1 ¼ cup water
- ½ cup ghee
Mix salt in cauliflower and let it stand for 10 minutes. Squeeze out the water. Mix cauliflower with potatoes, chilies, ginger, coriander, garam masala, red chili, mango powder. Mix the flour, 4 table spoon ghee, salt and water to make the dough.
Knead well, cover with a damp cotton cloth and leave to rest for 15 minutes. Divide the dough into 6 equal portions and roll out each one into a thick round. Spread a little ghee. Spoon the filling into the center of each one and fold over. Roll into balls. Dust a cake of dough lightly with flour and roll out into a 5 inch disk. Preheat a cast iron griddle over medium high heat. Place a paratha on it. Brush a little ghee and turn it again brush a little ghee and fry on both sides until lightly browned. Serve with plain low fat yogurt.
Cauliflower Paratha Serving 6(modified recipe)
- 350 gm grated cauliflower
- 450 gm / 4 cups whole wheat flour
- 2 medium potatoes, boiled, peeled and mashed
- 2 chopped green chilies
- 1 cm/ ½ inch ginger roots, grated
- 1 tablespoon chopped fresh coriander
- 1 tsp garam masala
- ½ tsp red chili
- Salt to taste
- 1 tsp green mango powder (amchoor)
- 300 cc/ ½ pt. /1 ¼ cup water
- 4 table spoon canola oil or vegetable oil
Mix salt in cauliflower for 10 minutes. Squeeze out the water. Mix cauliflower with potatoes, chilies, ginger, coriander, garam masala, red chili, mango powder. Mix the flour, 1table spoon oil, salt and water to make the dough. Knead well, cover with a damp cotton cloth and leave to rest for 15 minutes. Divide the dough into 6 equal portions and roll out each one into a thick round. Spoon the filling into the center of each one and fold over. Roll into balls. Dust a cake of dough lightly with flour and roll out into a 5 inch disk. Preheat a cast iron griddle over medium high heat. Place a paratha on it. Brush a little oil and turn it again brush a little oil and fry on both sides until lightly browned. Serve with plain low fat yogurt.
Indian Foods: AAPI's Guide to Nutrition, Health and Diabetes
Snacks
Rava Dhokla Serves 4 (Original recipe)
- 1 cup Rava
- 1 cup plain yogurt
- ½ tsp ground ginger
- 2 ground green chilies
- Salt to taste
- 1 tsp eno powder
- 1 tsp baking soda
- ½ tsp sugar
- ½ tsp ground turmeric
- 4 tablespoon ghee
- 1tsp mustard seeds
- ½ tsp citric acid or lime juice
- ½ cup water
- 2 green chilies chopped
- 12 curry patta leaves
- Fresh coriander leaves
- 2 tablespoon shredded coconut
Mix rava and yogurt, cover and keep for 30 minutes. Add ginger chili paste, salt, eno, baking soda, sugar and turmeric. Place a trivet in a large saucepan, fill with water to come just below the trivet and bring to boil. Pour the batter into a greased heat proof dish so that it is about 2 cm / ¾ inches deep. When water starts boiling, place the dish on the trivet, cover and cook for about 15 minutes until the dhokla is soft and spongy. After few seconds cut into 1 inch cubes. Heat ghee and fry mustard seeds until they start cracking. Add curry patta, pieces of chili, ½ cup water with lime juice and dokhla pieces and cook further for 1 minute. Serve in a bowl and garnish with coconut and coriander.
Rava Dhokla Serves 4 (Modified recipe)
- 1 cup Rava
- ½ tsp ground ginger
- 2 ground green chilies
- Salt to taste
- 1 tsp eno powder
- 1 tsp baking soda
- ½ tsp sugar
- ½ tsp ground turmeric
- 2 tablespoon canola oil or vegetable oil
- 1tsp mustard seeds
- ½ tsp citric acid or lime juice
- ½ cup water
- 2 green chilies chopped
- 12 curry patta leaves
- Fresh coriander leaves
- 2 tablespoon shredded coconut
Mix rava and yogurt, cover and keep for 30 minutes. Add ginger chili paste, salt, eno, baking soda, sugar and turmeric. Place a trivet in a large saucepan, fill with water to come just below the trivet and bring to boil. Pour the batter into a greased heat proof dish so that it is about 2 cm / ¾ inches deep. When water starts boiling, place the dish on the trivet, cover and cook for about 15 minutes until the dhokla is soft and spongy. After few seconds, cut into 1 inch cubes. Heat oil and fry mustard seeds until they start cracking. Add curry patta, pieces of chili, ½ cup water with lime juice and dokhla pieces and cook further for 1 minute. Serve in a bowl and garnish with coconut and coriander.
Moong Dal Dosa Serving 10 (Original recipe)
- 250 gm moon dal
- 4 green chilies chopped
- Fresh coriander chopped
- ½ medium size radish, scraped and grated
- Salt to taste
- ½ tsp red chili powder
- 1 cup plain fat free yogurt
- 1/6tsp asafetida
- ½ tsp ground ginger
- ½ cup ghee
LowFat Cooking & How to Modify a Recipe
Soak the dal in water for 6 hours. Grind coarsely then mix all the ingredients. Heat a heavy based pan and smear with ghee. Pour a ladleful of batter into the pan and spread to a 15 cm / 6 inch in circle. Pour a spoonful of ghee around the edges and cook for about 2 minutes. Until each side is golden color. Serve hot with chutney.
Moong Dal Dosa Serving 10 (Modified recipe)
- 250 gm moon dal
- 4 green chilies chopped
- Fresh coriander chopped
- ½ medium size radish, scraped and grated
- Salt to taste
- ½ tsp red chili powder
- 1/6tsp asafetida
- 4 table spoon canola oil or vegetable oil
Soak the dal in water for 6 hours. Grind coarsely then mix all the ingredients. Heat a heavy based pan and smear with ghee. Pour a ladleful of batter into the pan and spread to a 15 cm / 6 inch in circle. Pour a spoon of oil around the edges and cook for about 2 minutes. Until each side is golden color. Serve hot with chutney.
South Indian Coconut Chutney (Original recipe)
- 50 gm grated coconut
- 1 cup plain yogurt
- 2 tsp ghee
- ½ tsp black mustard seeds
- 2 dried pieces of red chilies
- 1 inch of ginger
- A bunch of coriander
- 4-5 curry leaves
- Salt to taste
Mix coconut, Yogurt, coriander, ginger and salt in a blender. Heat ghee and fry the mustard seeds until seeds start cackling. Add red chilies, curry leaves, and stir in the coconut puree. Leave to cool.
South Indian Coconut Chutney (Modified recipe)
- 50 gm grated coconut
- 1 cup plain fat free yogurt
- 2 tsp canola oil or vegetable oil
- ½ tsp black mustard seeds
- 2 dried pieces of red chilies
- 1 inch of ginger
- A bunch of coriander
- 4-5 curry leaves
- Salt to taste
Mix coconut, Yogurt, coriander, ginger and salt in a blender. Heat oil and fry the mustard seeds until seeds start cackling. Add red chilies, curry leaves, and stir in the coconut puree. Leave to cool.
Raitas
Cucumber Raita Serving 4 (original recipe)
- 1 ½ cup plain yogurt
- 1 medium size cucumber
- ½ tsp black salt
- ½ tsp sugar
- 1 tsp ground roasted cumin (dry roast the cumin seeds for few seconds until golden color then grind.)
In a mixing bowl beat the yogurt with a wire whisk until smooth. Peel the cucumber and grate it. Squeeze out the excess water, mix yogurt, cucumber, salt and sugar. Sprinkle ground roasted cumin over the raita and serve.
Cucumber Raita Serving 4 (modified recipe)
- 1 ½ cup plain fat free yogurt
- 1 medium size cucumber
- ½ tsp black salt
- ½ tsp sugar
- 1 tsp ground roasted cumin (dry roast the cumin seeds for few seconds until golden color then grind.)
In a mixing bowl beat the yogurt with a wire whisk until smooth. Peel the cucumber and grate it. Squeeze out the excess water, mix yogurt, cucumber, salt and sugar. Sprinkle ground roasted cumin over the raita and serve.
Nimesh Bhargava MS, RD, CNSD, MBA is a certified dietitian / nutritionist. He is Professor of Nutrition at Mount Saint Mary College, Newburgh, NY and Clinical Nutrition Manager at Somers Manor Nursing Home and Rehab Center, Somers, NY. Contact information nimesh777@yahoo.com
Chapter 12
Choosing Healthy Snacks
Janaki Sengupta, MSc, RD, CDN, CDE
Nutritious snacks by delaying hunger and stabilizing blood sugars are an essential part of healthful meals. A recent trend is the availability of a wide variety of pre-packaged ready to eat snack items and the proliferation of Indian snack food restaurants in most metro areas in the US raising concerns about health outcomes. Savory and sweet snack foods have always been an indispensable part of the Indian cuisine. We are only too familiar with the Samosas, Kachoris, Vadas Chevda, Sev and a myriad of saltines (namkeens) not to mention the sweet “ mithais” whipped out of the kitchen in a quick minute to be served and shared with a cup of tea or coffee with family, friends and even upon the arrival of unexpected guests.
Lack of traditional social support systems, adequate time for food preparation, the need to multi task and recently the ready availability of prepared and ready to eat snacks has left Asian Indian families with a variety of choices to choose from though not be necessarily healthful. Most vegetarian snack items are either made with cereals like rice, rice flour, semolina (sooji), refined wheat flour (maida) or whole wheat flour (atta) and legume flours like chick pea flour (besan), moong flour either in combination or alone. Some snack items may contain nuts, vegetables, spices, salt, oil, ghee and or sugar.
Based on the method of preparation snacks may be:
- Savory and salted snacks that is not deep-fried, for example: Uppuma, Pav Bhaji, and Dhokla
- Savory and salted items that are deep fat fried, for example: Samosa, Pakoras, Bhujias, and Murruku (deep-fried, crunchy spirals).
- Savory and salted items that contain a combination of deep-fried and raw ingredients, for example: Bhel puri, Dahi wada, Pani puri and Chaats.
- Sweet snacks prepared and preserved in a sugar medium, for example: Rasagolla, Pumpkin petha.
- Sweet snacks deep fat fried and preserved in sugar syrup, for example: Jilebi, Gulab Jamun.
- Non-vegetarian snacks baked, fried or grilled, for example: Chicken or mutton tikka, Egg pakoras, Fish fry, Shish kababs.
Nutritional Values
Vegetarian cereal or legume based snack foods are high in carbohydrates. The fat and calorie content is high due to many of the items being either fried or containing oils, ghee or butter. While the salt content of the savory snacks may be high the sweet snacks tend to have even higher amounts of simple sugars. When served in combination a savory item with a sweet snack, - the mini meal may have the calories, fats and carbohydrates to be safely considered a meal replacement.
Non-vegetarian snack items though considerably lower in carbohydrates and higher in protein are nevertheless calorie rich due to the saturated fats they may contain.
Indian Foods: AAPI's Guide to Nutrition, Health and Diabetes
Snack Patterns
Traditionally savory snacks are consumed between meals while sweet snacks may be consumed after dinner. A social visit by friends or family prompts the inclusion of snacks with a cup of coffee or tea and may be sweet, savory or both, for not only the guests but the hosts as well. Snacks feature prominently in holiday and special occasion menus.
A predominant number of Asian Indians men and women are in the workforce; hence on weekdays the work force environment may permit the inclusion of a pre-lunch snack at work and a pre-dinner snack either before leaving the workplace or upon arrival at home. Lack of time for food and snack preparation may influence the inclusion of ready to eat snacks in the diets of this population. Store made, ready to eat snacks while being available on time to appease hunger may offer very little room for manipulation of the actual nutrients and calories ingested. These items tend to have high salt and fat content and may be unsuitable for individuals wishing to adhere to a healthful diet. Weekend snacking provides an opportunity to consume more traditional Indian snack items both at home and /or social gatherings. It is customary to serve snacks as appetizers in restaurants and homes.
The challenge of selecting and consuming healthy snacks though daunting is achievable for those seeking a healthful lifestyle contributing to glycemic control and weight management.
Tips for choosing healthful snacks
Daily living
- Plan your snack menu ahead. Foods least processed and closer to its natural state are the best choices
- Take snacks along with you to work.
- Add ‘zing’ to bland items with free foods.
- Select whole grains when feasible.
- Select baked or steamed snacks rather than fried snacks.
- Include fresh whole fruit and vegetables rather than fruit / vegetable juice for increased fiber.
- When using ready to use snacks read the nutrition facts panel and avoid high fat and high sodium items
Dining Out
- Eat a healthy snack at home before you go out (a slice of low calorie whole wheat toast with coriander chutney* or fresh whole fruit).
- Pick appetizers that are not fried – pick a light soup or fresh lemonade or tomato juice.
- Eat slowly relishing every bite.
- In social situations learn to say – no thanks to second servings.
- If eating in a restaurant – divide your entrée into 2 parts consume one part and take the other home for the next meal.
- Avoid ‘All you can eat buffets.’
* Available at most Indian grocers.
Some Healthful Snack Ideas
- Make your own chevda mix by mixing together 1cup whole wheat Chex, 1cup Puffed rice, 1 cup baked vegetable chips and ½cup of dry roasted unsalted peanuts – add your favorite spice powder - shake in a bag and divide into 1/ cup portions and take it along for a snack at work.
- Don’t like those dry crackers – don’t ever want to eat that Melba toast again? Try putting low calorie toppings like a teaspoon of tomato salsa, coriander or mint chutney for a tasty healthy snack. You could even make your own version of chutney/salsa sandwiches with lettuce /tomato and cucumber on whole wheat or multigrain bread for an office snack. If you are being treated for high blood pressure use toppings like salsa, coriander chutney pickles sparingly.
- Before you stock your pantry with snacks – plan on items you will buy – choose Whole grain cereals, crackers and breads. Mint and coriander chutneys along with tomato salsa may be store bought. Include fresh carrots, cucumbers tomatoes and your favorite vegetables to be eaten raw in your snack list. Include unsalted nuts, seeds and whole fruits. Do not shop on an empty stomach.
- If you plan on making snacks avoid deep fat frying or adding excessive amounts of oil, butter or ghee. Use low fat replacements when feasible.
- When making sweet snacks consider replacing part of the sugar with sugar substitutes like Equal or Splenda.
- Use salt and baking soda with caution in all your cookery.
- Read all product labels to learn the ingredients they contain.
- For a personalized snack/ food plan contact a Registered Dietitian “RD”.
- A snack is not a meal! – keep snack portions small.
How Nutritious is your Favorite Snack?
The table below will help you think about possible healthy snack items in different food groups. Remember portions will still have to be controlled and so should the use of oils, fats, sugar and salt.
|
Healthy Snack (Enjoy all the time) |
Not so healthy (Enjoy all the time – but within your day’s food plan) |
|
Plain Puffed rice (mamra, moori, pori.) Puffed cereals Whole wheat phulka or chappati |
Bhel puri Fried maida or whole-wheat puri |
|
Roasted corn on the cob Boiled potato chaat or tikkia Baked vegetable chips Popcorn |
Corn pakora Potato vada or fritters, samosa Potato chips |
|
Green gram or chickpea sundal or ghugni or channa masala. Fresh sprouted moong beans. Dhokla |
Gram flour batter fried bajjia, vegetable fritters. Dal vada |
|
Fruit Chaat Fresh whole fruit |
Sweet fruit preserves chutneys. Fruit pies and cake. Chocolate covered fruit. |
|
Grilled tandoori fish, chicken or lamb, kababs or tikka |
Fish fry, Chicken nuggets, Meatballs, cutlets and meat croquettes. |
|
Plain lassi |
Sweet lassi or mango lassi |
|
Roasted unsalted nuts, peanuts |
Salted nuts peanuts mixed with fried chevda |
Indian Foods: AAPI's Guide to Nutrition, Health and Diabetes
Practical Snack Modifications
|
Snacks |
Healthful Modification |
Comments |
|
Sev/ mixed chevda |
Mix 1 part chevda mix with 3 parts puffed rice or |
Reduce fats, carbohydrates |
|
bhel and nut mixes |
puffed wheat. |
and calories |
|
|
Add chopped up tomatoes, onion, coriander |
|
|
|
leaves, cucumber and a dash of lemon juice to puffed wheat /rice instead of chevda or fried mixes. |
Adding vegetables adds fiber and taste. |
|
Samosa /Kachori/eggrolls |
Prepare filling and use as stuffing in whole-wheat chappati, roll serve cut as cocktail wraps. Cherry tomatoes. Steamed cabbage leaves. Bell pepper halves Alternately form the filling into small patties lightly flour and roast on griddle |
By not using the pastry shell and not frying you will cut on the calories and fat. |
|
Sooji Uppuma |
Prepare uppuma with cracked whole wheat |
Adds fiber. |
|
Fish fry and meat patties |
Grill / bake or broil. Do not bread or batter |
By not frying, the fat and calories are lower. By not breading or batter dipping you reduce the starch and calories. |
|
Pappad |
Roast in microwave or grill over open flame. Do not fry. Select less often if on a low salt diet. |
By not frying you cut calories. |
|
Sweet desserts |
Replace with whole fresh fruit and vegetables |
Cuts carbohydrates and |
|
Fruit juice /drinks, |
|
calories. Adds fiber. |
|
dried fruits, |
|
|
|
chocolate coated |
|
|
|
raisins or |
|
|
|
strawberries. |
|
|
|
Portion sizes |
Small and petite |
Reduce calories, fats/ carbs |
|
Chips / Dips |
Replace with fresh vegetables like cucumber, bell peppers, carrots, tomatoes, and broccoli. Alternately use baked vegetable chips. Serve with coriander chutney, mint chutney or tomato salsa |
Reduce calories, fats and carbohydrates. By including vegetables you reduce calorie intake and increase fiber. |
Choosing Healthy Snacks
Exchanges
1 STARCH:
Sweet tamarind chutney 2tbsp 30gms. (Nirav)
Free Foods
Salsa 2tbsp contains 450mg sodium (Taco bell).
Janaki N.Sengupta, MSc, RD, CDN, CDE is a Registered Dietitian and Certified Diabetes Educator. She is the Nutrition Manager for theDiabetes Disease Management Team (an expert group that provides diabetes self-management education to Guildnet members), a managed care network in New York City. Contact information 516-414-0143 or at janakisengupta@gmail.com
References
1 :India & Pakistani Food Practices, Customs and Holidays. American Dietetic Association, American Diabetes Association Inc.
2 :Premila Lal. Indian Recipes, Rupa & Co. Bombay.
Chapter 13
Desserts of India
Sharmila Chatterjee, MSc, MS, RD, CDE
Desserts are often used to convey gratitude, affection, respect, joy and reward. India with its rich heritage and diversified culture also varies a great deal in sweet preparations. Sweets are either prepared at home or eaten out not limited to any one occasion. Most common are parties, lunch/dinner invitations, birthdays, festivals, anniversaries and, in general, eating out. There are numerous homemade and traditional sweets or desserts prepared which vary from region to region and place to place. They are usually passed on from generations to generations. The most common preparations that are region specific but not limited to are as follows:
North India/Nepal
Kheer, Gulaab Jammun, Kulfi, Halwa (Suji or Gaajar or dhudhi), Mahi
South India
Payasam, Sweet Pongal, Laddu
East India
Rosogolla, Misti doi, Pithe, Sandesh, Rasmalai
West India
Besan Laddoos, Shrikhand
Irrespective of the region one belongs to, the main ingredients that are used in these preparations are grains, sugar, milk and fats or oils. These ingredients are a source of carbohydrate and calories and must be eaten cautiously.
The first ingredient is usually sugar, a fast absorbing carbohydrate that is absorbed in the blood stream very quickly and raises blood sugar. It is a concentrated source of calories (1 tsp or 5 gms = 20 calories) and therefore is referred to as a Calorie Sweetener as compared to a non-caloric sweetener such as ‘Sweet and Low’ or ‘Equal’ or ‘Splenda’ ®. Portion control is one big key to successfully manage diabetes.
The second ingredient most commonly used in the preparation of sweets and desserts is milk. Most homemade desserts use either milk or milk products in the form of plain and sweetened yogurt, condensed milk fudge (khoa), fresh chenna and paneer cheeses, ghee and clotted cream. However, most of these products when prepared from whole, evaporated, condensed milk or half n half or full cream can raise blood cholesterol or contribute to heart disease. Most of the desserts or sweets are prepared by either whole milk or half-and-half for rich and creamy taste.
Modifications/Tips
- Use Non-Calorie Sweetener in the preparation of sweets and desserts. Reduce the portion sizes. If you cannot make the entire dish with non-calorie sweetener, then use only ¼ of the amount of sugar suggested in the recipe and substitute the rest with non-calorie sweetener
- Try using canola or olive oil for frying. Shallow frying is better than deep frying and using a non- stick pan usually consumes less oil. Cooking spray equally does well and is recommended for shallow frying.
- Use 1% milk to make Mahi, Kheer, Payasaam, Halwa, yogurt for Shrikhand and Mistidoi, chenna for Rosogolla and Sandesh, paneer cheeses, custard and pudding.
- Squeeze the syrup out from Rosogolla, Gulab Jamun and other sweets that are immersed in sugar syrup or make the syrup using non-calorie sweetener.
- Try to eat only half or one piece depending on the size, if the recipe is not modified. Often sweets are served as a form of prasad or prasadam in places of worship. Learning to eat smaller portions is always helpful. Count them as carbohydrate choices.
- Use low-fat or fat-free evaporated milk and unsweetened condensed milk if a recipe calls for regular condensed milk.
- Total Carbohydrate content should be equal to or less than 15gms for a serving. Therefore, while making a dessert that includes grains, sugar and milk which are all carbohydrate sources should be modified to avoid a high glycemic response.
- It is also a good practice to read labels and to look for total fat, carbohydrate sodium, and cholesterol content when buying a product if the nutrition information is available.
- Remember to count dessert as a carbohydrate source and make appropriate adjustments in the diet and insulin intake where ever applicable.
- Self monitoring of blood glucose (SMBG) is recommended to keep a track of your blood sugars. If it is high before a meal, passing the desserts may be a good idea. Generally, “Blood Sugar”and “Blood Glucose” refer to the same measure. Blood glucose is the value that indicates glucose content in the blood when tested. Fasting blood glucose levels refer to the blood test that is done in the morning before any food is eaten while Post –Prandial or Post meal is done 1-½ to 2 hrs after eating a meal.
Carbohydrate Loading
Feasting on a high carbohydrate diet may increase blood glucose to such high levels that bringing it down would be very difficult. This is called carbohydrate loading. Recent studies have focused on carbohydrate loading as being the primary factor that has a direct influence on post meal blood glucose. Therefore spacing of meals is very important and it has been found that 6 small meals are better than 3 large meals.
In general it is recommended that carbohydrates be limited to only 3-4 servings per meal. For example 1 roti w/ ½ cup dal + ½ cup yogurt is 3 carbohydrate choices. If you add 1/ cup cooked rice to your meal then it becomes 4 carbohydrate choices. Besides, it leaves no room for desserts. But if desserts were to be included then with prior planning, one carbohydrate could be omitted from the main meal. This way, the discomfort from over eating a high carbohydrate and fat-loaded meal can be avoided. Proteins are found mainly in foods such as lean meats, low-fat soy, poultry (skinless), egg, non fat cheese, paneer/chenna or lentils. Increasing fiber in the diet has been found to be helpful in the management of diabetes and heart disease. Incorporation of whole wheat breads, whole grains, raw vegetables and fruits, whole wheat flour such as rotis or tortillas, legumes etc would provide with fiber. Hence, the bottom line is to monitor carbohydrate content in a meal and avoid carbohydrate loading.
Sharmila Chatterjee, MSc, MS, RD, CDE is a Registered Dietitian (RD) and Certified Diabetes Educator (CDE). She is the Program Manager & Nutrition Consultant for the California Diabetes and Pregnancy Program called “Sweet Success” for Region 9 (San Diego and Imperial County). She also is the Out-Patient Dietitian for University of California San Diego (UCSD) Medical Center. Contact information schatterjee@ucsd.edu (W) or sharmilabchat@gmail.com (H)
References
- American Dietetic Association. ADA Evidence Analysis Library. Diabetes Mellitus Type 1 & 2. March 2008. Available at: http://www.adaevidencelibrary.com/. Accessed February 15, 2011
- Evidence Based Nutrition principles and Recommendations for the treatment and prevention of Diabetes and related complications. Diabetes Care; 25 (1), 2002.
- Jorge Salmeron, etal: Dietary Fiber, Glycemic Load, and risk of Non-insulin dependent diabetes mellitus in women. JAMA, 277 (6), 1997.
- Sharad Pendsey: Practical management of Diabetes. Jaypee brothers medical publishers. 1997.
- Madhur Jaffrey: Flavors of India. West publishings. 1995
Chapter 14
Managing your Menu in an Indian Restaurant
Karmeen Kulkarni, MS, RD, BC-ADM, CDE
Eating out at restaurants or bringing takeout food is common in the lifestyle of the average immigrant or person of East Indian origin. At least 3-4 meals are eaten away from home each week. Or there is an increase in buying convenience or packaged foods from Indian food stores or supermarkets to save preparation and cooking time. Eating out is one of the social and enjoyable recreations for many individuals.
Following are a list of tips to assist in making healthful food choices when eating out:
Lets start with appetizers
A healthful appetizer in Indian cuisine is rare, most are deep fried, for example : samosas, pakoras, puris. Papad can be either fried or baked, so of course the baked version is the preferred healthful piece. Recommendations are to share the appetizer or take a half of two different types.
Soups
Typical Indian soups are a lentil variety or a mulligatawny type soup. Both of these type of soups are healthy, low in fat and calories and high in carbohydrates. Other types of healthful soup choices, are a clear mulligatawny, a light rasam , sambar, or a yogurt base Gujarati kadi. Creamy soups with coconut, which is high in saturated fat should be an infrequent choice.
Breads
There are healthful options and of course the not so healthful ones. Papads if they are baked area great choice, the fried ones are the ones to avoid. Chappatis and naans are fine as long as they are not swimming in ghee or oil. Puris and parathas are also laden with fat and not a great choice. Size always matters , so try and select the smaller ones.
Entrees
Entrees to keep total fat , saturated fat and calories on the low end , if you are non-vegetarian, try and select fish , chicken , or shrimp. Tandoori and tikka can be low in fat, malai and korma dishes are creamy and high in fat, and can be incorporated in the not-so frequent list .Try and reduce the fried versions of the non – vegetarian items. If you are vegetarian meatless entrees are a recommended choice, however again check out the oil and or the ghee in the entrée.
Rice
Rice most restaurants serve plain pullao, a healthful version .And if one wants something more, biryani is always on the menu, there are many varieties of biryani, the chicken , shrimp and vegetable versions would be recommended over the lamb and beef , mainly for the fat content. Portion size is a key with regards to rice items, as one-third cup of cooked rice is a starch or carbohydrate serving, so attention to the amount of rice as part of the meal is always helpful.
Vegetable dishes
Menu items made with garbanzos, lentils, potatoes, green peas are starch or carbohydrate servings, and
Indian Foods: AAPI's Guide to Nutrition, Health and Diabetes
should be counted as such. Vegetables like spinach, cauliflower, carrots, onions and /or tomatoes, are all non starchy, and lower in carbohydrates and calories than the starchy ones.. These are in the form of curries and if limited oil is used then they are a definite healthy addition to the menu.
Accompaniments and condiments
Raita (if prepared with non-fat or low –fat yogurt) and all the other chutneys, like mint and tamarind, are all prepared with a variety of low calorie ingredients, and spices. The pickles and some chutney though low in calories, maybe high in sodium and if a person has hypertension, then it would be a red flag, and a reduced intake would be recommended.
Desserts
Desserts are an integral part of the meal, kulfi, various versions of kheers, are all high in calories and saturated fat, and should be eaten with caution or with portion sizes in mind. Moderation being the key.
It is easy to choose a healthy meal in an Indian restaurant, the main items to watch out for are the fats, fried foods, and overeating. Portion control should not be too difficult, as very large portions are not served. Try to not over order and not overeat, but enjoy and stay healthy.
Karmeen Kulkarni, MS, RD, BC-ADM, CDE is the Director, Scientific Affairs, Abbott Diabetes Care. She has served as the President, Health Care &Education for the American Diabetes Association. Contact information kdev.kul.22@gmail.com
Chapter 15
Carbohydrate Counting for Indian Foods
Karmeen Kulkarni, MS, RD, BC-ADM, CDE
Carbohydrate counting is a meal planning tool that helps plan and eat balanced meals and control blood glucose levels, along with the medications and physical activity. When a person uses carbohydrate counting, the focus is on the carbohydrate in the food. This is due to the fact that carbohydrate raises your blood glucose much more rapidly than the other two macronutrients that provide calories protein and fat (excluding alcohol, which is not a macronutrient).
Calculating the amount of carbohydrate in each meal or snack that a person eats each day can help in keeping the blood glucose at an optimal level, adjusting the diabetes medication or insulin as needed.
Most often carbohydrate foods are associated with starches. For example: pasta, bread, potatoes, corn all contain carbohydrates. But these are not the only foods that contain carbohydrates. Following is a more complete list of the food groups whose calories are mainly from carbohydrate:
- Starches: rice, pasta, bread, cereal, crackers
- Starchy vegetables: potatoes, com, green peas, beans and lentils
- Fmit and fruit juices
- Non Starchy vegetables: spinach, tomatoes, cauliflower
- Dairy Foods: yogurt, milk, and other dairy foods
- Sweets I Desserts: cakes, cookies, candy
- Beverages high in sugar
Foods that do not contain carbohydrate in them are:
- Meats (poultry, fish, seafood, eggs, red meat)
- Fats (butter, oil, margarine, nuts have some ccu-bs)
The carbohydrate content of these foods ccm be found in the chapter on Food Exchanges
Carbohydrate Counting and Blood Glucose Control?
Blood glucose levels are directly related to tl1e amount of carbohydrate one eats. If the amount of carbohydrate is tracked at meals and snacks, and the blood glucose levels are taken before and two hours after the meal; a trend or pattern will emerge. Keeping an eye on the carbohydrate intake daily and eating the same amount each day, will assist in maintaining the blood glucose levels within the target range.
Starting Carbohydrate Counting
The focus on basic carbohydrate counting is to eat about the same amount of carbohydrates at the same time each day to get an estimate on how much carbohydrate effects the blood glucose levels before and two hours after a meal. Counting carbohydrate can be done either way. Count the total grams of carbohydrate in a meal or snack; or a carbohydrate serving is equal to 15 grams of carbohydrate (based on the exchange food list). The size of the serving will vary based on the type of food you plan to eat, for example ½ cup of cooked aviyal or a three inch round idly or a six inch chapati or phulka or ½ cup of sambar. All of tl1ese foods contain 15 grams of carbohydrate per serving. This means that if you eat more then one more serving of the food item, then you will need to count the carbohydrate in your serving size you have eaten. The exchange lists in this book contain a listing of the 15 gram portions of commonly eaten Indian foods.
How much Carbohydrate should a person eat?
Each person has their own threshold for carbohydrate; the correct amount for them. A few of the areas to consider when trying to estimate the amount of carbohydrate amount for the clay is a person's weight and height, the usual food intake, daily work and leisure schedule, the favorite foods, amount of daily physical activity, target blood glucose goals, diabetes medications or insulin (type of insulin and the timing of insulin action)
For a female, a basic rule of thumb for estimating the carbohydrate servings is approximately 45-60 grams of carbohydrate, or three to four carbohydrate servings per meal. For males, it is four to five carbohydrate servings per meal or 60-75 grams of carbohydrate per meal. Plan to keep the carbohydrate amount the same at meals and snacks, until the person feels comfortable to move forward that variation. A Registered Dietitian that expertise in Indian foods and carbohydrate counting would be a resource to consult re individualizing tl1e carbohydrate prescription.
Tips for Successful Carbohydrate Counting
Carbohydrate counting takes a bit of practice, but it's a great way to learn about eating well with diabetes. It is one option,regarding meal planning for diabetes. Here are tips that will help to get you started. These are some ideas from which you can select what works for you:
- Educate Yourself. Attend classes on diabetes offered at clinics and hospitals related to diabetes management. Read everything your doctor, endocrinologist or Certified Diabetes educator has provided to you.
- Start small. Know the insulin to carb ratio and what one unit of insulin does to your blood glucose without eating.
- Begin at Home. It's always easier to eat at home than eat out because you know the ingredients.
- Test your blood glucose (BG)frequently: Test your BG before and after you eat, to see what impact each food has on your BG.
- Learn to read the nutrition facts labels. It is easier to close insulin when the carbohydrates are listed on the package, except for fruits, and vegetables.
- Keep it simple. Keep it simple. Stick to certain foods like salad dressing you like.
- Be competent: The trick is to be consistent with habits and the volume of food you eat.
- Find Technology diat works for you and use it: You may use the Lose it iphone app to look up food's carbohydrate counts. It will help with recipes and nutrition information for one servmg.
- Figure out what you can't eat: Most people with diabetes can eat anything in moderation, but carbohydrate counters sometimes find foods that jmt aren't worth the glucose spikes.
- Study your body : A little bit of record keeping goes a long way toward helping you figure things out about food and insulin dose.
- Plan it out. Do your Grocery shopping and meal planning the night before so you know what you are having.
- When you are at a restaurant Learn how to improvise. Don't take insulin until you see the menu.
- Do your homework: Always check the menu before you go to a restaurant. It's okay to ask for substitutions.
- Stay current: Use different lists of foods as it helps to keep current on what tl1e food industry has to say about certain cultural foods, uncommon foods and popular foods.
- Get comfortable with guesswork: If the meal is mainly pasta, estimate the quantity of noodles and the dose of insulin.
- Get up to speed on the internet: You can look up anything on the internet. You can't weigh everything when you go out to eat.
- When eating out at a restaurant, order basic foods.
- If it is an unknown restaurant,try to order lower carb items. Never take anything for granted.
- Pay attention to portion size. Learn what average portion sizes look like and avoid large meals when eating out.
- Share your meal. The climber of eating out is you get huge portions. Split the food up on the plate into portion sizes before you start eating.
- Weigh your food with a scale
- Be smart about mindless munching. when you are eating things like chips, count out one portion instead of eating your way through the bag or bowl.
- Don't expect your book, app or list to have all the answers: Try to stay away from things that you know are going to spike your blood glucose. Stay with foods you know.
- Learn the rules then ignore ones that don't work: Learn what different foods do for you.
- Know thyself: Carbohydrate counting is individual. Eat and test is the rule of thumb.
- Don't worry about being an expert: You will never feel like you have it 100 percent but you get used to it. Plan for a refresher diabetes class.
- Be aware of the following warning signs: Hypoglycemia usually sets in with some signals like shakiness, dizziness, hunger, mood changes, increased sweating, head ache, and pale skin color. Keep carbohydrates on hand or pack glucose tabs.
- Treat immediately: Treat your low blood glucose with 15 grams of carbohydrate, wait 15 minutes, then check your blood glucose again. Test and treat before driving, as needed.
Kanneen Kulkarni, MS, RD, BC-ADM, CDE; is Director, Scientific Affairs, Abbott Diabetes Care. She has served as the President, Health Care & Education, American Diabetes Association. She has pioneered the carbohydrate counting approach for people with diabetes. Contact information kdev.kul.22@gmail. com.
Tips for Carbohydrate counting was done by Chhaya Patel, MA, RD, CSR, DaVita Renal/Divisional Dietitian. She is the Area 1 Representative for Renal Practice Group of the American Dietetic Association. Contact information 925-937-0203 or chhaya88@hotmail.com.
Chapter 16
Achieving a Healthy Body Weight and
Exercise Interventions to the Prevention
Dr Wahida Kannally, DrPH, RD, CDE, CLS, FNLA
Maintaining a Healthy Weight is a Balancing Act
Calories In = Calories Out

Obesity is a growing epidemic worldwide and the second leading cause of preventable death in developing countries.
Overweight and obesity are major risk factors for a number of chronic diseases, including diabetes, heart diseases, and cancer. Coronary heart diseases is twice as common in obese people as in normal weight people, and obesity substantially exacerbates all cardiac risk factors, including diabetes. Obesity is associated with decreased longevity and quality of life.
The Health Consequences of Obesity
- Coronary heart disease
- Type 2 diabetes
- Cancers, such as endometrial, breast, and colon
- High blood pressure (hypertension)
- High total cholesterol or high levels, of triglycerides (dyslipidemia)
- Stroke
- Liver and gallbladder disease
- Sleep apnea and respiratory problems
- Osteoarthritis
- Reproductive health complications
Obesity also has physical, psychological, and social consequences for adults and children. Children and adolescents are now developing obesity-related diseases, such as type 2 diabetes, that in the past were seen only in adults. One study of 5- to 17-year olds found that 70% of obese children had at least one risk factor for cardiovascular disease and 39% had at least two risk factors.
Overweight and obesity can be defined as disease states in which excess body fat has accumulated to an extent that may have a negative impact on the health status of an individual. Obese individuals can differ not only according to the degree of excessive fat, which they store, but also in the regional distribution of the fat in the body. Excess abdominal fat is as great a risk factor for disease as is excess total body fat. Overweight is currently defined as body mass index (BMI) of 23 to 2 4.9 and obesity as a BMI of 25 according to the World Health Organization Western Pacific Region.
BMI=Weight (pounds) X 703/height (inches)2
http://www.nhlbisupport.com/bmi/bmicalc.htm
Asian Indians with a BMI value in the normal range have higher associated risks. Consult your doctor for your healthy BMI.
Waist Circumference
Besides using weight and BMI to identify health risk, a large waist circumference is another sign of increased risk for many health problems including:
- Heart Disease
- Type 2 Diabetes
- High Blood Pressure
where your fat is located makes a difference. If you are carrying fat around the middle, mainly around your waist (apple-shaped), you are more likely to develop health problems than if you carry fat mainly in your hips and thighs (pear -shaped).
A high-risk waist circumference is:
- A man with waist measurement over 35 inches
- A woman with waist measurement over 31 inches
Track your waist circumference as you work toward your weight loss goals.
To measure your waist circumference, place a tape measure around your bare abdomen just above your hip bone. Be sure that the tape is snug (but does not compress your skin) and tJ1at it is parallel to the floor. Relax, exhale, and measure your waist
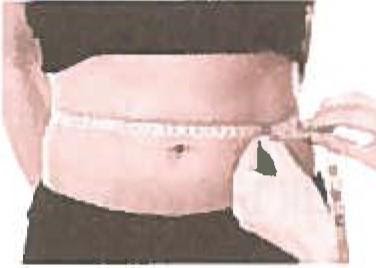
Healthy choices in nutrition and physical activity are most effective in fighting obesity.
Fad diets that promising fast results limit your nutrient needs, can be unhealthy, and tend to fail in the long run. Controlling your weight with foods dense in nutrients rather than just "empty" calories contributes to good health now and as you get older.
In the past few years, a modest weight loss, defined as a weight loss of 5% to 10% of baseline weight, has received increasing attention as a new treatment strategy for overweight and obese patients. Even a modest weight loss seems to have a positive effect on obesity- related health problems.
The key to achieving and maintaining a healthy weight is about a lifestyle that includes enjoyable and healthful foods, regular physical activity, and balancing the number of calories you consume with the number of calories your body uses. You need to enjoy your food- just eat less.
Weight Loss Guidelines
Control Calorie Intake
- self monitor regularly to help recognize and correct any fluctuations quickly
- Weigh yourself twice a week
- Track your food intake to calculate calorie intake http://www.fitday.com (free online diet journal)
- eat breakfast regularly to help spread your caloric intake throughout the day. Also curbs overeating and excessive snacking
- exercise regularly
- Spend 60 minutes daily on physical activity (walking, household chores, dancing etc). Start small
- walk 10 minutes/day to start, then increase by 3-5 minutes each week.
Expanding Portion Sizes
Control portion sizes to control dress size by:
At home
- Eat off of a smaller plate so that the portion appears to be more than it actually is
- Don't make big batches that will allow you to over-eat
- Wrap up any leftovers before the meal begins to prevent second helpings
If You are eating out
- Tell the waiter NOT to bring the bread/naan basket
- Split a regular sized meal with a friend or family member
- Eat fresh fruit in place of high fat desserts
Balancing calories is to eat foods that provide calories. You can help children learn to be aware of what they eat by developing healthy eating habits, looking for ways to make favorite dishes healthier, and reducing calorie-rich temptations.
Encourage healthy eating habits
There's no great secret to healthy eating. To help your children and family develop healthy eating habits:
- Provide plenty of vegetables, fruits,and whole grain products.
- Include low-fat or non-fat milk or dairy products.
- Choose lean meats, poultry without skin, fish, lentils, and beam including tofu
- Limit sugar sweetened beverages.
- Limit consumption of fat and saturated fat
- Be mindful of serving size
https://www.cdc.gov/healthyweight/healthy_eating/
Remember that small changes every day can lead to a lifetime of healthful returns!
Be creative in making favorite dishes healthier
The recipes that you may prepare regularly, and that your family enjoys, with just a few changes can be healthier and just as satisfying. You may makeover recipes in several ways:
Use evaporated skim milk or a few pureed almonds in place of heavy cream
Use low fat or non-fat yogurt in place of full fat yogurt
Use canola oil or olive oil in place of butter, ghee or vanaspati, in smaller amounts
Add larger amounts of vegetables such as greens, okra, tomatoes to dais, sambar
Use whole wheat flour to prepare chappatis, naan
Add vegetables to rice and pasta
Bake or saute with oil spray instead of frying foods
Remove calorie-rich temptations for daily consumption!
Although most foods can be enjoyed in moderation , save the calorie-rich temptations of high-fat and high-sugar, or salty snacks for special occasions. An attractive bowl of fruit on the kitchen counter or in your refrigerator can be very tempting for an after school or late night snack.
Raise your Fitness Level One Step at a Time
At work
- Take stretch breaks during meetings
- Have a "walking" meeting- get your colleagues to walk while you discuss business
- Take the stairs- the cheapest gym available!
- Replace your coffee break with a walking break
- Take a brisk walk before lunch for 10 minutes
At home
- Create a new morning routine. Start your day with 10 minutes of movement indoors or outdoor
- Go for a bike ride
- Trade in a power mower for a push mower
- Park the car 10 minutes from the shopping center
- Start a neighborhood walking club
- Play 'catch' or fly a kite with your children
- Dance to your favorite up-beat music for 10 minutes a day
How to lose one pound a week
- One pound of body fat 3500 Calorie
- Subtracting 500 Calories a day from your daily caloric intake will result in the loss of I pound a week.
- This can be clone with decreased food intake or replaced with a lower calorie alternative that is enjoyable
Have fresh fruit in place of a large amosa as a snack ( 100g samosa has 400 calories, 100 grams murukku have 530 Calories) and increased physical activity. Step up with 10,000steps to burn 300 Calories or spend ½ hour mopping your floors plus 1/2 hour doing housework to bum 230 Calorie.
Dr. Wahida Karmally is Associate Research Scientist, Director of Nutrition in the Irving Institute for Clinical and Translational Research and Lecturer in Dentistry at Columbia University. Contact information wk2@columbia.edu.
Chapter 17
Exchange Lists for Indians with Diabetes
Chhaya Patel, MA, RD, CSR
What are Exchange lists?
Exchange lists are foods listed together under different food groups because each serving of a food has about the same amount of carbohydrate, protein, fat, and calories as the other foods on that list. Carbohydrates are found in mainly foods rich in starches and sugars, proteins are found mainly in meats, poultry, seafood, eggs, dairy and legumes and fats and oils are found mainly in butter, hydrogenated fats, margarine and all oils. Carbohydrates, proteins and fats yield calories and a person with diabetes must make sure that there is no overload or any or all or these nutrients in a day's meal. This is why with an Exchange List, any food on the list can be exchanged or traded for any other food on the same list. Exchange lists and a meal plan can help you make healthy choices. There are three main groups - the Carbohydrate group, the Meal and Meat substitute group, and the Fat group. Foods in fat group are divided into monounsaturated, polyunsaturated, and saturated fats.
Food Group
1 Starch Exchange
(15 gms Carbohydrate, 3 gms protein, 0-1 gm fat, and 80 calories)
| Food | Portion |
|---|---|
| Aviyal | ½ cup |
| Bran cereal | ½ cup |
| Bagel | ½(1 oz) |
| Bulgur | ½ cup |
| Bread | 1 slice ( 1 oz) |
| Cereals | 1/2 cup |
| Bread sticks (4" long) | 2 (⅔ oz) |
| Cornmeal | 3 Tbsp |
| Couscous | ⅓ cup |
| English muffin | ½ |
| Hot clog or hamburger bun | ½ (1 oz) |
| Idli, plain | 3" round |
| Flour | 3 Tbsp |
| Naan | ¼ or 8"x2" |
| Granola, low fat | ¼cup |
| Grape-Nuts, | ¼ cup |
| Pita (6") | ½ |
| Grits | 1/2 cup |
| Phulka/sookhi roti/ chapati | 1 (6") |
| Food | Portion |
|---|---|
| Mumra (puffed rice) | 1 1/2 cup |
| Plain Dosa | 1 |
| Kasha | 1/2 cup |
| Plantain,green | ⅓ cup |
| Millet | ¼cup |
| Raisin bread | 1 slice ( 1 oz) |
| Muesli | ¼ cup |
| Rice, plain, cooked, wh/hr | ⅓ cup |
| Oats | ½ cup |
| Roll, plain, small | 1 (l oz) |
| Pasta | ½ cup |
| Roti (bajra, corn , juwar) | ½ (6") |
| Puffed cereal | 1 ½ cup |
| Samhar | ½ cup |
| Rice milk | ½ cup |
| Tortilla, com/flour (6-8") | 1 |
| Rice vermicelli | ½ cup |
| Waffle(4 ½ “ low fat) | 1 |
| Wheat germ | 3 Tbsp |
Starchy vegetables
Crackers and Snacks
| Baked beans | ⅓ cup |
| Animal crackers | 8 |
| Corn | ½ cup |
| Graham crackers | 3 |
| Com on cob | 1 (5 oz) |
| Matzoh | ¾ oz |
| Mixed vege (corn, peas) | 1 cup |
| Melba toast | 4 slices |
| Peas, green | ½ cup |
| Oyster crackers | 24 |
| Plantain | 4 slices |
| Popcorn (no fat) | 3 cups |
| Potato, baked or boiled | 1 small |
| Pretzels | 3/4 oz |
| Potato, mashed | 1/2 cup |
| Rice cakes | (4") 2 |
| Potato sulji ( low fat) | ½ cup |
| Whole wheat crackers | ¾ oz |
| Squash, winter | 1 cup |
| Saltine crackers | 6 |
| Yam, sweet potato, plain | ½ cup |
| Chip (fat free) | ¾ oz |
1 Starch + 1 Fat 1 Starch + 1 Very Lean Meat
(15 gms carbohydrate, 3 gms protein, 0-1 gm fat, and 80 calories.)
| Food | Portion |
| Portion | (2½”)1 |
| Beam and peas | ½ cup |
| Chow mein noodles | ½ cup |
| (Garbanzo, pinto, Corn bread (2") kidney, white, split black-eyed) | 1 (2 oz) |
| Crackers, butler type | 6 |
| Croutons | 1 cup |
| Lima beans | ⅔ cup |
| French fried potatoes | 16-25 (3 oz) |
| Lentils | 1/2 cup |
| Granola | 1/4 cup |
| Miso | 3 Tbsp |
| Mullin, small | 1 (1 ½ oz) |
| Tomato dhal | ½ cup |
| Pancake | (4") 2 |
| Food | Portion |
| Toor dhal, ckd | 1/2 cup |
| Popcorn, microwave | 1 cup |
| Rasam | 1 cup |
| Puries | 2 (5") |
| Mung dhal, ckd | 1/2 cup |
| Paratha or Thepla | 1 (6") |
| Dhansak | 1/2 cup |
| Dhokla | 1 "Square |
| Poha | 1 cup |
| Matki usal | 1/2 cup |
| Sandwich crackers (cheese) | 3 |
| Stuffing, bread | 1/2 cup |
| Taco shell | (6") 1 |
| Waffle | (4 ½'') 1 |
Fruit Exchange
15 gms carbohydrate and 60 calories.
| Apple, small, unpeeled | 1 (4 oz) |
| Peach, medium, fresh | 1 (6 oz) |
| Applesauce, unsweetened | ½ cup |
| Peaches, canned | ½ cup |
| Apples, dried | 4 rings |
| Pear, large, fresh | ½ cup |
| Apricots, fresh | 4 whole |
| Pears, canned | ½ cup |
| Apricots, dried | 8 halves |
| Pineapple, fresh | ¾ cup |
| Apricots, ccmned | ½ cup |
| Pineapple, canned | 1/2 cup |
| Banana, small | I (4 oz) |
| Plums, small | 2 |
| Blackberries | ¾ cup |
| Plums, canned | ½ cup |
| Blueberries | ¾ cup |
| Prunes, dried | 3 |
| Cantaloupe, cube: | 1 cup |
| Raisins | 2 Tbsp |
| Cherries, fresh | 12 (3 oz) |
| Rasbenies | 1 cup |
| Cherries, canned | 1 med |
| Seetaphal | 1 med |
| Strawberries, whole | 1 ¼ cup |
| Dates | 3 |
|
Tangerines, small |
2 (8oz) |
||
|
Figs, fresh |
2 medium |
||
|
Watermelon |
1 slice or 1 ¼ cup |
||
|
Figs, dried |
1 ½ |
||
|
Fruit cocktail, Fruit Juice: |
½ cup |
||
|
Grapefruit, canned |
¾ cup |
||
|
Apple juice/cider |
½ cup |
||
|
Grapes, small |
17 (3 oz) |
||
|
|
1/3 cup |
||
|
Guava, medium |
1 ½ |
||
|
Cranberry cocktail |
1 cup |
||
|
Honeydew melon, cubes |
1 cup (Reduced calories) |
||
|
Jambu |
6 |
||
|
Guava juice |
½ cup |
||
|
Kiwi, medium |
1 |
||
|
|
1/3 cup |
||
|
Loquat |
4 |
||
|
Grape juice |
½ cup |
||
|
Mandarin oranges, canned |
¾ cup |
||
|
Mixed juices, 100% |
/3 cup |
||
|
Mango, small |
½ or ½ cup |
||
|
Orange juice |
½ cup |
||
|
Nectarine, small |
1 (5 oz) |
||
|
Pineapple juice |
½ cup |
||
|
Orange, small |
1 |
||
|
Prune Juice |
1/3 cup |
||
|
Papaya, cubes |
1 cup |
||
|
Passion fruit |
½ med |
Vegetable Exchange
5 gms carbohydrate, 2 gms protein, 0 gm fat, and 25 calories per ½ cup cooked (100 gms) or 1 cup raw vegetables.
|
Artichoke hearts |
Onions |
|
Asparagus |
Parwar |
|
Bamboo shoots |
Pea pods |
|
Beans (green, wax, Italian) |
Peppers |
|
Bean sprouts (mung) |
Pink beans (valore) |
|
Beets (chukandar) |
Radish |
|
Bottle gourd (lauki) |
Ridge gourd (torai or turia) |
|
Broad beans (papdi) |
Salad greens |
|
Broccoli |
Sauerkraut |
|
Brussels sprouts |
Spinach (palak) |
|
Cabbage |
Summer squash |
|
Carrots |
Taro leaves |
|
Cauliflower (gobi) |
Taro roots |
|
Celery |
Tomatoes, fresh, canned, sauce |
|
Cluster beans (guvar) |
Turnip |
|
Cow pea pods |
Water chestnuts |
|
Cucumber |
Watercress |
|
Dill (suva bhaji) |
Zucchini |
|
Drumsticks (surgavo) |
Eggplant (brinjal) |
Vegetable Juice
|
Fenugreek leaves (methi) |
Carrot juice |
|
Green Onions or scallions |
Tomato juice |
|
Green Papaya |
Vegetable, |
|
mixed juice |
|
|
Greens (collard, kale, Mustard, Turnip) |
|
|
Karela (bittermelon) |
Kankoda (golkandra) |
|
Kohlrabi |
Leeks |
|
Lettuce |
Mixed vegetables |
|
Mushrooms |
|
Meat and Meat Substitutes
Very Lean
7 gms protein, 0-1 gm fat, 0 gm carbohydrate, and 35 calories.
|
Chicken or turkey (no skin) |
1 oz |
|
Fish |
1 oz |
|
Shellfish (crab, lobster, shrimp) |
1 oz |
|
Game |
1 oz |
|
Goat meat |
1 oz |
|
Egg white |
2 |
|
Egg substitutes |
¼ cup |
|
Cheese, fat free |
1 oz |
|
Cooked dhal or legumes |
½ cup |
|
Paneer, 1% milk |
¼ cup |
Lean Meat
7 gms protein, 3 gms fat, 0 carbohydrate, and 100 calories.
Exchange Lists for Indians with Diabetes
|
Beef, select or choice grade |
1 oz |
|
Baked/Tandoori chicken (no skin) |
1 oz |
|
Chicken (skinless) |
1 oz |
|
Pork, lean |
1 oz |
|
Lamb |
1 oz |
|
Veal, lean |
1 oz |
|
Turkey (skinless) |
1 oz |
|
Fish, fresh or canned |
1 oz |
|
Ground meat kabab |
1 oz |
|
Oysters |
6 |
|
Sardines |
2 |
|
Cottage cheese, 4.5% fat |
¼ cup |
|
Parmesan, grated |
2 Tbsp |
Medium-Fat Meat
7 gms protein, 5 gms fat, 0 carbohydrate, and 130 calories.
|
Beef, prime grades |
1 oz |
|
Pork |
1 oz |
|
Veal cutlet |
1 oz |
|
Chicken with skin |
1 oz |
|
Chicken, fish, lamb Tikka |
3x1” pieces |
|
Fish, fried |
1 oz |
|
Cheese, Feta, mozzarella, ricotta |
1 oz |
|
Egg |
1 |
|
Soy milk |
1 cup |
|
Tempeh |
¼ cup |
|
Tofu |
2 oz |
High-Fat Meat
7 gms proteitn, 8 gms fat, 0 gm carbohydrate, and 150 calories.
|
Pork, spareribs, sausage, ground |
1 oz |
|
Cheese, all regular cheeses |
1 oz |
|
Processed sandwich meats |
1 oz |
|
Hot dog |
1 |
|
Bacon |
3 slices |
|
Peanut butter |
2 Tbsp |
|
Paneer , regular |
¼ cup |
Milk Exchange
12 gms carbohydrate, and 8 gms protein. Skim and very low fat milk (0-3 gms fat) Whole milk (8 gms fat)
|
Food |
Portion |
|
Skim milk |
1 cup |
|
½% milk |
1 cup |
|
Whole milk |
1 cup |
|
1% milk |
1 cup |
|
Evaporated whole milk |
½ cup |
|
Nonfat buttermilk |
1 cup |
|
Goat’s milk |
1 cup |
|
Evaporated skim milk |
½ cup |
|
Kefir |
1 cup |
|
Nonfat dry milk |
1/3 cup |
|
Lassi, regular |
1 cup |
|
Plain nonfat yogurt |
¾ cup |
|
Fruit flavored yogurt (non-fat, sugar free) |
1 cup
|
|
Lassi, non-fat, sugar free |
1 cup |
|
Paneer, 1% milk |
1 oz |
|
Masala Tea, with 1% milk |
1 cup Low fat (5 gm fat) |
|
2% milk |
1 cup |
|
Plain low fat yogurt |
¾ cup |
|
Sweet acidophilus milk |
1 cup |
Fat Exchange
5 gms fat and 45 calories.
|
Monounsaturated Fats |
Saturated Fats* |
|
Avocado, medium |
1/8 (1 oz) |
|
Bacon, cooked |
1 slice |
|
Oil, canola, olive, peanut |
1 tsp |
|
Bacon, grease |
1 tsp |
|
Olives |
8 large |
|
Butter, stick Nuts |
2 tsp |
|
Whipped |
1 Tbsp |
|
Almonds, cashews |
6 |
|
Reduced fat |
2 Tbsp |
|
Mixed |
6 |
|
Ghee, clarified butter |
1 tsp |
|
Peanuts |
10 |
|
Coconut |
2 Tbsp |
|
Pecans |
4 halves |
|
Half and half cream |
2 Tbsp |
|
Peanut butter |
2 tsp |
|
Cream cheese, regular |
1 Tbsp |
|
Sesame seeds |
1 Tbsp |
|
Reduced fat |
2 Tbsp |
Indian Foods: AAPI's Guide to Nutrition, Health and Diabetes
|
Tahini paste |
2 tsp |
Nuts, walnuts |
4 halves |
|
|
Shortening or lard |
1 tsp |
Oils, corn, safflower, soy |
1 tsp |
|
|
Sour cream, regular |
2 Tbsp |
Salad dressing, regular |
1 Tbsp |
|
|
|
Salad dressing, low fat |
2 Tbsp |
||
|
Polyunsaturated Fats Reduced fat |
3 Tbsp |
Miracle whip, regular |
2 tsp |
|
|
Miracle whip, low fat |
1 Tbsp |
|||
|
Margarine, stick, tub |
1 tsp |
Seeds, pumkin, sunflower |
1 Tbsp |
|
|
Mayonnaise, regular |
1 tsp |
*Saturated fats can raise cholesterol blood levels. |
||
|
Mayonnaise, reduced fat |
1Tbsp |
|
||
Other Carbohydrate List: Sweets and Snacks
Many of these foods are concentrated source of carbohydrate and fat. Always check Nutrition Facts on the food label. It will be most accurate source of information.
|
Food |
Portion |
Exchange per serving |
|
Angel food cake, unfrosted |
1/12 the cake |
2 carbohydrates |
|
Banana chips |
1 oz |
1 carbohydrate, 2 fats |
|
Bhel puri |
1 oz |
1 carbohydrate, 1 fat |
|
Bhujjia |
1 oz |
1 carbohydrate, 1 fat |
|
Brownie, small |
2” square |
1 carbohydrate, 1 fat |
|
Cake, unfrosted |
2” square |
1 carbohydrate, 1 fat |
|
Cookies, fat-free |
2 small |
1 carbohydrate |
|
Sandwich cookie with cream |
2 small |
1 carbohydrate, 1 fat |
|
Cauliflower Bhajia |
2 pieces |
1 carbohydrate, 1 fat |
|
Chevda mix |
1 oz |
1 carbohydrate, 1 fat |
|
Chhunda (mango pickle) |
2 Tbsp |
1 carbohydrate |
|
Chutney, tamarind |
2 Tbsp |
1 carbohydrate |
|
Cranberry sauce, jellied |
¼ cup |
1 ½ carbohydrates |
|
Cupcake, frosted |
1 small |
2 carbohydrates, 1 fat |
|
Dahi vadai, non fat yogurt |
2 pieces |
1 carbohydrate, 1 fat |
|
Doughnut, plain cake |
1 medium |
1 ½ carbohydrate, 2 fats |
|
Doughnut, glazed |
2 oz |
2 carbohydrates, 2 fats |
|
Fruit juice bars, 100%, frozen |
1 bar (3 oz) |
1 carbohydrate |
|
Fruit snack, chewy |
1 roll |
1 carbohydrate |
|
Fruit spread, 100% |
1 Tbsp |
1 carbohydrate |
|
Gelatin, regular |
½ cup |
1 carbohydrate |
|
Ghari, no ghee topping |
1 |
1 carbohydrate, 2 fats |
|
Gingersnaps |
3 |
1 carbohydrate |
|
Granola bar |
1 bar |
1 carbohydrate, 1 fat |
|
Granola bar, fat-free |
1 bar |
2 carbohydrates |
|
Gulabjammun |
2 med |
2 carbohydrate, 2 fats, ½prot |
|
Halwa, carrot and milk |
1 piece |
1 carbohydrate, 1 fat, 1 prot |
|
Halwa, sooji and milk |
1/4 cup |
1 carbohydrate, 1 fat, ½prot |
|
Handava |
1 small piece |
1 carbohydrate, 1 fat |
|
Hummus |
1/3cup |
1 carbohydrate, 1 fat |
Exchange Lists for Indians with Diabetes
|
Ice cream |
½ cup |
1 carbohydrate, 2 fats |
|
Ice cream, light |
½ cup |
1 carbohydrate, 1 fat |
|
Ice cream, fat-free, no sugar |
½ cup |
1 carbohydrate |
|
Jam or jelly, regular |
1 Tbsp |
1 carbohydrate |
|
Kachories, vegetable |
2 |
2 carbohydrate, 2 fats |
|
Kachories, mungdhal |
2 |
2 carbohydrate, 2 fats |
|
Kadhi |
1 cup |
1 carbohydrate, 1fat, 1 prot |
|
Khandavi |
6 pieces |
1 carbohydrate, 1 fat, ½ prot |
|
Khichadi, no ghee |
½ cup |
1 carbohydrate, ½ prot |
|
Kulfi |
½ cup |
1 carbohydrate, 1 fat |
|
Kheer |
½ cup |
2 carbohydrate, 3 fat, ½ prot |
|
Laddoo, wheat |
1 small |
2 carbohydrate, 2 fats |
|
Magas |
1 ½”x 1 ½” |
1 carbohydrate, 1 fat, 1 prot |
|
Mathia |
2 thin |
1 carbohydrate, 2 fats |
|
Milk, chocolate, whole |
1 cup |
2 carbohydrates, fat |
|
Mohanthal |
1 ½” x1 ½” |
1 carbohydrate, 1 fat, 1 prot |
|
Muthia, dudhi |
+ wheat flour |
4 pieces 2 carbohydrate, 1 fat |
|
Namkeen (snack mix) |
½ cup |
1 carbohydrate, 2 fats |
|
Nankhatai |
2 small |
1 carbohydrate, 1 fat |
|
Pakoda, spinach |
3 piece |
1 carbohydrate, 1 fat |
|
Pani puri |
6 |
1 carbohydrate, 1 fat |
|
Papad |
2 |
1 carbohydrate |
|
Pav bhaji, small |
3 oz |
1 carbohydrate, 1 fat |
|
Petha, pumkin |
2” piece |
2 carbohydrates |
|
Pie, fruit, 2 crust |
1/6 pie |
3 carbohydrates, 2 fats |
|
Pie, pumpkin or custard |
1/8pie |
1 carbohydrate, 2 fats |
|
Pizza, cheese, thin crust |
¼ of 10” |
2 carbohydrates, 2 med fat |
|
|
Meats, 1 fat |
|
|
Potato chips |
12-18 (1oz) |
1 carbohydrate, 2 fats |
|
Potato Paratha |
1 (6”) |
1 carbohydrate, 2 fats |
|
Pudding, regular low fat milk |
½ cup |
2 carbohydrates |
|
Pudding, sugar-free, low fat milk |
½ cup |
1 carbohydrate |
|
Rasagolla |
2 med |
2 carbohydrate, 1 fat, 1 prot |
|
Rasmalai, in reg milk |
2 small |
2 carbohydrate, 2 fats, 2 prot |
|
Salad dressing, fat free |
¼ cup |
1 carbohydrate |
|
Samosa, vegetable |
1 |
1 ½ carbohydrate, 1 fat |
|
Sherbet, sorbet |
½ cup |
2 carbohydrates |
|
Shrikhand |
¼ cup |
1 carbohydrate, 1-2fat, 1 prot |
|
Spaghetti, pasta sauce, canned |
½ cup |
1 carbohydrate, 1 fat |
|
Sweet Roll or Danish |
1 (2 ½ oz) |
2 ½ carbohydrate, 2 fat |
|
Syrup, light |
2 Tbsp |
1 carbohydrate |
|
Syrup, regular |
1 Tbsp |
1 carbohydrate |
|
Syrup, regular |
¼ cup |
4 carbohydrates |
|
Tortilla chips |
6-12 (1 oz) |
1 carbohydrate, 2 fats |
|
Undhiyu, with 1 tsp oil |
½ cup |
1 carbohydrate, 1 fat |
|
Uppuma, with 1 tsp oil |
1/3cup |
1 carbohydrate, 1 fat |
|
Uttapam, vege |
1 small |
2 carbohydrate, 1 fat |
|
Vanilla wafers |
5 |
1 carbohydrate, 1 fat |
|
Vegetable cutlet |
1 med |
1 carbohydrate, 1/2 fat
|
|
Yogurt, frozen, low-fat, fat free |
1/3cup |
1 carbohydrate, 0-1 fat |
|
Yogurt, frozen, fat free, no sugar |
½ cup |
1 carbohydrate |
|
Yogurt, low-fat, with fruit |
1 cup |
3 carbohydrates, 0-1 fat |
Free Foods
|
Coriander chutney |
1 tsp |
100 mg sodium (Nirav) |
|
Salsa |
2 Tbsp |
450 mg sodium (Taco bell) |
|
Marinated chillies |
1 |
Follow American Dietetic Association Inc and The American Diabetes Association’s Exchange lists for Meal Planning for the following lists:
§ Free foods list
§ Drinks
§ Condiments
§ Seasonings
§ Combination foods list
§ Fast foods list
§ Sodium content of some of the foods on this exchange lists
§ Avoid canned, cured, ready to eat and processed foods for sodium/salt restricted diets.
Chhaya Patel, MA, RD, CSR, is the DaVita Renal/ Divisional Dietitian in the San Francisco Bay Area. She is a Certified Specialist in Renal Nutrition and the Area 1 Representative for Renal Practice Group of the American Dietetic Association. She was the Associate Chair and Region V representative for CRN. Contact information 925-937-0203 or chhaya88@hotmail.com.
References
1. Exchange Lists for Meal Planning. American Diabetes Association, Inc. and The American Dietetic Association. 2008.
2. Diabetes Meal Planning for Indian and Pakistani clients. The American Dietetic Association.
3. Patel, C and Denny, M. Cultural Foods and Renal Diets- A Multilingual Guide for Renal Patients, Section II, Council on Renal Nutrition of Northern California, NKF. Second Edition, 1997.
Chapter 18
Selecting Foods from Different Food Groups in the Indian Cuisine
Paclmini Balagopal, Rita Batheja, Wahida Kannally, Karmeen Kulkarni, Raqjita Misra, Sudha Raj, and Nirmala Ramasubramanian
The Dairy and Equivalents Group
(Fat-Free And Low-Fat Cheese, Milk, Yogurt And Equivalent Foods)
Use
low fat or fat-free cheese, yogurt, curds and paneer made from skim or 1 % fat milk, low-fat soy and other beverages (usually with fortified with calcium- but watch for high sugar content and varying nutrient values!)
Use Less Often
Whole milk and whole milk products, full-fat yogurts, whole milk paneer, cheeses, sweetened flavored milk, ice creams, whole milk smoothies or milk equivalents from other sources that are high in fat and/or sugar etc.
The Meats, Legumes, and Equivalents Group
(Dry Beans, Eggs, Fish, Lean Meat, Nuts, Skinless Poultry And Seeds)
Use
Egg whites, fish, legumes and dhals (remember they also have carbohydrates), lean meat, poultry (without skin), low-fat tofu,seitan,unsalted nuts and seeds.
Use Less Often
Egg yolks, creamed dhals, fried and or highly fatty and salted meats.
The Fruit Group Use
Apple, berries, grapes, mango, orange, papaya, pear, pineapple, plum, pomegranate, sapota, sita phal etc
Use Less Often
Preserves, dried fruits or fruits with added sugar, salt or fats
The Vegetable Group
Use
Brinjal (eggplant), cabbage, capsicum, carrots, cauliflower, cucumber, drumstick, gourds like karela, mushrooms, radish, spinach, tomatoes in salads or with a little oil to sautee the seasonings
Use Less Often
Pickled or vegetables fried in oil such as bhajias, fried papads etc.
The Starch and Grains Group
(Whole, Fortified and Fiber-Rich Grain Foods)
Use
Brown rice, bajra, quinoa, whole wheat pasta, ‘samai’, ‘varagu’, oats etc
Use with Controlled Fat
Idly,aviyal, biriyani, bissibele, dhansak,dhokla, dosa, dum aloo, khandvi, masala dosa, mutthiya, poha, pongal, pulao, puliodarai, etc
Use Sparingly
Bhajiya, boondi, chakkarai pongal, chakka- pradaman, fried dosa, fried vadams, golgappa, pani-puri, puris, tikki, uthappam, vada, etc.( lower case)
Concentrated Sweets, Fats, Oils – Use Sparingly
butter, ghee coconut oil, coconut milk, vanaspati, sugar, gur,desserts such as gulab jamoon, , halwa, kheer, laddu, milkshakes, peda, pudding, rasmalai, rossogolla, badushah, barfi, bassundi, seera (sooji ka halwa), sonpapadi etc.
Information was compiled by the reviewers of this book. Contact information (Padmini Balagopal, PhD, RD, CDE, IBCLC) velchet2@gmail.com
Chapter 19
Do Indian Spices & Condiments have a Role to Play in Preventive Health and Therapeutics?
Padmini Balagopal, Wahida Karmally, Karmeen Kulkarni, Ranjita Misra and Sudha Raj
Indian spices and condiments have been around for aeons and influence the nature, taste, flavor and characteristics of Indian dishes. Many of them are part of Ayurveda (the science of life and health) and it has always been a moot question as to whether they were added to enhance taste and flavor or to promote health because many of these spices and condiments have been ascribed health-promoting or therapeutic roles. In fact, it is postulated that some of them like turmeric were given religious significance (to make sure it would be used). Scientific research is exploring the possible benefits, and/or the presence of bio-active substances, present in these accompaniments. In order to define their roles, it is necessary to itemize them and examine the evidence-based research available. Given below, is a list of some of the various spices and condiments that are added in one form or other to Indian dishes.
|
No |
Ref |
Spice/ Condiment |
Botanical name |
Note worthy data |
‘Putative’ or ascribed benefits |
Common dosage in a dish for 4 people |
Evidence-based benefits/side-effects* |
|
1 |
- |
Asafoetida (used to flavor dishes) ‘Hing’ |
Ferula foetida |
Acrid, bitter taste, strong, pungent alliaceous odor due to its sulphur compounds |
Used as a digestive aid to relieve flatulence |
Approx 1 tsp |
No side-effects are known when used in food preparation. |
|
2 |
[1, 2] |
Basil (used in pesto, soups), also include ‘holy’ basil ‘tulsi’ |
Ocimum basilicum (4 diff. types) |
Seeds or leaves used. Has a clove scent |
Anti-infective uses ascribed |
A few leaves or 2 tsps of paste |
Effectiveness for claims to treat flatulence and stimulate appetite has not been documented. |
|
3 |
[3-7] |
Black Cumin ‘Kalajheera’ |
Nigella sativa- essential oil- thymoquinone; alkaloids and saponins |
Thymoquinone; nigellicine, nigellidine, saponins Nigella sativa- essential oil- thymoquinone;alk aloids and saponins |
As a digestive aid |
1 tsp |
Potential to induce apoptotic activity in human breast cancer cell lines and reactivates epigenetically silenced genes; regulate blood glucose level, inhibit cholesterol absorption and produce dyslipidemic effects. |
|
4 |
- |
Black Pepper ‘kali mirch’ ‘milagu’ |
Piper Nigrum |
Used to season |
Powdered black pepper and turmeric is used for cough and upper respi- ratory infections |
½ tsp |
No available evidence on benefits or side effects in human studies. |
|
5 |
[8, 9] |
Caraway seeds “Sajeera’ |
Carum carvi |
Carvone |
Used to season dishes |
1 and ½ tsp dried fruit and oil |
Case studies and small trials on bronchial dilatory effects. Chemotherapeutic properties; Antimutagenic activity. |
|
6 |
[10-13] |
Cardamom ‘Elaichi’ ‘Elakkai’ |
Elettaria cardamomum |
Along with other ingredients it contains phytochemical – limonene and 1, 8- cineole. |
As a digestive aid, relieve flatulence, stomach cramps |
1-2 pods |
Anti-oxidant and may have anti-spasmodic properties. No known harmful effects with amounts used in food preparation. |
|
7 |
[14, 15] |
Chillies ( active compound Capsaicin) Cayenne Pepper ‘Lal mirchi’ |
Capsicum annum |
Many varieties with varying Degrees of ‘sting’ measured in ‘scoville heat units’ - SCH |
Believed to improve taste and health |
1 tsp - 1 ½tsp |
Capsaicin is used in topical pain medications. Large doses over a period of time can cause chronic gastritis, kidney damage and liver damages. |
|
8 |
[16, 17] |
Cloves Lavang Kirambu, Lavangam Lavangalu |
Syzygium aromaticum |
Can be eaten raw or used in dishes |
Used to improve flavor; clove oil used for toothache |
1 or 2 |
No side effects are known when used in food preparation. |
|
9 |
[18-20] |
Cinnamon ‘Dalchini’ ‘Patthai’ Karuva |
Sold as cinnamon Cinnamomum verum, Cinnamomum zeylanicum indigenous to Sri Lanka and southwest India |
Inner layer of the bark |
Used to improve flavor |
¼ - ½ inch |
Limited evidence for diabetes management. May benefit halitosis when cinnamon gum is chewed. No side effects are known when used in cooking. |
|
10 |
[21, 22] |
Coriander leaves (fresh) and Coriander seeds ‘Dhania’ ‘Kothmeer’ ‘kothamalli’ |
Coriandrum or sativum L Coriander sativum |
Seeds are usually ground and leaves and stems used as such |
Used for flavor |
1 tsp or to taste |
Reported to have bactericidal properties, anti-oxidant and hepato- protective properties. |
|
11 |
[23] |
Cumin seeds ‘jheera’ |
Cuminum cyminum |
Eaten raw or added to dishes |
Used as a digestive aid |
1 tsp |
It has chelating power, lipid peroxidation inhibitor with highest chelating powers. |
|
12 |
[24-26] |
Curry leaves ‘kadi patha’ |
Murraya koenigii |
Breaking the leaves increases the flavor |
Used for flavor and fragnance |
1 tsp |
Anti-diabetic effect on streptozotocin-induced diabetic rats. |
|
13 |
[27] |
Fennel seeds/Aniseed ‘Saunf’ |
Pimpinella anisum |
Eaten raw or used in cooking |
Used as a mouth freshner and digestive aid; belived to be a galactagogue in breast feeding |
1 tsp |
Fennel seed is a potential source of natural anti-oxidants |
|
14 |
[28] |
Fenugreek seeds ‘methi’ |
Trigonella foenum graecum |
Usually mixed into dishes or sprouted etc |
Help in digestion and diarrhea; belived to be a galactagogue in breast feeding |
1 tsp |
Fenugreek seeds have demonstrated a beneficial hypoglycemic effect in diabetic subjects |
|
15 |
[29-33] |
Garlic ‘lasan’ |
Allium sativum |
Used after sautéing in oil to flavor dishes |
Used in different forms (powder, toothpaste, mouthwash, raw, crushed) Believed to have medicinal value and a galactagogue in breast feeding |
1-4 cloves |
Beneficial effects of CVD health, prevention of dental caries, and reductions in blood pressure |
|
16 |
[34-36] |
Ginger (fresh) ‘adrak’ |
Zinziber officinale |
Crushed and added to dishes |
Used to contribute to health and help with digestion |
1 inch piece |
Increased intestinal motility. |
|
17 |
[37, 38] |
Kandanthippili ‘pipali’ |
Piper longum |
Crushed and added to dishes |
Aid in digestion |
1 tsp |
Anti-amoebic activity and anti-inflammatory. |
|
18 |
[39-41] |
Nutmeg/ mace ‘jaiphal’ ‘jaipatri’ |
Mystica fragrans |
Whole nuts are preferable to ground nutmeg, as flavor deteriorates quickly |
Believed to have psychological effects in varying forms and amounts |
1-2 pinches |
Nutmeg is poisonous and should be used in very small quantities in food preparation. Nutmeg poisoning occurs in large doses and can cause death. |
|
19 |
[42, 43] |
Onion ‘Pyaz’ |
Allium cepa |
Organo sulphur compounds. The outer layers contain quercetin- a flavonoid with sulfides. |
Antioxidant properties, flavor and galactagogue (increase breast milk production) |
1 small |
Meta-analysis of 11 Randomized Control Trials indicated hypotensive effects, increased antioxidant status, and increased bioavailability of nitric oxide. Inconsistencies in human research. |
|
20 |
[44] |
Mango ‘aam’ ‘Manga’ |
Mangifera Indica |
Can be eaten raw or ripe. Used widely in chutneys, pickles, panna and other dishes |
Antioxidant. To add ‘zest’ to dishes |
1-2 fruits |
No known side effects when used in food preparation but mango allergen may cause contact dermatitis of the lips or tongue. Reduces dental caries. Antioxidant (Vitamins A, C and E), dietary fiber and minerals). |
|
22 |
[45] |
Mango ginger ‘Am haldi’ |
Curcuma amada |
Chopped and used as an accompaniment. Used to give the dish a ‘zesty’ flavor |
Used as a digestive and anti-bloating aid. |
1 Tbsp |
Anti-microbial, anti- oxidant and platelet aggregation inhibitory activity. |
|
23 |
- |
Mango powder ‘amchoor’ |
Mangifera Indica |
Used to season dishes |
Flavoring; to add zest |
1 tsp |
No available human studies. |
|
24 |
- |
Mustard seeds ‘sarson’ ‘kadugu’ |
Brassica Nigra |
Can be used whole or ground, available in white, black and brown forms. Mustard oil is used in cooking. |
Used to flavor dishes but believed to produce ‘heat’ when consumed in excess. |
1 tsp |
No known side effects when used in food preparation. May cause allergy. |
|
25 |
[46, 47] |
Neem leaves |
Azadirachta indica |
Nimbin, nimbidin, ninbidol etc. |
As a toxic killer due to its bitterness; neem sticks as a tooth brush; dry roasted need flower used in diarrhea , |
Oil, leaves, flowers and seeds |
Small clinical trials on antioxidant properties; increase in CD4+ levels in HIV patients. |
|
26 |
[48] |
Oregano Ajwan Omum ‘ajwan’ |
Oreganum vulgari
Trachysperum um ammi |
Used to season dishes and add a distinctive flavor Oleanolic acid, ursolic acid, flavonoids, tannins |
Believed to be health promoting |
1 tsp |
Antioxidant effects, beneficial in preventing atherogenesis and certain types of cancer. |
|
27 |
[49] |
Poppy seeds ‘postdana’ Kasa-kasa |
Papaner somniferum |
Used to season and flavor dishes |
May cause positive results of opiates screening |
½ tsp |
A few reported cases of allergies to poppy seeds. |
|
28 |
[50, 51] |
Saffron ‘keshar’ |
Crocus sativus |
Used in desserts as a flavoring agent |
Used to flavor milk, milk dishes and desserts. Used in pregnancy to promote fetal health and complexion! |
A few stamens |
Limited evidence as an antidepressant and relieve premenstrual syndrome |
|
29 |
[52, 53] |
Turmeric ‘haldi’ |
Curcuma domestica Curcuma longa Curcumin |
Used to season most non-sweet vegetable and legume dishes in the Asian cuisine |
Regarded as anti- inflammatory, antiseptic, and health promoting effects; purifier |
Average intake is 2-2.5g/day |
Clinical trials using large doses show no toxicity of curcumin, small clinical trials showed anti-cancer effects; low bioavailability does not permit clarity of beneficial effects. |
*Studies done may be at doses very different from common usage.
* There have been no recommended dosages established for the spices and condiments above and the responsible amount to use is not yet known. Consult your Medical Provider before use.
Ref = References
- indicates that there are no available evidence
Contact information (Padmini Balagopal PhD, RD, CDE, IBCLC) velchet2@gmail.com.
References
- Rattanachaikunsopon, P. and P. Phumkhachorn, Antimicrobial activity of basil (Ocimum basilicum) oil against Salmonella enteritidis in vitro and in food. Biosci Biotechnol 74(6): p. 1200-4.
- Opalchenova, G. and D. Obreshkova, Comparative studies on the activity of basil--an essential oil from Ocimum basilicum --against multidrug resistant clinical isolates of the genera Staphylococcus, Enterococcus and Pseudomonas by using different test methods. J Microbiol Methods, 2003. 54(1): p. 105-10.
- Salem, E.M., et al., Comparative study of Nigella Sativa and triple therapy in eradication of Helicobacter Pylori in patients with non-ulcer Saudi J Gastroenterol. 16(3): p. 207- 14.
- Akhondian, J., A. Parsa, and H. Rakhshande, The effect of Nigella sativa L. (black cumin seed) on intractable pediatric Med Sci Monit, 2007. 13(12): p. CR555-9.
- Ali, B.H. and G. Blunden, Pharmacological and toxicological properties of Nigella Phytother Res, 2003. 17(4): p. 299-305.
- Burits, and F. Bucar, Antioxidant activity of Nigella sativa essential oil. Phytother Res, 2000. 14(5): p. 323-8.
- Isik, H., et al., Potential adjuvant effects of Nigella sativa seeds to improve specific immunotherapy in allergic rhinitis patients. Med Princ 19(3): p. 206-11.
- Laribi, B., et al., Fatty acid and essential oil composition of three Tunisian caraway (Carum carvi ) seed ecotypes. J Sci Food Agric. 90(3): p. 391-6.
- Khan, R., et al., Novel compound from Trachyspermum ammi (Ajowan caraway) seeds with antibiofilm and antiadherence activities against Streptococcus mutans: a potential chemotherapeutic agent against dental caries. J Appl 109(6): p. 2151-9.
- Acharya, , et al., Chemopreventive properties of indole-3-carbinol, diindolylmethane and other constituents of cardamom against carcinogenesis. Recent Pat Food Nutr Agric. 2(2): p. 166-77.
- Verma, S.K., V. Jain, and S.S. Katewa, Blood pressure lowering, fibrinolysis enhancing and antioxidant activities of cardamom (Elettaria cardamomum). Indian J Biochem Biophys, 2009. 46(6): 503-6.
- Jamal, A., et al., Gastroprotective effect of cardamom, Elettaria cardamomum Maton. fruits in rats. J Ethnopharmacol, 2006. 103(2): p. 149-53.
- Suneetha, W.J. and T.P. Krishnakantha, Cardamom extract as inhibitor of human platelet aggregation. Phytother Res, 2005. 19(5): 437-40.
- Ritter, M., Human models of hyperalgesia and pain (chilli pepper with your acid indigestion, Sir?). Br J Clin Pharmacol. 70(2): p. 161-3.
- Ericson, A., et al., The effects of capsaicin on gastrin secretion in isolated human antral glands: before and after ingestion of red Dig Dis Sci, 2009. 54(3): p. 491-8.
- Raghavenra, H., et al., Eugenol--the active principle from cloves inhibits 5-lipoxygenase activity and leukotriene-C4 in human PMNL cells. Prostaglandins Leukot Essent Fatty Acids, 2006. 74(1): 23-7.
- Srivastava, K.C. and N. Malhotra, Acetyl eugenol, a component of oil of cloves (Syzygium aromaticum L.) inhibits aggregation and alters arachidonic acid metabolism in human blood platelets. Prostaglandins Leukot Essent Fatty Acids, 42(1): p. 73-81.
- Blevins, S.M., et al., Effect of cinnamon on glucose and lipid levels in non insulin- dependent type 2 diabetes. Diabetes Care, 2007. 30(9): 2236-7.
- Tang, M., D.E. Larson-Meyer, and M. Liebman, Effect of cinnamon and turmeric on urinary oxalate excretion, plasma lipids, and plasma glucose in healthy subjects. Am J Clin Nutr, 87(5): p. 1262-7.
- Zhu, , et al., Short-term germ-killing effect of sugar-sweetened cinnamon chewing gum on salivary anaerobes associated with halitosis. J Clin Dent. 22(1): p. 23-6.
- Kubo, I., et al., Antibacterial activity of coriander volatile compounds against Salmonella choleraesuis. J Agric Food Chem, 2004. 52(11): 3329-32.
- Chithra, V. and S. Leelamma, Hypolipidemic effect of coriander seeds (Coriandrum sativum): mechanism of action. Plant Foods Hum Nutr, 1997. 51(2): 167-72.
- Hajhashemi, V., A. Ghannadi, and H. Jafarabadi, Black cumin seed essential oil, as a potent analgesic and antiinflammatory drug. Phytother Res, 18(3): p. 195-9.
- Iyer, M. and U.V. Mani, Studies on the effect of curry leaves supplementation (Murraya Koenigi) on lipid profile, glycated proteins and amino acids in non-insulin-dependent diabetic patients. Plant Foods Hum Nutr, 1990. 40(4): p. 275-82.
- Ningappa, M.B. and L. Srinivas, Purification and characterization of approximately 35 kDa antioxidant protein from curry leaves (Murraya koenigii L.). Toxicol In Vitro, 2008. 22(3): p. 699-709.
- Math, M.V. and P. Balasubramaniam, The hypoglycaemic effect of curry leaves (Murraya Koenigii spreng). Indian J Physiol Pharmacol, 2005. 49(2): 241-2.
- Alexandrovich, I., et al., The effect of fennel (Foeniculum Vulgare) seed oil emulsion in infantile colic: a randomized, placebo- controlled study. Altern Ther Health Med, 2003. 9(4): 58-61.
- Pathak, P., S. Srivastava, and S. Grover, Development of food products based on millets, legumes and fenugreek seeds and their suitability in the diabetic diet. Int J Food Sci Nutr, 51(5): p. 409-14.
- Sobenin, I.A., et al., The effects of time- released garlic powder tablets on multifunctional cardiovascular risk in patients with coronary artery disease. Lipids Health Dis. 9: p. 119.
- Namazi, H., The role of garlic in the prevention of ischemia-reperfusion injury: a new mechanism. Mol Nutr Food Res, 2008. 52(6): 739; author reply 740.
- Fani, M.M., J. Kohanteb, and M. Dayaghi, Inhibitory activity of garlic (Allium sativum) extract on multidrug-resistant Streptococcus mutans. J Indian Soc Pedod Prev Dent, 2007. 25(4): 164-8.
- Borek, , Garlic reduces dementia and heart- disease risk. J Nutr, 2006. 136(3 Suppl): p. 810S-812S.
- Lau, B.H., Suppression of LDL oxidation by garlic compounds is a possible mechanism of cardiovascular health benefit. J Nutr, 2006. 136(3 Suppl): 765S-768S.
- Chiang, H.M., et al., Ginger significantly decreased the oral bioavailability of cyclosporine in rats. Am J Chin Med, 2006. 34(5): 845-55.
- Manju, V. and N. Nalini, Effect of ginger on bacterial enzymes in 1,2-dimethylhydrazine induced experimental colon carcinogenesis. Eur J Cancer Prev, 15(5): p. 377-83.
- Ghayur, M.N. and A.H. Gilani, Pharmacological basis for the medicinal use of ginger in gastrointestinal Dig Dis Sci, 2005. 50(10): p. 1889-97.
- Ghoshal, S., B.N. Prasad, and V. Lakshmi, Antiamoebic activity of Piper longum fruits against Entamoeba histolytica in vitro and in vivo. J Ethnopharmacol, 50(3): p. 167-70.
- Kumar, A., et al., Antiinflammatory Activity of Piper longum Fruit Oil. Indian J Pharm Sci, 2009. 71(4): 454-6.
- Beyer, J., D. Ehlers, and H.H. Maurer, Abuse of nutmeg (Myristica fragrans ): studies on the metabolism and the toxicologic detection of its ingredients elemicin, myristicin, and safrole in rat and human urine using gas chromatography/mass spectrometry. Ther Drug Monit, 2006. 28(4): p. 568-75.
- Demetriades, A.K., et al., Low cost, high risk: accidental nutmeg intoxication. Emerg Med J, 2005. 22(3): 223-5.
- Pastrana Delgado, , et al., [Nutmeg poisoning]. Med Clin (Barc), 2008. 131(16): p. 639.
- Galeone, C., et al., Onion and garlic use and human cancer. Am J Clin Nutr, 2006. 84(5): 1027-32.
- Vazquez-Prieto, M.A. and R.M. Miatello, Organosulfur compounds and cardiovascular disease. Mol Aspects 31(6): p. 540-5.
- Rocha Ribeiro, S.M., et al., Antioxidant in mango (Mangifera indica ) pulp. Plant Foods Hum Nutr, 2007. 62(1): p. 13-7.
- Policegoudra, R.S., et al., Antimicrobial, antioxidant, cytotoxicity and platelet aggregation inhibitory activity of a novel molecule isolated and characterized from mango ginger (Curcuma amada ) rhizome. J Biosci. 35(2): p. 231- 40.
- Veeraraghavan, J., et al., Neem leaf extract induces radiosensitization in human neuroblastoma xenograft through modulation of apoptotic Anticancer Res. 31(1): p. 161-70.
- Mbah, A.U., et al., Fractionated neem leaf extract is safe and increases CD4+ cell levels in HIV/AIDS patients. Am J Ther, 2007. 14(4): 369-74.
- Li, Z., et al., Antioxidant-rich spice added to hamburger meat during cooking results in reduced meat, plasma, and urine malondialdehyde concentrations. Am J Clin Nutr. 91(5): 1180-4.
- Keskin, O. and B.E. Sekerel, Poppy seed allergy: a case report and review of the literature. Allergy Asthma Proc, 27(4): p. 396-8.
- Akhondzadeh, , et al., Comparison of Crocus sativus L. and imipramine in the treatment of mild to moderate depression: a pilot double- blind randomized trial [ISRCTN45683816]. BMC Complement Altern Med, 2004. 4: p. 12.
- Agha-Hosseini, M., et al., Crocus sativus L. (saffron) in the treatment of premenstrual syndrome: a double-blind, randomised and placebo-controlled trial. BJOG, 2008. 115(4): p. 515-9.
- Zhang, F., et al., Curcumin inhibits cyclooxygenase-2 transcription in bile acid- and phorbol ester-treated human gastrointestinal epithelial Carcinogenesis, 1999. 20(3): p. 445-51.
- Sharma, R.A., et al., Pharmacodynamic and pharmacokinetic study of oral Curcuma extract in patients with colorectal Clin Cancer Res, 2001. 7(7): p. 1894-900.
Chapter 20
Summary
Padmini Balagopal, PhD, RD, CDE, IBCLC
This book has been written to help you take a proactive role with your health and help prevent and/or manage chronic disease. It is also written to empower you with information with which you can adapt the Asian-Indian cuisine into a health- promoting lifestyle that will help prevent the onset of risk factors for many diseases brought about by poor eating. Other lifestyle habits that include exercise and stress-relaxation techniques work synergistically not only to help you take charge of your health but also to optimize it.
This book is also meant to be a loud call to the men and women who have the condition of diabetes, hypertension or other lifestyle conditions to help prevent it in their children with appropriate lifestyle modifications. The introduction outlines the current health risks faced by the Asian Indian population with a description of some of the chronic diseases common to this group. The next section tells us how fetal nutrition, eating and lifestyle habits of children and adults have put us at risk for chronic diseases throughout the world epidemiologically. If we guide the eating habits of our children from a very young age, healthful eating can become second nature to them as they grow up and can help them in the future when they face healthy and unhealthy food choices!!! Many Asian Indians also face chronic heart disease and kidney disease and there are two sections that guide you through the Asian-Indian cuisine on how to eat to prevent and/or manage these conditions, both for the vegetarian and the non-vegetarian.
The Asian Indian cuisine has many interesting ways to prepare vegetables, (mainly stir-frying with different spices and condiments), legumes and lentils-also known as dhals (or dals) in a variety of gravies like sambaar or rajma, and even ways to include low-fat milk and yogurt into the everyday meal (khaddi, paneer or aviyal). When food is consumed in excess, when whole milk is used instead of 1% fat or fat-free milk to make the paneer or when just an excessive amount of foods are eaten within a day, foods can become ‘less than favorable’. It is not the single ‘soda’, the ‘chivda’ or the ‘small dessert’ that become a problem but the quantity, frequency and quality of these dishes can affect the whole day’s meal by making it high in calories, simple sugars, starches or oils and fats. The Asian- Indian meal can be a balanced meal, high in a variety of grains, vegetables and lentils and less on meat or meat alternatives. In these proportions, it can provide around 20-25 grams of valuable soluble and insoluble fiber, vitamins and minerals along with the benefits of spices and condiments (see section on Indian Spices and Condiments).
The different regional cuisines in this booklet talk about their characteristics and about how the usual diet of this region can be modified to become healthier. The Asian-Indian cuisine has been presented in six sections – the Eastern-Indian (Odia and Bengali) cuisine, the South Indian cuisine, the Maharashtrian cuisine, the Gujarati cuisine, the North Indian cuisine and the Nepali cuisine. In the chapter on Snacks, you will see the variety of snacks with cautionary alerts on how to keep snack portions small raising awareness on the possibilities of healthier substitutes for the fried snacks in the Asian-Indian cuisine. Indian desserts and sweets have had many unique characteristics from the use of ‘reduced’ milk to the use of a variety of bases from fruits and grains to even the use of vegetables. The chapter on Indian desserts sheds light on how to modify the many Indian desserts into becoming less calorie-intense.
The Asian-Indian cuisine, both in restaurants and in the home may have taken an unwise turn towards more fried, high refined foods lower in fiber and higher in salt. How to turn the Asian-Indian cuisine into becoming a high complex-carbohydrate, low-fat but high fiber cuisine is outlined in the section on ‘How to modify a recipe’. Some of the current recipes are shown with health-promoting modifications. The next section is an appropriate follow-up as you will be guided through restaurant- eating and the many pitfalls one faces with ideas on how to select wisely using the ‘healthier’ more cardio-protective alternatives. You can request that dhals be prepared without malai, that palak paneer be prepared with low-fat paneer, that the oils like olive or canola be used, instead of hydrogenated fats including ‘Vanaspati’ or ‘Dalda’, that desserts be prepared to be less ‘atherogenic’ or ‘diabetogenic’.
You will find that in each cuisine, all the foods are divided into different groups – Carbohydrates, Proteins and Fats, Dairy, Vegetables and Fruits. The section of Food Exchanges shows the amount of a food that makes up one serving and how they can be exchanged for one another within a food group. A guideline on selecting foods from each food group has also been provided.
The Asian Indian cuisine is usually high in carbohydrates and when carbohydrates become important in treatment regimens, the chapter on carbohydrate counting will help to guide the individual with specific tips to keep a count with foods in this cuisine.
Excessive weight has become a widespread issue that makes the individual vulnerable to chronic disease and general ill-health. There is a section in the book that guides you to interpret your weight, total body fat and abdominal adiposity that are crucial checkpoints. It also gives detailed guides to help you to lose excess weight with lifestyle modifications of exercise. These are vital points in self-management education that help you not only to achieve a healthy body weight but also help you to maintain it.
In recent years, there has been a lot of speculation about the role of Indian spices and condiments and a section in this book reviews the current research and literature on the role of the various spices and condiments to see if they play an active role in preventive health, therapeutics, or even palliative care.
What are some of the unhealthy trends among our children today? Drinking a lot of soda every day, eating a lot of high fat, high-refined carbohydrates and not maintaining good eating habits are factors that make the everyday diet of the younger generation weak in valuable fiber and nutrients. If we do not prevent our children from developing poor eating habits (such as indiscriminate snacking, eating ‘fast foods’ frequently and leading sedentary lifestyles from a very young age), the risk factors of becoming overweight follows easily and we may lose the weapon we have to prevent the onset of this disease as the next generation grows up. Bringing up our children on the Asian-Indian cuisine or managing our diabetes on this cuisine is not difficult once we know its strong points as well as the pitfalls that accompany it when it is not used properly. You will find that many chapters in this book caution the reader about weekend parties (common to this ethnic group) that can contribute to excessive eating.
The following sections include some concise tips to become aware of signs of hyperglycemia and hypoglycemia and tips on exercise and blood glucose management.
Tips on Blood Glucose Management
When the portions are also large, then the body is stressed to try and keep the blood glucose within optimal ranges. Conversely, when food eaten is insufficient, then a person can suffer from hypoglycemia. See below for tips on signs and symptoms of these two conditions. Here are some of the signs & symptoms of Hyperglycemia (when blood glucose levels are higher than the range at which the body functions optimally) and Hypoglycemia (when blood glucose levels drop below this range). Remember that any of these symptoms does not necessarily mean that you have the condition. The best way to know is to test your blood glucose and consult your doctor.
Some of the Signs & Symptoms of Hyperglycemia
- Increased thirst and urination
- Weakness, pain in stomach, aching all over
- Heavy labored breathing
- Loss of appetite, nausea and vomiting
- Fatigue
- Large amounts of sugar in blood
- Ketones in urine
What can you do?
- Call the Doctor immediately
- Take fluids without sugar if able to swallow
- Test blood glucose frequently
- Test urine for ketones
What are the causes?
- Not enough insulin
- Too much food
- Infection, fever, illness
- Emotional stress
Some of the Signs & Symptoms of Hypoglycemia
- Cold sweats, dizziness, feeling faint
- Headache
- Pounding of heart, trembling, nervousness
- Blurred vision
- Hunger
- Inability to awaken
- Personality changes
What can you do?
- Take Glucose tablets or orange juice (Your doctor may have specific instructions for you)
- Educate yourself about the 15-15 rule
- Check blood glucose levels
- Do not give insulin
- Do not give anything by mouth if unconscious
- Give glucagons according to package instructions
What are the causes?
- Too much insulin
- Not enough food
- Unusual amount of exercise
- Delayed meals
- Alcohol effects without food
How can you avoid Hyperglycemia or Hypoglycemia?
Consult your Doctor and work with your dietitian/ diabetes educator. Your dietitian can recommend a diet suited to your lifestyle and preferences. She/he can also show you the amounts of calories, carbohydrates, fats & proteins you are consuming presently, if you give him/her the information of the exact amounts consumed. So keeping a food record is a useful tool
Eating Tips on Blood Glucose Management
(Ask your doctor what the optimal range of blood glucose for you should be and try to keep your blood glucose within this range)
There is no diet known as a ‘diabetes diet’ and no special foods are necessary. The Introduction explains how the body regulates glucose levels in the blood from the foods we eat. Foods available in the supermarket can be used and can be eaten but with the information and awareness, you can combine health-promoting foods in a moderate amounts so that the insulin produced by your body (along with any other medication that is prescribed by your Medical Provider) will help your body use the foods you eat and keep the blood glucose (or ‘blood sugar’ as it is commonly called) within the doctor- prescribed range.
Here are some tools that can help you achieve this goal:
- Keep a record of foods and the approximate amounts till you get a good working knowledge with the help of your Medical Provider and Dietitian.
- Use heart-healthy fats and oils – monounsaturated oils like olive oil, canola oil are recommended. If you use ghee, keep it to a minimum and for occasional use but also count it in your total daily fat allowance.
- Include plenty of fresh or cooked vegetables (stir-fried with 1-2 tsps of oil to season for 3-4 cups of vegetables is recommended). Eating patterns of some regions talk about the small quantity of vegetables eaten. This is where the eating patterns can be improved. While stir- frying vegetables, use the spices, garlic, onion, coriander and other spices of your choice to improve taste instead of large amounts fats and oils. Try to avoid ‘feasting’ and ‘fasting’. If you fast, make sure that you have a good balanced meal before and after a ‘fast’.
- Make sure you include 6-8 cups of water every day. Try to avoid soda or juices as a beverage substitute for water especially for young children as this can become a habit that is tough to break!
- Eat 3-4 cups of vegetables (without much oil) and fruits with whole grain cereals, brown basmati, whole wheat flour, oats to increase fiber intake
- Avoid excess salt while garnishing foods.
- Foods like ginger, onion, garlic, cumin seeds, fenugreek seeds, fennel seeds, dhals, curry leaves, coriander leaves etc have been recommended in Ayurveda and can continue to be included
- Include a workout program that includes Yoga (after you check this out with your Medical Provider) everyday or at least 3-4 times a week.
There are references at the end of almost every chapter that can give you additional information. We have also tried to include some translations at the end. A useful reference to keep is the number to the American Dietetic Association (800-877-1600) or the e-mail address (www.eatright.org). This organization can direct you to resources and qualified professionals to help you empower yourself with helpful information on eating and on how to manage your diabetes and blood glucose levels.
More Information on Body Mass Risk Assessment and Physical Activity see chapter 16 of this book entitled “Achieving a healthy body weight and exercise interventions to the prevention and management of Type 2 diabetes” by Dr. Wahida Karmally.
Key Recommendations (From the Expert Panel on the Identification, Evaluation, and Treatment of Overweight and Obesity in Adults)
Weight loss is advised to lower elevated blood pressure in overweight and obese persons with high blood pressure. Weight loss is also suggested to lower elevated levels of total cholesterol, LDL- cholesterol, and triglycerides, and to raise low levels of HDL-cholesterol in overweight and obese persons with dyslipidemia. Weight loss is effective to lower elevated blood glucose levels in overweight and obese persons with type 2 diabetes. Use the BMI to assess overweight and obesity. Body weight alone can be used to follow weight loss, and to determine the effectiveness of therapy. The BMI to classify excess weight and obesity and to estimate relative risk of disease compared to normal weight. The waist circumference should be used to assess abdominal fat content. The initial goal of weight loss therapy should be to reduce body weight by about 10 percent from baseline. With success (and if warranted), further weight loss can be attempted. Weight loss should be about 1 to 2 pounds per week for a period of 6 months, with the subsequent strategy based on the amount of weight lost. Low calorie diets (LCD) for weight loss in overweight and obese persons. Reducing fat as part of an LCD is a practical way to reduce calories. Reducing dietary fat alone without reducing calories is not sufficient for weight loss. However, reducing dietary fat, along with reducing dietary carbohydrates, can help reduce calories. A diet that is individually planned to help create a deficit of 500 to 1,000 kcal/day should be an integral part of any program aimed at achieving a weight loss of 1 to 2 pounds per week. Physical activity should be part of a comprehensive weight loss therapy and weight control program because it: (1) modestly contributes to weight loss in overweight and obese adults, (2) may decrease abdominal fat, (3) increases cardio respiratory fitness, and (4) may help with maintenance of weight loss. Physical activity should be an integral part of weight loss therapy and weight maintenance. Initially, moderate levels of physical activity for 30 to 45 minutes, 3 to 5 days a week, should be encouraged. All adults should set a long-term goal to accumulate at least 30 minutes or more of moderate-intensity physical activity on most, and preferably all, days of the week. The combination of a reduced calorie diet and increased physical activity is recommended since it produces weight loss that may also result in decreases in abdominal fat and increases in cardio respiratory fitness. Behavior therapy is a useful adjunct when incorporated into treatment for weight loss and weight maintenance. Weight loss and weight maintenance therapy should employ the combination of LCD's, increased physical activity, and behavior therapy. After successful weight loss, the likelihood of weight loss maintenance is enhanced by a program consisting of dietary therapy, physical activity, and behavior therapy which should be continued indefinitely. Drug therapy can also be used. However, drug safety and efficacy beyond 1 year of total treatment have not been established. A weight maintenance program should be a priority after the initial 6 months of weight loss therapy.
Assessing Your Risk
According to the NHLBI guidelines, assessment of overweight involves using three key measures:
- Body Mass Index (BMI)
- Waist Circumference, and
- Risk factors for diseases and conditions associated with obesity.
The BMI is a measure of your weight relative to your height and waist circumference measures abdominal fat. Combining these with information about your additional risk factors yields your risk for developing obesity-associated diseases.
BMI is a reliable indicator of total body fat, which is related to the risk of disease and death. The score is valid for both men and women but it does have some limits. The limits are:
- It may overestimate body fat in athletes and others who have a muscular build.
- It may underestimate body fat in older persons and others who have lost muscle mass.
Use the BMI calculator shown in Chapter 16 to estimate your total body fat.
Determine your waist circumference by placing a measuring tape snugly around your waist. It is a good indicator of your abdominal fat which is another predictor of your risk for developing risk factors for heart disease and other diseases. This risk increases with a waist measurement of over 35 inches or 90 cm in men and over 31 inches or 80 cm in women.
Besides being overweight or obese, there are additional risk factors to consider are as follows: high blood pressure (hypertension), high LDL- cholesterol ("bad" cholesterol), low HDL-cholesterol ("good" cholesterol), high triglycerides, high blood glucose (sugar), and family history of premature heart disease, physical inactivity, and cigarette smoking
For people who are considered obese and have two or more risk factors, the guidelines recommend weight loss. Even a small weight loss (just 10 percent of your current weight) will help to lower your risk of developing diseases associated with obesity. Patients, who are overweight, do not have a high waist measurement, and have less than 2 risk factors may need to prevent further weight gain rather than lose weight.
Talk to your doctor to see if you are at an increased risk and if you should lose weight. Your doctor will evaluate your BMI, waist measurement, and others risk factors for heart disease. People who are overweight or obese have a greater chance of developing high blood pressure, high blood cholesterol or other lipid disorders, type 2 diabetes, heart disease, stroke, and certain cancers, and even a small weight loss (just 10 percent of your current weight) will help to lower your risk of developing those diseases.
Guide to Physical Activity
An increase in physical activity is an important part of your weight management program. Most weight loss occurs because of decreased caloric intake. Sustained physical activity is most helpful in the
prevention of weight regain. In addition, exercise has a benefit of reducing risks of cardiovascular disease and diabetes, beyond that produced by weight reduction alone. Starts exercising slowly and gradually increase the intensity. Trying too hard at first can lead to injury.
|
Examples of moderate amounts of physical activity |
|
|
Common Chores |
Sporting Activities |
|
Washing and waxing a car for 45-60 minutes |
Playing volleyball for 45- 60 minutes |
|
Washing windows or floors for 45-60 minutes |
Playing touch football for 45 minutes |
|
Gardening for 30-45 minutes |
Walking 13/4 miles in 35 minute (20min/mile) |
|
Wheeling self in wheelchair 30-40 minutes |
Basketball (shooting baskets) 30 minutes |
|
Pushing a stroller 1½ miles in 30 minutes |
Bicycling 5 miles in 30 minutes |
|
Raking leaves for 30 minutes |
Dancing fast (social) for 30 minutes |
|
Walking 2 miles in 30 minutes (15min/mile) |
Water aerobics for 30 minutes |
|
Shoveling snow for 15 minutes |
Swimming Laps for 20 minutes |
|
Stair walking for 15 minutes |
Basketball (playing game) for 15-20 minutes |
|
|
Bicycling 4 miles in 15 minutes |
|
|
Jumping rope for 15 minutes |
|
|
Running 1½ miles in 15 min. (10min/mile) |
Your exercise can be done all at one time, or intermittently over the day. Initial activities may be walking or swimming at a slow pace. You can start out by walking 30 minutes for three days a week and can build to 45 minutes of more intense walking, at least five days a week. With this regimen, you can burn 100 to 200 calories more per day. All adults should set a long-term goal to accumulate at least 30 minutes or more of moderate-intensity physical activity on most, and preferably all, days of the week. This regimen can be adapted to other forms of physical activity, but walking is particularly attractive because of its safety and accessibility. Also, try to increase "every day" activity such as taking the stairs instead of the elevator. Reducing sedentary time is a good strategy to increase activity by undertaking frequent, less strenuous activities. With time, you may be able to engage in more strenuous activities. Competitive sports, such as tennis and volleyball, can provide an enjoyable form of exercise for many, but care must be taken to avoid injury.
Activity Progression
For the beginner, activity level can begin at very light and would include an increase in standing activities, special chores like room painting, pushing a wheelchair, yard work, ironing, cooking, and playing a musical instrument.
The next level would be light activity such as slow walking of 24 min/mile, garage work, carpentry, house cleaning, childcare, golf, sailing, and recreational table tennis.
The next level would be moderate activity such as walking 15 minute/mile, weeding and hoeing a garden, carrying a load, cycling, skiing, tennis, and dancing.
High activity would include walking 10 minute/mile or walking with load uphill, tree felling, heavy manual digging, basketball, climbing, or soccer/kick ball.
You may also want to try:
- flexibility exercise to attain full range of joint motion
- strength or resistance exercise
- aerobic conditioning
http://www.nhlbi.nih.gov/health/public/heart/obesity/lose_wt/phy_act.htm
Body Mass Index, Assessing your Risk and Guide to Physical Activity: "Source: National Heart, Lung, and Blood Institute".
Some Important links: http://www.nhlbisupport.com/bmi/ www.va.gov/diabetes http://www.hhs.gov/topics/diabetes.html http://ndep.nih.gov/
http://www.diabetes.org/main/application/commercewf
http://www.diabetesnet.com/
http://www.aadenet.org/
http://www.joslin.harvard.edu/education/library/index.shtml
http://www.eatright.org/
There are six Appendices at the end of the book. Appendix 1 gives a gestational meal plan with vegetarian and non-vegetarian foods from the different food groups. The health of the fetus and mother is very sensitive to the amount of glucose in blood. Acceptable target levels will have to be established in consultation with your Medical Provider and a Registered Dietitian can help you design your eating pattern with foods that suit your preferences and still stay within established macronutrient ranges. But every prenatal woman should inform herself of the benefits of breastfeeding for her own health, the health of her baby and for the ramifications of the metabolic syndrome. Breastfeeding has been shown to help the new mother lose the excess weight gained during pregnancy besides bestowing many other benefits such as the prevention of certain types of cancers both in the mother and the baby as well as contributing to an increase the newborn’s immunity, brain growth and help with overall physiological and psychological health. For more information, contact ilca.org.
Appendix 2 is Diabetes Numbers at a Glance provided by the National Diabetes Education Program (NDEP). Appendix 3 is a Diabetes Mellitus Reference Pocket Card for use either by physicians or as a self-education tool by patients under the supervision of a Medical Provider.
Appendix 4 provides information on the require4s screening, immunization and counseling preventive services recommended for normal-risk adults and Appendix 5 is a Glossary of terms used in this book to help the reader. Appendix 6 is a 4-sided handout in English and several Indian languages that can be given to the patient as part of a patient self-education program for blood glucose and health management. There are references at the end of almost every chapter that can give you additional information. A useful reference to keep is the number to the American Dietetic Association (800-877-1600) or the e-mail address (www.eatright.org). This organization can direct you to resources and qualified professionals.
Readers of this book must be aware that the protocols used in this book regarding blood pressure, blood lipids and blood glucose levels are current as of 2011 and every individual must consult his/her Physician before implementing the information about target levels from this book.
Padmini Balagopal, PhD, RD, CDE, IBCLC is a Nutrition Consultant and a current board member of the International Board of Certified Lactation Examiners (IBLCE). She is active in the fields of diabetes prevention, management, lactation practice, and training in United States and India. Contact information velchet2@gmail.com.
Body Mass Index Table
|
Normal |
Overweight |
Obese |
Extreme Obesity |
||||||||||||||||||||||||||||
|
BMI |
19 |
20 |
21 |
22 |
23 |
24 |
25 |
26 |
27 |
28 |
29 |
30 |
31 |
32 33 34 35 36 37 |
38 |
39 |
40 |
41 |
42 |
43 |
44 |
45 |
46 |
47 |
48 |
49 |
50 |
51 |
52 |
53 |
54 |
|
Height (inches) |
|
|
|
|
|
|
|
|
|
|
|
|
|
Body Weight (pounds) |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
58 |
91 |
96 |
100 |
105 |
110 |
115 |
119 |
124 |
129 |
134 |
138 |
143 |
148 |
153 158 162 167 172 177 |
181 |
186 |
191 |
196 |
201 |
205 |
210 |
215 |
220 |
224 |
229 |
234 |
239 |
244 |
248 |
253 |
258 |
|
59 |
94 |
99 |
104 |
109 |
114 |
119 |
124 |
128 |
133 |
138 |
143 |
148 |
153 |
158 163 168 173 178 183 |
188 |
193 |
198 |
203 |
208 |
212 |
217 |
222 |
227 |
232 |
237 |
242 |
247 |
252 |
257 |
262 |
267 |
|
60 |
97 |
102 |
107 |
112 |
118 |
123 |
128 |
133 |
138 |
143 |
148 |
153 |
158 |
163 168 174 179 184 189 |
194 |
199 |
204 |
209 |
215 |
220 |
225 |
230 |
235 |
240 |
245 |
250 |
255 |
261 |
266 |
271 |
276 |
|
61 |
100 |
106 |
111 |
116 |
122 |
127 |
132 |
137 |
143 |
148 |
153 |
158 |
164 |
169 174 180 185 190 195 |
201 |
206 |
211 |
217 |
222 |
227 |
232 |
238 |
243 |
248 |
254 |
259 |
264 |
269 |
275 |
280 |
285 |
|
62 |
104 |
109 |
115 |
120 |
126 |
131 |
136 |
142 |
147 |
153 |
158 |
164 |
169 |
175 180 186 191 196 202 |
207 |
213 |
218 |
224 |
229 |
235 |
240 |
246 |
251 |
256 |
262 |
267 |
273 |
278 |
284 |
289 |
295 |
|
63 |
107 |
113 |
118 |
124 |
130 |
135 |
141 |
146 |
152 |
158 |
163 |
169 |
175 |
180 186 191 197 203 208 |
214 |
220 |
225 |
231 |
237 |
242 |
248 |
254 |
259 |
265 |
270 |
278 |
282 |
287 |
293 |
299 |
304 |
|
64 |
110 |
116 |
122 |
128 |
134 |
140 |
145 |
151 |
157 |
163 |
169 |
174 |
180 |
186 192 197 204 209 215 |
221 |
227 |
232 |
238 |
244 |
250 |
256 |
262 |
267 |
273 |
279 |
285 |
291 |
296 |
302 |
308 |
314 |
|
65 |
114 |
120 |
126 |
132 |
138 |
144 |
150 |
156 |
162 |
168 |
174 |
180 |
186 |
192 198 204 210 216 222 |
228 |
234 |
240 |
246 |
252 |
258 |
264 |
270 |
276 |
282 |
288 |
294 |
300 |
306 |
312 |
318 |
324 |
|
66 |
118 |
124 |
130 |
136 |
142 |
148 |
155 |
161 |
167 |
173 |
179 |
186 |
192 |
198 204 210 216 223 229 |
235 |
241 |
247 |
253 |
260 |
266 |
272 |
278 |
284 |
291 |
297 |
303 |
309 |
315 |
322 |
328 |
334 |
|
67 |
121 |
127 |
134 |
140 |
146 |
153 |
159 |
166 |
172 |
178 |
185 |
191 |
198 |
204 211 217 223 230 236 |
242 |
249 |
255 |
261 |
268 |
274 |
280 |
287 |
293 |
299 |
306 |
312 |
319 |
325 |
331 |
338 |
344 |
|
68 |
125 |
131 |
138 |
144 |
151 |
158 |
164 |
171 |
177 |
184 |
190 |
197 |
203 |
210 216 223 230 236 243 |
249 |
256 |
262 |
269 |
276 |
282 |
289 |
295 |
302 |
308 |
315 |
322 |
328 |
335 |
341 |
348 |
354 |
|
69 |
128 |
135 |
142 |
149 |
155 |
162 |
169 |
176 |
182 |
189 |
196 |
203 |
209 |
216 223 230 236 243 250 |
257 |
263 |
270 |
277 |
284 |
291 |
297 |
304 |
311 |
318 |
324 |
331 |
338 |
345 |
351 |
358 |
365 |
|
70 |
132 |
139 |
146 |
153 |
160 |
167 |
174 |
181 |
188 |
195 |
202 |
209 |
216 |
222 229 236 243 250 257 |
264 |
271 |
278 |
285 |
292 |
299 |
306 |
313 |
320 |
327 |
334 |
341 |
348 |
355 |
362 |
369 |
376 |
|
71 |
136 |
143 |
150 |
157 |
165 |
172 |
179 |
186 |
193 |
200 |
208 |
215 |
222 |
229 236 243 250 257 265 |
272 |
279 |
286 |
293 |
301 |
308 |
315 |
322 |
329 |
338 |
343 |
351 |
358 |
365 |
372 |
379 |
386 |
|
72 |
140 |
147 |
154 |
162 |
169 |
177 |
184 |
191 |
199 |
206 |
213 |
221 |
228 |
235 242 250 258 265 272 |
279 |
287 |
294 |
302 |
309 |
316 |
324 |
331 |
338 |
346 |
353 |
361 |
368 |
375 |
383 |
390 |
397 |
|
73 |
144 |
151 |
159 |
166 |
174 |
182 |
189 |
197 |
204 |
212 |
219 |
227 |
235 |
242 250 257 265 272 280 |
288 |
295 |
302 |
310 |
318 |
325 |
333 |
340 |
348 |
355 |
363 |
371 |
378 |
386 |
393 |
401 |
408 |
|
74 |
148 |
155 |
163 |
171 |
179 |
186 |
194 |
202 |
210 |
218 |
225 |
233 |
241 |
249 256 264 272 280 287 |
295 |
303 |
311 |
319 |
326 |
334 |
342 |
350 |
358 |
365 |
373 |
381 |
389 |
396 |
404 |
412 |
420 |
|
75 |
152 |
160 |
168 |
176 |
184 |
192 |
200 |
208 |
216 |
224 |
232 |
240 |
248 |
256 264 272 279 287 295 |
303 |
311 |
319 |
327 |
335 |
343 |
351 |
359 |
367 |
375 |
383 |
391 |
399 |
407 |
415 |
423 |
431 |
|
76 |
156 |
164 |
172 |
180 |
189 |
197 |
205 |
213 |
221 |
230 |
238 |
246 |
254 |
263 271 279 287 295 304 |
312 |
320 |
328 |
336 |
344 |
353 |
361 |
369 |
377 |
385 |
394 |
402 |
410 |
418 |
426 |
435 |
443 |
Source: Adapted from Clinical Guidelines on the Identification, Evaluation, and Treatment of Overweight and Obesity in Adults: The Evidence Report.
For specific definition for Asian Indians, please see page 84
Appendix 1
Gestational Diabetes Sample Meal Plan
Sharmila Chatterjee, MSc, MS, RD, CDE
|
Meal/Time |
Meal Plan Number of Food Choices Group |
Menu Ideas for the Vegetarian Indian |
Menu Ideas for the Non-Vegetarian Indian |
|
Breakfast 8am |
1-2 Protein as desired Vegetables 1 Starch as desired Fat |
1 cup paneer jalfrezi with 1 cup bell peppers, onions, 1 roti or chapati |
1 egg omelet 1 cup non starchy vegetables 1 roti or chapati |
|
Snack 11am |
1 Protein 1 Starch as desired Vegetables as desired Fat |
1oz soy nuts ½ cup moong beans sprout |
1 oz string cheese ¾ oz whole wheat crackers |
|
Lunch 1 pm |
3-4 Protein as desired Vegetables 2 Starch 1 Milk as desired Fat |
1 cup of tofu curry 1 cup spinach sabji 2 rotis or chapati ¾ cup non fat yogurt/curd |
1 cup chicken curry 1 cup okra sabji 2 rotis or chapati 1 cup non fat milk |
|
Snack 4 pm |
1 Protein 1 Starch 1 Fruit As desired Fat |
1oz mixed nuts 1 ½ cup puffed rice 1 small mango |
20 small peanuts 1 cup poha (rice flakes) 1 small pear |
|
Dinner 7 pm |
3-4 Protein as desired Vegetables 3 Starch as desired Fat |
1 cup ground soy curry 1 cup cabbage sabji 2 rotis or chapati + ½ cup dhal |
1 cup mutton curry 1 cup cauliflower sabji 3 rotis or chapati |
|
Snack 10 pm |
1 Milk 1 Fruit or Starch 1 Protein |
1 cup non fat milk 1 small apple or 6 saltine crackers 1Tbsp peanut/almond butter |
1 cup plain lassi (no sugar added) 1 ¼ cup strawberries or ¾ oz pretzels ¼ cup cottage cheese |
***Remember to include 8-10 glasses of water throughout each day***
Please consider potato, peas, and corn as starch but not sabji (dry prepared vegetables without gravy/curry)
Adapted with permission from the California Department of Public Health, California Diabetes and Pregnancy Program website: "Asian Indian Food Pyramid for Gestational Diabetes" by Sharmila Chatterjee and Geetha Desai and the California Diabetes and Pregnancy Program, October 2006. Funding for the development of this material was provided by the federal Title V block grant from the California Maternal, Child and Adolescent Health Division.
Appendix 2
Diabetes Numbers At-a-Glance
National Diabetes Education Program (NDEP)

Appendix 3
Diabetes Mellitus Pocket Reference Card
Ritesh Gupta, Anoop Misra, Shashank Joshi, Banshi Saboo, TG Patel
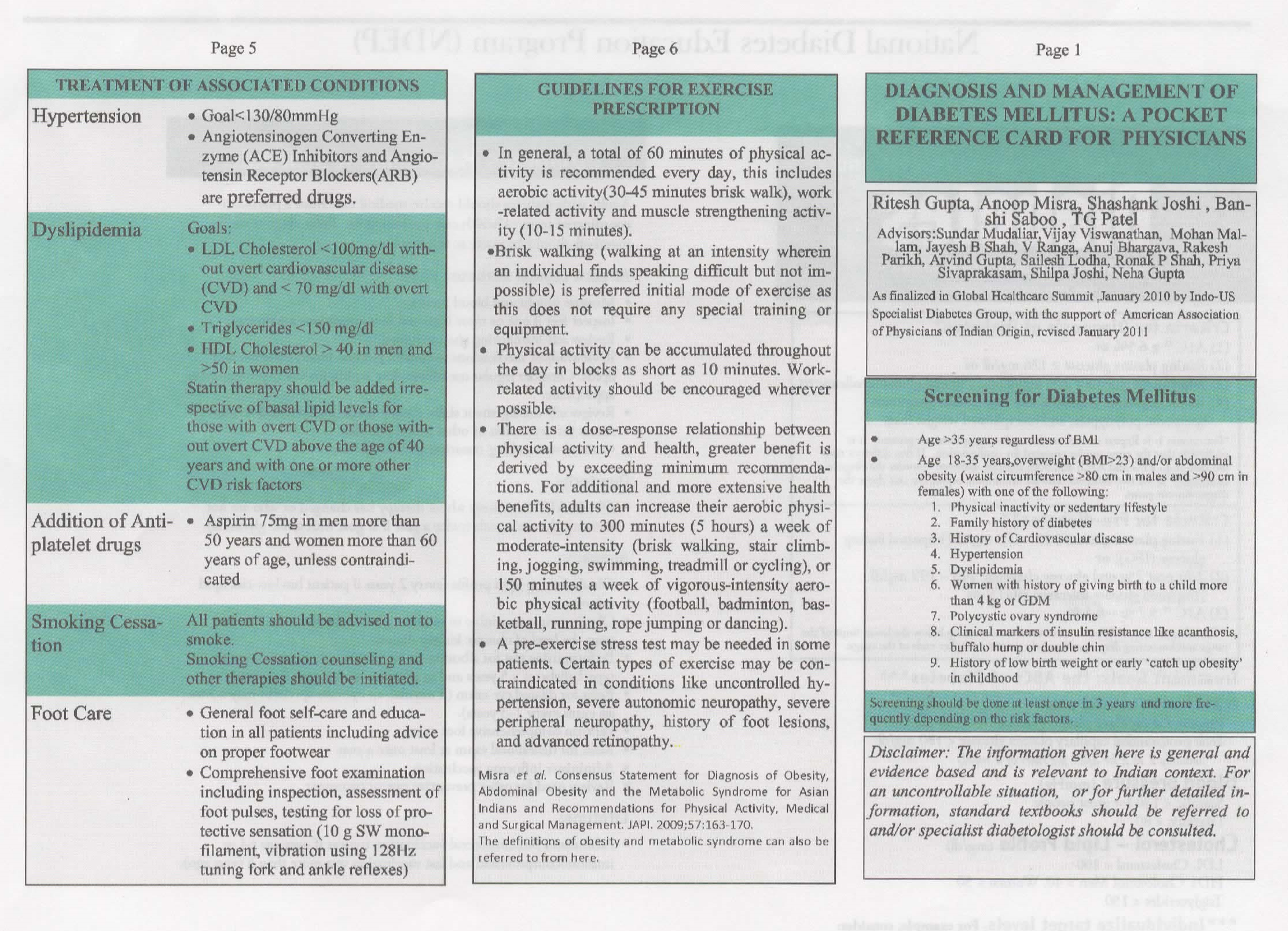

Appendix 4
Clincal Preventive Services for Normal-Risk Adults
Recommended by the U.S. Preventive Services Task Force
|
Test or Disorder |
Population,a Years |
Frequency |
|
Blood pressure, height and weight |
>18 |
Periodically |
|
Cholesterol |
Men > 35 Women > 45 |
Every 5 years Every 5 years |
|
Diabetes |
>45 or earlier, if there are additional risk factors |
Every 3 years |
|
Pap smearb |
Within 3 years of onset of sexual activity or 21-65 |
Every 1-3 years |
|
Chlamydia |
Women 18-25 |
Every 1-2 years |
|
Mammographya |
Women > 40 |
Every 1-2 years |
|
Colorectal cancera |
>50 |
|
|
fecal occult blood and/or |
|
Every year |
|
sigmoidoscopy or |
|
Every 5 years |
|
colonoscopy |
|
Every 10 years |
|
Osteoporosis |
Women > 65; >60 at risk |
Periodically |
|
Abdominal aortic aneurysm (ultrasound) |
Men 65-75 who have ever smoked |
Once |
|
Alcohol use |
>18 |
Periodically |
|
Vision, hearing |
>65 |
Periodically |
|
Adult immunization |
|
|
|
Tetanus-diphtheria (Td) |
>18 |
Every 10 years |
|
Varicella (VZV) |
Susceptibles only, >18 |
Two doses |
|
Measles, mumps, rubella (MMR) |
Women, childbearing age |
One dose |
|
Pneumococcal |
>65 |
One dose |
|
Influenza |
>50 |
Yearly |
|
Human papillomavirus (HPV) |
Up to age 26 |
If not done prior |
|
a) Screening is performed earlier and more frequently when there is a strong family history. Randomized, controlled trials have documented that fecal occult blood testing (FOBT) confers a 15 to 30% reduction in colon cancer mortality. Although randomized trials have not been performed for sigmoidoscopy or colonoscopy, well-designed case-control studies suggest similar or greater efficacy relative to FOBT. b) In the future, Pap smear frequency may be influenced by HPV testing and the HPV vaccine. Note: Prostate-specific antigen (PSA) testing is capable of enhancing the detection of early-stage prostate cancer, but evidence is inconclusive that it improves health |
||
Appendix 5
Glossary
Theja Mahalingaiah, MA, RD & Nirmala Abraham, MS, RD
Alcohol - An ingredient in a variety of beverages, including beer, wine, liqueurs, cordials, and mixed or straight drinks. Pure alcohol itself yields about 7 calories per gram.
Blood Glucose - The main sugar that the body makes from the three elements of food - proteins, fats, and carbohydrates - but mostly from carbohydrates. Glucose is the major source of energy for living cells and is carried to each cell through the bloodstream. However, the cells cannot use glucose without the help of insulin.
Bennecol - A type of plant based margarine that helps lower blood cholesterol level.
Body mass index (BMI) - a method of determining by the relationship between height and weight whether or not a person is obese, overweight, underweight or of normal weight.
Calorie - A unit used to express the heat or energy value of food. Calories come from carbohydrate, protein, fat, and alcohol.
Carbohydrate - One of the three major energy sources in foods. The most common carbohydrates are sugars and starches. Carbohydrates are found in foods from the Milk, Vegetable, Fruit and Starch exchange lists.
Carbohydrate counting – method of meal planning approach for people with diabetes that involves calculating the number of grams of carbohydrate, or choices of carbohydrate, eaten at meals or snacks.
C.D.E. (Certified Diabetes Educator) - A health care professional who is qualified by the American Association of Diabetes Educators to teach people with diabetes how to manage their condition. The health care team for diabetes should include a diabetes educator, preferably a C.D.E.
Cholesterol - A fat-like substance normally found in blood. A high level of cholesterol in the blood has been shown to be a major risk factor for developing heart disease. Dietary cholesterol is found in all and only animal products, but is especially high in egg yolks and organ meats. But saturated fats and oils that can also contribute to heart disease is found in both animal and some plant products. Eating foods high in dietary cholesterol and saturated fat tends to raise the level of blood cholesterol. Foods of plant origin such as fruits, vegetables, grains, and beans, peas, and lentils contain no cholesterol. Cholesterol is found in foods from the Milk, Meat, and Fat exchange lists.
Chronic - Present over a long period of time. Diabetes is an example of chronic disease.
Dietitian - A registered dietitian (RD) is recognized by the medical profession as the primary provider of nutritional care, education, and counseling. The initials RD after a dietitian’s name ensure that he or she has met the standards of The American Dietetic Association. Look for these credentials when you seek advice on nutrition.
Exchange lists - A grouping of foods by type to help people on special diets stay on the diet. Each group lists measured amounts of foods within the group that may be exchanged or traded in planning meals. A single exchange contains approximately equal amounts of carbohydrate, protein, fat, and calories.
Fasting blood glucose test - A method for finding out how much glucose (sugar) is in the blood. The test can show if the person has diabetes. A blood sample is taken in lab or doctor’s office. The test is usually done in the morning before the person has eaten.
Fat - One of the three major energy sources in food. A concentrated source of calories- about 9 calories per gram. Fat is found in foods from the Fat and Meat lists. Some kinds of milk also have fat; some foods from the Starch list also contain fat.
*Saturated fat - Type of fat that tends to raise blood cholesterol levels. It comes primarily from animals and is usually hard at room temperature. Examples of saturated fats are butter, lard, meat fat, solid shortening, palm oil, and coconut oil.
*Polyunsaturated fat - Type of fat this is liquid at room temperature and is found in vegetable oils. Safflower, sunflower, corn, and soybean oils contain the highest amounts of polyunsaturated fats. Polyunsaturated fats, such as corn oil, can help lower high blood cholesterol levels when they are part of a healthful diet.
*Monounsaturated fat - Type of fat that is liquid at room temperature and is found in vegetable oils, such as canola and olive oils. Monounsaturated fats can help lower high blood cholesterol levels when they are part of a lower-fat diet.
Fiber - An indigestible part of certain foods. Fiber is important in the diet as roughage, or bulk. Fiber is found in foods from the Starch, Vegetable, and Fruit exchange lists.
Gestational diabetes mellitus (GDM) - a type of diabetes that develops only during pregnancy and usually disappears upon delivery, but increases the mother’s risk of developing diabetes later in life.
GDM is managed with meal planning, physical activity, and, in some cases, medication.
Gram - a unit of weight in the metric system. An ounce equals 28 grams. In some meal plans for people with diabetes, the suggested amounts of food are given in grams.
Lipid - A term for fat. The body stores fat as energy for future use just like a car that has a reserve fuel tank. When the body needs energy, it can break down the lipids into fatty acids and burn them like glucose (sugar).
Meal Plan - A guide showing the number of food exchanges to use in each meal and snack to control distribution of carbohydrates, proteins, fats, and calories throughout the day.
Mineral - Substance essential in small amounts to build and repair body tissue and/or control functions of the body. Calcium, iron, magnesium, phosphorus, potassium, sodium, and zinc are minerals.
Non calorie sweetener - A man made sweetener that people use in place of sugar because it has no calories.
Ex- Saccharin
Nutrient - Substance in food necessary for life. Carbohydrates, proteins, fats, minerals, vitamins, and water are nutrients.
Obesity - When people have 20 percent (or more) extra body fat for their age, height, sex, and bone structure. Fat works against the action of insulin. Extra body fat is thought to be a risk factor for diabetes.
Protein - One of the three major nutrients in food. Protein provides about 4 calories per gram. Protein is found in foods from the Milk and Meat exchange lists. Smaller amounts of protein are found in foods from the Vegetable and Starch lists.
Sodium - A mineral needed by the body to maintain life, found mainly as a component of salt. Many individuals need to cut down the amount of sodium (and salt) they eat to help control high blood pressure.
Starch - One of the two major types of carbohydrate. Foods consisting mainly of starch come from the Starch list.
Sugars - One of the two major types of carbohydrate. Foods consisting mainly of naturally present sugars are those from the Milk, Vegetables, and Fruit lists. Added sugars include common table sugar and the sugar alcohols (sorbitol, mannitol, etc).
Promise Activa (formerly known as Take control) – A type of plant based margarine that helps lower blood cholesterol level.
Tofu – A protein substitute made with soy beans. Many vegetarian protein alternatives such as Vegetarian burger patties are made with tofu.
Trans fatty acid (also called Trans fat) – comes from adding hydrogen to vegetable oil through a process called hydrogenation. Partially hydrogenated oil is another name for Trans fat. Trans fats are more solid than oil is, making them less likely to spoil. Using Trans fats in the manufacturing of foods helps foods stay fresh longer. Commercially processed goods such as crackers, cookies and cakes, Indian savory snacks and many fried foods, may contain Trans fats. Shortenings (e.g. Vanaspathi commonly used in India) and some margarine can be high in Tran’s fat. Unlike other fats, Trans-fatty acids raise "bad" (LDL) cholesterol and lowers “good" (HDL) cholesterol. A high LDL cholesterol level in combination with a low HDL cholesterol level increases the risk of heart disease, the leading killer of men and women.
Triglycerides - Fats normally present in the blood that are made from food. Gaining too much weight or consuming too much fat. Alcohol, or carbohydrates may increase the blood triglycerides.
Vitamins - Substances found in food, needed in small amounts to assist in body processes and functions. These include vitamins A, D, E, the B- complex, C, and K.
PREPARED INDIAN DISHES
APPETIZERS
- Bhujia - fried lentil snacks.
- Bhel puri - puffed rice mixed with fried snacks and spicy sauce (popular street snack)
- Chiura /Chevda /Chira /Awul - Flattened Rice for Long shelf life / sauteed or fried. Chaat – mixed sweet & savory snack.
- Dahi Vada – Deep fried bean fritters in a yogurt sauce.
- Dhokla –a steamed bread made with fermented chik pea batter.
- Lassi – a yogurt based drink.
- Kachori – Deep fried savory pastry stuffed with lentils.
- Mulligatawny – soup made with lentils and spices.
- Murruku – fried spiral snack.
- Namkeens / Nimki/ Karam - Salty snacks ( spicy at times)–distinct from sweet snacks
- Nimbu paani – a drink similar to lemonade.
- Pakoras – Batter fried vegetables.
- Papad – Baked or fried item that looks like a Large potao chip made with legumes and or rice flour with spices.
- Papad – Baked or fried item that looks like a large potato chip made with legumes and or rice flour with spices.
- Pani puri – mini puri filled with spicy potato & tamarind water ( popular street snack)
- Pav Bhaji - spicy potato served on bread with sauce.
- Puris – Deep fried flat bread made with wheat flour.
- Rasam- Thin soup made with tomatoes, lentils, tamarind (optional) and spices.
- Samosa – Deep fried pastry stuffed with potatoes & other vegetables or meat.
- Sev – Thin fried lentil noodles.
- Vada/ Vadai/Bora – Deep fried savory bean fritters.
BREADS
- Bathura – fried dough made with all purpose flour.
- Chapathi / Phulka / Roti / Rooti – Flat bread made with wheat flour.
- Idli – Stemed dough made of rice and urad dhal (white lentil).
- Nan – Baked (traditionally in clay oven called Tandoor) bread.
- Paratha – a kind of bread made with all purpose flour.
- Roti – a kind of flat bread made with wheat flour.
- Thepla – a flat bread made with wheat flour, gram flour and spices.
- Uppuma – Cooked cream of wheat with onion, spices and oil.
ENTREES
- Biriyani – Rice dish made with vegetables; chicken, meat or shrimp.
- Chicken curry – Chicken in spicy sauce.
- Chole – A dish made with chikpeas, onions, tomatoes and spices.
- Kabab – ground lamb baked, grilled or fried.
- Malai Kofta –Cheese and vegetable balls in special sauce.
- Maccher Jhol – Fish curry.
- Palak paneer – A dish made with spinach, cheese and spices.
- Pullao – Rice dish made with spices & or with vegetables; meat.
- Rogan josh – lamb, goat or chicken dish in spicy sauce.
- Tandoori Chicken – Marinated chicken baked in clay oven.
- Tandoori Fish – Marinated fish baked in clay oven.
- Tikka – boneless marinated meat cooked in spicy sauce.
- Qua gasa – a dish made with dal patty, fried boiled egg and timur.
VEGETABLE DISHES
- Dalma – Dhals cooked with vegetables.
- Dhal – Are cooked legumes. Most common dhals are toor, mung etc.,
- Koottu – diced vegetables cooked with dhal and coconut and added spices.
- Palak paneer – A dish made with spinach, cheese and spices.
- Saag –made with mixedgreens such as spinach, mixed greens etc.,
- Shukto – a vegetable stew.
- Sambar – a vegetable curry made with dhal, vegetables, spices & small amount of oil.
DESSERTS
- Adirasam – deep fried1sweet dish made with rice flour.
- Appam – rice/wheat based preparation.
- Barfies –Look like bar cookies made with ghee, milk, nuts etc.
- Gulab Jamoon – A sweet dish soaked in rose flavored sugar syrup.
- Halwa – a sweet made with milk, sugar, ghee etc.
- Jilebi – Fried dish made with chikpea flour and dipped in sugar syrup.
- Kheers – a dessert made by reducing milk and with other ingredients such as vermicelli, rice, almonds etc.,
- Kulfi –a milk based frozen dessert similar to ice cream.
- Laddu – Ball shaped sweet made with chikpea flour, sugar etc.,
- Mahi: buttermilk which can be sweetened with sugar.
- Misti Doi: sweetened yogurt
- Mithai/Misti – Desserts, Sweets.
- Petha - vegetables preserved in a crystalline sugar medium.
- Payasam – sweet dish made with milk, sugar, rice or dhal.
- Peda – A sweet made with milk, ghee and sugar.
- Rosagolla - cheese based, syrupy sweet dish.
- Rasmalai – sweet made with flattened paneer ball soaked in cream sauce flavored with cardamom.
- Sweet Pongal - sweet tasting cooked rice.
- Payasam – sweet dish made with milk, sugar, rice or dhal.
- Peda – A sweet made with milk, ghee and sugar.
- Pite- Rice flour pancakes immersed in sweetened syrup.
- Rasogolla- Indian cheese balls in sugar syrup
- Sandesh: Indian cheese made with sugar.
- Sweet Pongal - Sweet tasting cooked rice.
MISSELANEOUS
May be sweet , tart or piquant
- Chai – Tea made with milk.
- Chutneys - Are pureed condiments made with coconut, mango, cilantro, mint, Tamarind and spices.
- Pickles- are condiments which may be sweet, tart or piquant that accompany Indian cuisine. Lemon and Mango pickles are common among many varieties of pickles.
- Raita/Pacchadi – A meal accompaniment made with yogurt; grated cucumber, green chilies, onions etc.
|
Measurements and Converstions |
|
1 ounce =30 grams (actual weight 28.35g) 1 fluid ounce =30 millilitres (actual amount 28.35ml) 1 cup = ½ pint = 240 ml = 8 fl ounces 2 cups = 1 pint = 480 ml = 16 fl ounces 2 pints = 1 quart = 960 ml = 32 fl ounces 4 quarts = 1 gallon 1 teaspoon fluid = 5 ml or 1/ 1 tablespoon fluid = 15 ml or ½ oz 1 cup (8 oz) = 16 tablespoons 1 kilogram = 2.2045 pounds (2.2 lb) 1 liter = 1.0567 quarts 1 pound = 453.6 grams |
|
6 oz |
|
To change pounds to kilograms, multiply by |
Guide to Ingredients
- All-purpose flour – Maida
- Aniseed – Ajowain or Carum
- Asafoetida – Hing
- Aubergine – Baingan (egg plant)
- Basmati rice – a kind of aromatic rice
- Bay leaf – Tej patta
- Beets – Chukandar
- Besan flour – chikpea flour
- Bottle gourd - Lauki
- Broad beans – Papdi
- Bitter gourd - Karela
- Cauliflower - gobi
- Cluster beans - Papdi
- Bitter gourd – Karela
- Black pepper – Kali mirchi
- Cardamom – Elaichi
- Chilies – Mirchi
- Cinnmon – Dalchini
- Cloves – Lavang
- Coconut – Nariyal
- Coriander seeds – Dhaniya
- Cumin – Jeera
- Curry leaves – Kari patta
- Dill – suva bhaji
- Drumsticks – Surgavo
- Eggplant - Brinjal
- Fennel – Saunf
- Fenugreek – Methi seeds
- Fenugreek leaves – Methi leaves
- Fresh coriander - Cilantro
- Garam Masala – Indian spice blend
- Garlic – Lasoon
- Ghee – Clarified butter
- Ginger – Adrak
- Gram flour – Besan or chik pea flour
- Spine gourd -Kankoda
- Jaggery – Gur
- Mace – Javitri
- Malai - Cream
- Mango powder – Amchoor
- Mint – Hara pudeena
- Mustard – Sarasoon or Rai
- Nut meg – Jaiphal
- Onion seeds – Kalonji
- Oregano seeds – Ajwain
- Sambal oelek – Chilli paste
- Palak – Spinach
- Paanch phhotan/phhotan –five seed seasoning mix of mustard, nigella, fenugreek, fennel & wild celery
- Parsley – Ajmood ka patta
- Paneer – Indian cheese
- Pink beans - Valore
- Pomogranate seeds – Anardana
- Poppy seeds – Khus Khus
- Puffed rice : Mamra, Moori , Pori
- Raisin – Kismish
- Red lentils – Masoor Dhal
- Ridge gourd – Torai or Turia
- Saffron – Kesar
- Semolina – Sooji
- Sesame seeds – Til
- Tamarind – Imli
- Toor Dhal – Yellow split peas
- Turmeric – haldi
- Urad Dhal – Split black gram
- Vinegar – Sirka
- Whole Wheat Flour – Atta
- Yellow split peas – Channa dhal
- Yogurt – Dhahi
Theja Mahalingaiah, MA, RD is a clinical dietitian at Southbury Training School Southbury Connecticut. Contact information theja305@yahoo.com
Nirmala Abraham MS, RD is from Delaware. Contact information 302-239-7119 or ocnirmala@aol.com
Appendix 6
Diabetes Information in English and Regional languages
Padmini Balagopal, PhD, RD, CDE, IBCLC
What Can I Eat To Manage My Diabetes?
Information & Guidelines on the Asian-Indian Cuisine
- Diabetes is a condition where your body is not able to make enough insulin or where the insulin not being used properly. Insulin enables your body to get energy from glucose – the sugar broken down from the foods you eat. An imbalance between insulin and blood glucose levels can result in high glucose (hyperglycemia) or low blood glucose (hypoglycemia) levels in your blood.
- Maintaining blood glucose levels in established target range levels is important and research has shown that it can help prevent complications in your eyes, kidneys, blood vessels and more.
- Under your physician’s guidance, diabetes and blood glucose levels are managed with Medical Nutrition Therapy, and an Individualized mean plan (see page 4), an exercise routine and medications as needed.
- The foods your eat, your total caloric intake, physical activity and body weight are some of the factors that can affect blood glucose levels. Foods that contain carbohydrates can raise blood glucose levels. Fats and protein can also affect weight, if eaten in excess.
- Keep a daily log of your meals, snacks and blood glucose levels to better understand the effect of food on blood glucose.
- Include a daily exercise plan approved by your doctor, into your regimen.
- Learn to understand nutrition facts labels and ingredients listed on the product label. Your Registered Dietitian can help you with this.
Methods of preparing and cooking food
- Sprouting legumes increases nutritional value. It can be fun sprouting different legumes!
- Steam vegetables with little water. Do not drain the cooking water from rice and vegetables.
- Limit or avoid highly processed foods or high‐fat, salty “fast” foods.
- Try to eat small, frequent balanced meals at regular times.
Drink plenty of water
- 6‐8 glasses (8 oz each) are the usually recommended amount. Plain water is the best.
- Avoid excessive use of caffeinated drinks like coffee, tea and caffeine containing drinks.
- Use alcohol only after talking to your physician.
Some other factors that can affect health
- Include at least 20 grams of fiber every day. Whole grains, beans & fruits/veg. are rich sources.
- Many ‘fast’ foods are high in fat, salt and/or sugar. Limit or avoid frequent use of such foods.
- If you have high blood pressure, restrict the use of salt, foods high in salt like regular chips and pickles.
- Talk to your physician about your multi‐vitamin and multi‐mineral or other dietary supplements.
- Have a physical routine check‐up with the American Diabetes Association‘s Standards of Care for Diabetes as a guide.
- Know your ABCs of diabetes (A1C, blood pressure and cholesterol numbers).
DIABETES CAN BE MANAGED! TAKE CONTROL! YOU CAN DO IT!!
Diabetes Information in English and Regional languages
What Can I Eat To Manage My Diabetes?
Information & Guidelines on the Asian-Indian Cuisine
[To be used with the guidance of your physician and Registered Dietitian]
Name :
Calories/Day :
Your BMI:
Today’s Date :
Present Weight :
Your waist circumference :
Foods from a variety of sources can be combined to make up a balanced meal. Your personal meal plan should be designed to suit your lifestyle and would include servings of each food group at every meal. Each food group and examples of one serving in each food group are as follows: (Please note that values are approximate).
1.GRAINS/BEANS/STARCHY VEGETABLES (without added fats or oils)
[1 serving provides about 15 gms CHO, 3 gms protein and 80 calories]
Bread : 1 slice
Avial : ½ cup
Popcorn : 3 cups
Sambar : ½ cup
Cooked noodles/sooji : ½ cup
Rice Flour : 2 Tbsp
Wheat Flour: 2 ½ Tbsp
Sookhi roti : 1‐6” wide
Wheat, Corn, Oats, Potato : ½ c. (ckd)
Green Plaintain/Peas : ½ cup
Rice : 1/ cup (ckd)
Poha : ½ cup
Dhals/Beans/Legumes : ½ cup (100 cal.+ 7 gms protein)
Idli : 1
Naan : ¼ - 8” x 2”
2. MEAT & MEAT ALTERNTIVES – LEAN
[1 serving provides 7 gms protein, 0‐3 gms fat and 45 calories]
|
Chicken, turkey (skinless white meat) |
: |
1 oz |
|
Tuna in water, flounder |
: |
1 oz |
|
Low‐fat cheese |
: |
1 oz |
|
Egg whites only |
: |
2 |
|
Dhal* (*also supplies 15 gms CHO and 100 calories approximately) |
: |
½ cup (cooked) |
|
Shrimp (Prawns) |
: |
1oz |
|
Low‐fat Tofu |
: |
3 oz |
|
Chicken, turkey (skinless dark meat) |
: |
1 oz |
|
Seitan |
: |
1 oz |
|
Lean lamb, pork, beef |
: |
1 oz |
|
Regular cottage cheese |
: |
¼ cup |
|
Cheeses with 3 gm fat or less |
: |
1 oz |
MEAT & MEAT ALTERNATIVES – MEDIUM FAT
[1 serving provides 7 gms protein, 5 gms fat and 75 calories]
|
Egg |
: 1 |
|
Fried fish product |
: 1 oz |
|
Ricotta cheese |
: ¼ cup |
|
Lamb (rib roast, ground) |
: 1 oz |
|
Tofu |
: 3.5 oz |
|
Tempeh |
: ¼ cup |
MEAT & MEAT ALTERNATIVES – HIGH FAT
[1 serving provides 7 gms protein, 8+ gms fat and 100+ calories]
|
Regular cheese |
: |
1 oz |
|
Chicken/turkey hot dog |
: |
1 (10/lb) |
|
Peanut butter |
: |
1 oz (+ 1 fat exchange) |
|
Sausage |
: |
1 oz |
|
Paneer |
: |
1 oz |
3. VEGETABLE (no fat added)
[1 serving provides 5 gms CHO and 2 gms protein and 25 calories]
|
Greens |
: |
Fenugreek (methi) leaves ½ cup. |
|
Green beans |
: |
½ cup |
|
Cabbage Cauliflower |
: |
½ cup |
|
Gourds |
: |
½ cups |
|
Brinjal (eggplant) |
: |
½ cup |
|
Capsicum |
: |
½ cup |
|
Salad |
: |
1 cup |
|
Drumstick, okra |
: |
½ cup |
|
Tomato |
: |
½ cup |
|
White radish, chow‐chow |
: |
½ cup |
4. FRUITS (Serving size varies)
[1 serving provides 15 gms CHO 60 calories]
|
Banana |
: |
½ cup |
|
Apple, Orange |
: |
1 (small) |
|
Large Pear |
: |
½ |
|
Melons |
: |
1 cup |
|
Mango |
: |
½ cup |
|
Fresh guava |
: |
½ cup |
|
Canned fruit |
: |
½ small |
5. MILK AND MILK PRODUCTS
[1 serving provides 12 gms CHO, 8 gms protein; 0-8 gms fat; 100‐160 calories]
|
Whole/skimmed/low fat milk |
: |
1 cup |
|
Buttermilk /Yoghurt/curds (tones or whole) |
: |
1 cup |
|
Paneer |
: |
1 oz |
6. FATS and OILS
[1 serving provides 5 gms of fat and 45 calories]
|
Cooking oil |
: |
1 Tsp. |
|
Coconut, grated |
: |
2 Tbsp. |
|
Nuts or seeds |
: |
1 Tbsp. |
|
Margarine |
: |
1 Tsp. |
- The use of unsaturated oils like olive oil instead of saturated fats like butter, coconut products and ghee is recommended. Avoid frequent use of fried foods.
- Minimal use of oils, salt and sugar is recommended.
Adapted from Choose your foods: Exchange Lists for Diabetes
by American Dietetic Association and American Diabetes Association (2008:Page 4)
Diabetes Information in English and Regional languages
What Can I Eat To Manage My Diabetes?
Information and Guidelines to eat on the Asian‐Indian Cuisine
A sample of an Individualized Meal Plan that be completed by
Your Physician and Registered Dietitian
Yoga/Exercise :
Other scheduled activities:
Time:
Time:
|
Meal/Food Group |
Servings |
CHO* (gms) |
Protein (gms) |
Fat (gms) |
Calories |
|
Breakfast |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
Mid-morning |
|
|
|
|
|
|
|
|
|
|
|
|
|
Lunch |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
Mid-Afternoon |
|
|
|
|
|
|
|
|
|
|
|
|
|
Dinner |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
Night Snack |
|
|
|
|
|
|
|
|
|
|
|
|
|
Total |
|
|
|
|
|
*CHO = Carbohydrate; gms = Grams; oz = ounce; tsp = teaspoon; Tbsp = Tablespoon;
28‐30gms = 1 oz; 8 oz = 1 cup; 3 tsp = 1 Tbsp; 2 Tbsp = 1 oz; ckd = cooked.
Author:
Padmini Balagopal, PhD, RD, CDE
Reviewed by:
Wahida Karmally, DrPH, RD, CDE, CLS, FNLA
Karmeen Kulkarni, MS, RD, BC-ADM, CDE
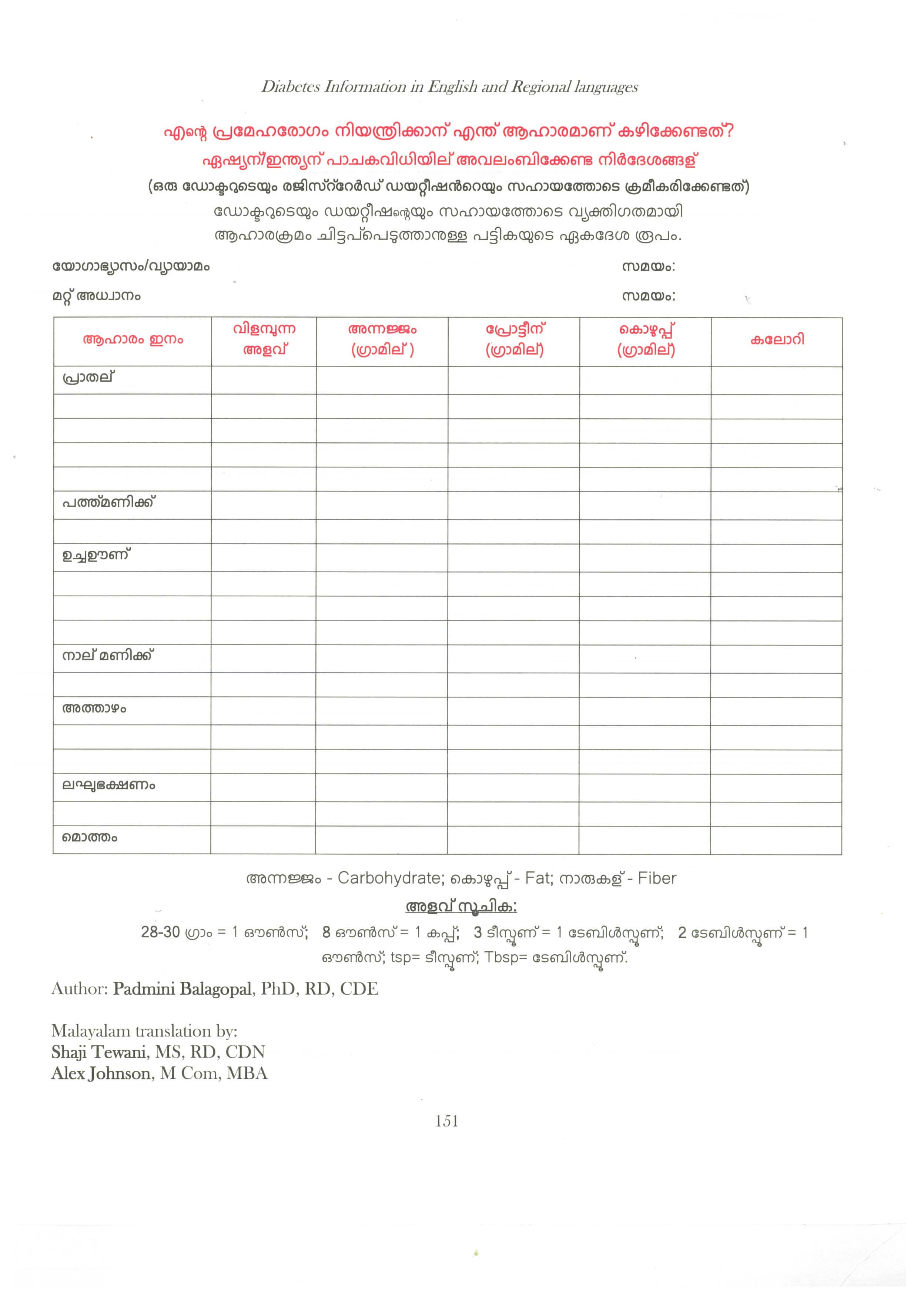
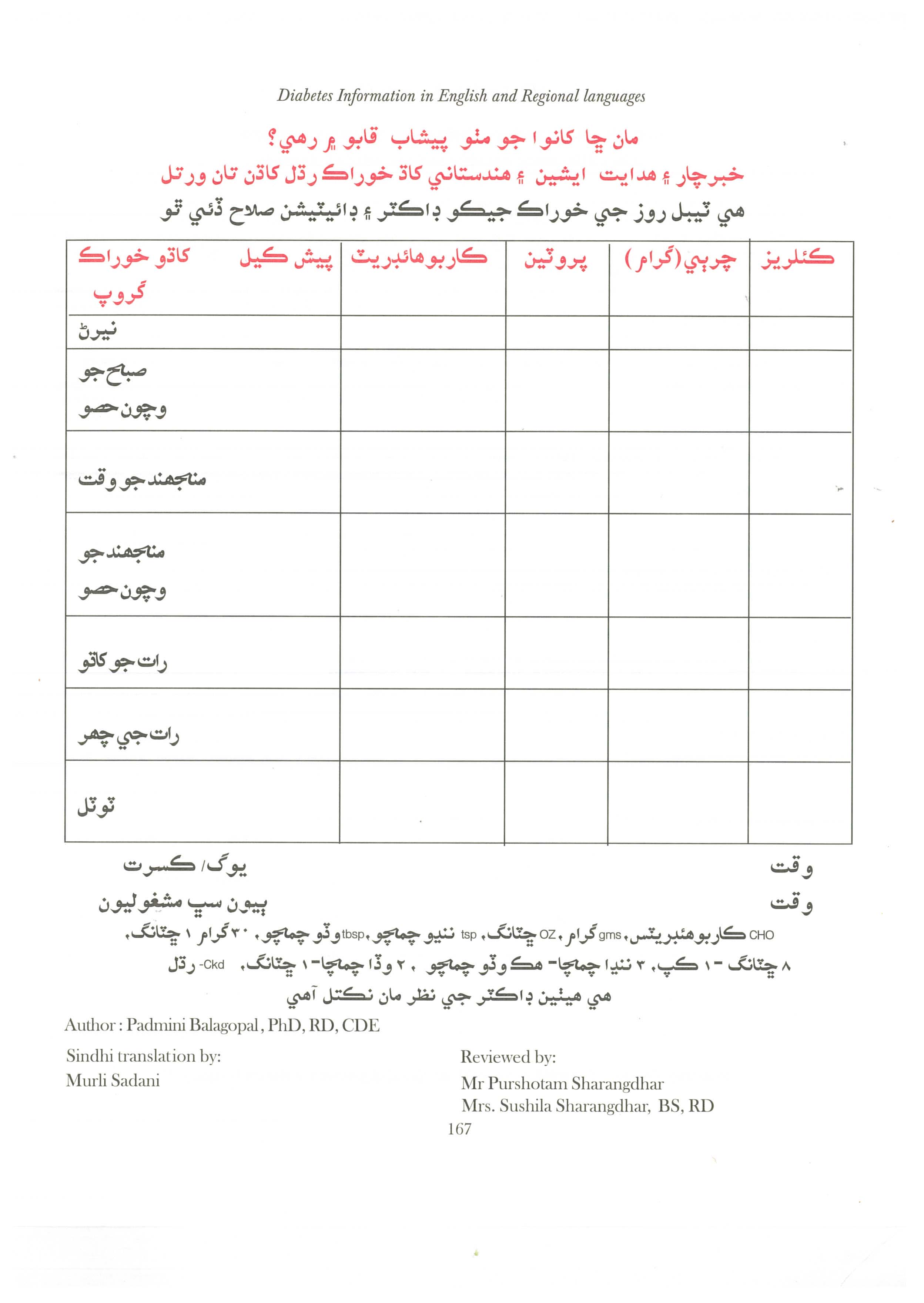







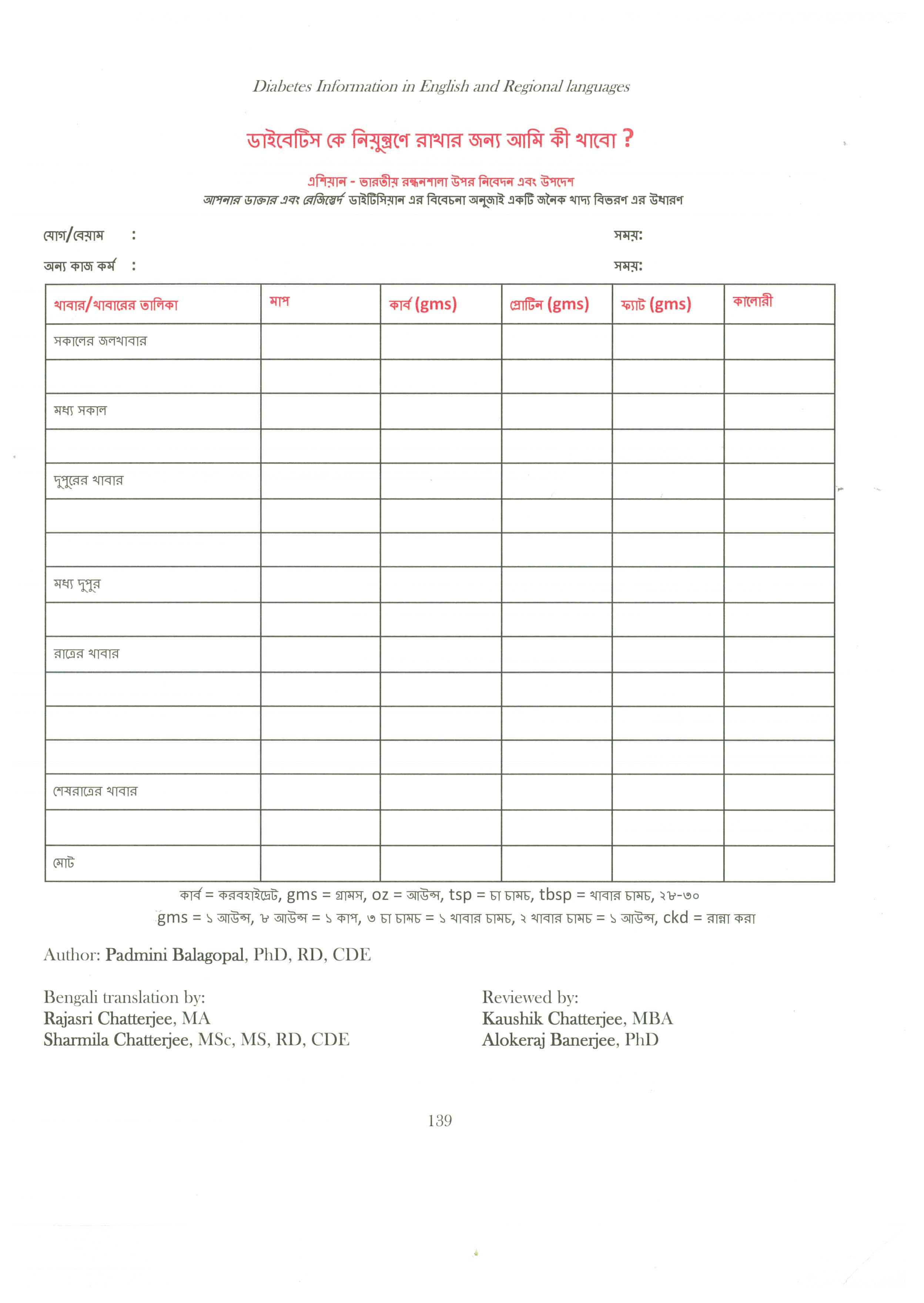




































 - Indian Foods: AAPI’s Guide To Nutrition, Health and Diabetes
- Indian Foods: AAPI’s Guide To Nutrition, Health and Diabetes